What immunity did having COVID-19 give me? Do I still need a vaccine?
Is the immune response robust enough that those who’ve had COVID can avoid getting vaccinated? Many people asked WHYY’s Health Desk Help Desk.
Listen 4:53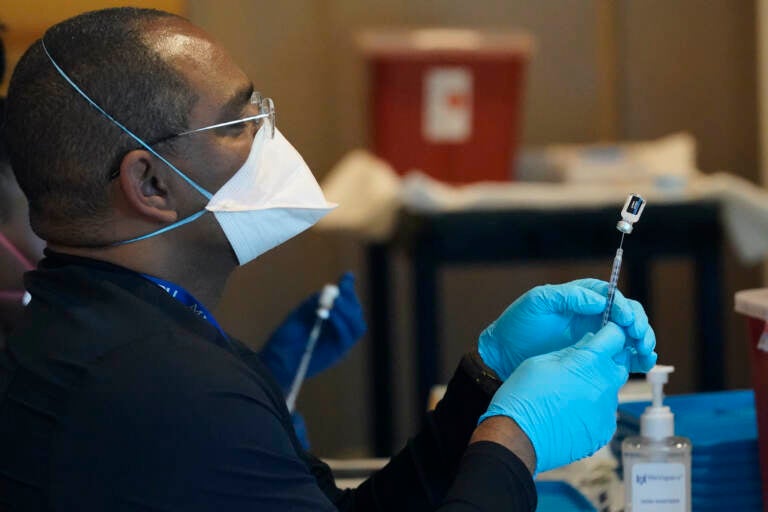
A health care worker fills a syringe with the COVID-19 vaccine. (AP Photo/Wilfredo Lee)
This is one of a series of articles in which reporters from WHYY’s Health Desk Help Desk answer questions about vaccines and COVID-19 submitted by you, our audience.
Ask us about COVID-19: What questions do you have about the coronavirus and vaccines?
After getting a fever, Margaret Grafenstine tested positive for the coronavirus in November, then developed a cough, a sore throat, and a slight numbness in her hands.
Grafenstine, 58, who lives in Trevose, Bucks County, said it took about two weeks for her to feel like herself again.
A test later confirmed Grafenstine had a robust antibody response to the infection and she even donated convalescent plasma. Now, she’s trying to decide whether to get vaccinated.
“If a person has already tested positive for COVID, why are the antibodies in that person’s system from actually having the virus not good enough?” she asked WHYY’s Health Desk Help Desk. “I just don’t understand why it’s necessary … I have a bit of a fear with the vaccine, just as I do with the virus, truthfully.”
Many other WHYY listeners and readers — including people who have never had COVID-19 — submitted questions asking whether people who have had infections develop a robust enough immune response to avoid getting vaccinated.
Here’s what the experts are saying, as the delta variant of the virus boosts case numbers in the region and nationwide.
Does a coronavirus infection provide protective immunity?
An infection causes the immune system to respond to and recognize the coronavirus. After getting the virus, most people have detectable antibodies, health experts say. Though other arms of the immune system might become involved, studies so far suggest that the key to fighting the virus correlates with the production of antibodies.
Though protection is decent for those who have previously had COVID-19, health experts say it is not as strong as when people get vaccinated.
“So that’s why there is that recommendation that despite having had COVID before, for full protection the vaccination is the best way to go,” said Dr. Lisa Maragakis, senior director for infection prevention at Johns Hopkins.
A prior infection offers protection in the range of 80%, compared to about 95% for the Moderna and Pfizer vaccines, said Dr. John Wherry, director of the Institute for Immunology at the Perelman School of Medicine at the University of Pennsylvania. That means about 15 to 20 out of every 100 people who have previously had COVID-19 could get reinfected, while 5 out of every 100 people who got an mRNA vaccine might get infected.
People with more severe infections appear to have stronger antibody responses than those who had milder or asymptomatic infections, Maragakis said. In addition, she said, the status of a person’s immune system can also dictate the quantity of antibodies and the quality of their antibody response. For example, immunosuppressed people might not mount an antibody response after being infected with COVID-19 or after getting vaccinated.
Lab studies suggest that protection following a case of COVID-19 begins to wane slightly after about three months, but can last for up to 10 months, although there’s a range to that, Wherry said.
“We see some people with mild COVID infections where their immunity wanes more quickly over time, or they don’t have as much coverage, and that is protection from variants. And we see people who have mild COVID that have lower levels of antibodies than you would get from vaccination,” Wherry said. “So there’s a wider range and it’s difficult to know where you are on that range from natural infection.”
Scientists still don’t know as much about the durability of immunity as they would like, he said. What they expect based on coronaviruses that existed prior to SARS-CoV-2 is that antibodies decline over time.
If I had COVID-19, should I take an antibody test?
It’s a good idea, Wherry said, but whether it’s practical is a different question.
“I think it’s useful to know whether or not you have antibodies, and that may be helpful in knowing whether your protection goes away,” he said. “I think a lot of institutions and businesses are thinking about whether or not to mandate vaccination. And if they do, will they use a documented previous COVID infection as evidence of being immune? So this is an important question.”
“Most people that previously had COVID will be protected. We don’t know for how long,” Wherry said. “Would it be valuable to check antibodies over time to know whether those antibodies have disappeared and use that as perhaps an indicator that now it’s time to get vaccinated? All really good questions. How you implement them in different settings, or even more broadly, from a public health standpoint, I think has to be factored in. It will be challenging to do so right now.”
There also are different kinds of antibody tests available, and they can be somewhat tricky to interpret because there are different ways of looking for the antibodies, Maragakis said.
“I would say right now there’s not a lot of reason for someone to go and get an antibody test unless you’re just curious,” she said. “I mean, that’s one reason, to see if you’ve been exposed in the past. But the recommendation is to get vaccinated, even if you’ve had a prior infection with COVID-19, because of that more robust, higher level of antibody response that most people get with vaccination as opposed to natural infection.”
How does getting one variant protect me from another?
When your immune system responds to one virus, it provides some degree of protection against similar viruses, Maragakis said. But the more different the viruses are, the more likely your immune system might not be able to recognize them, she said, and that’s why health experts are concerned about variants.
Studies show that the currently available COVID vaccines are effective against the current COVID variants.
A study published in July in the New England Journal of Medicine found that two doses of the Pfizer vaccine was 88% effective at preventing symptomatic disease from the delta variant, compared to about 95% for the original virus strain. Data from Israel estimated lower effectiveness against symptomatic disease, but said that the protection against severe illness remains high.
The concern, though, is that “the more the virus is allowed to circulate, the more variants may emerge and we may see a time that a variant escapes the currently available vaccine. And at that point, we would have to modify the vaccines and re-vaccinate people against the new variant,” Maragakis said.
Researchers can study the effectiveness of a previous infection against variants by taking antibodies from people who have had COVID-19 and testing their ability to neutralize the different variants in the laboratory.
Antibodies generated from natural infection and vaccination do respond to the delta variant reasonably well. It’s actually the beta variant, first identified in late 2020 in South Africa, that antibodies have had trouble neutralizing, Wherry said. The concern about the delta variant, though, is that the amount of virus that gets transmitted is much higher, making it more infectious.
“So let’s say that you needed a certain amount of antibodies to prevent a thousand viral particles from starting to infect your upper respiratory tract. So you’d be protected if all that’s been transmitted is a thousand particles,” Wherry said. “With the delta variant, we know that people are harboring a thousand-fold higher amounts of virus in their nasal passages when they get infected. So now you might be not transmitting a thousand viral particles, but actually a million viral particles, and you can overwhelm the antibody responses there.
“And so what that means,” Wherry added, “is that even if you’ve had the vaccine, even if you previously had COVID, even if you’re hearing that the vaccines are still working against delta, we need to be careful because delta is actually giving off more viral particles, meaning that all of us may still be, to some extent, a little bit susceptible.”
How long should I wait to get the vaccine after having COVID-19?
Right after an infection, the body’s immune response is at its peak, so it makes sense to wait several weeks before getting vaccinated, Maragakis said. She suggests about six weeks, or even up to 90 days. But you shouldn’t wait much longer than that, she said.
“We also know that immunity does wane after a natural infection, and people sometimes do get reinfected. And so it’s really a matter of waiting for several weeks, but not too long to get the vaccine,” Maragakis said.
Wherry said people who have had COVID-19 should consult with their physicians and make sure their symptoms have completely resolved. Getting a vaccine too soon could dampen its effectiveness, the experts said.
Right after getting COVID-19, the immune system is activated, and it responds to the viral pathogen and spike protein. If the person gets vaccinated too soon, the vaccine-mediated spike protein might get “lost” in the rest of the pathogen-mediated immune response, and fail to provide any additional boost to the immune response, Paragakis explained.
“We believe that giving the vaccination at least six weeks after acute infection gives the best chance for the vaccine to act as a ‘reminder’ to boost and stimulate a stronger and more durable immune response,” she said.
What are the health risks of getting the vaccine after an infection?
By and large, the COVID-19 vaccines are very safe.
There have been some exceedingly rare adverse events, including blood clots and myocarditis. But for most of those cases, the patients recovered quickly and showed no evidence of long-term consequences.
Wherry said most of the people who had the rare blood clots and allergic reactions did not previously have COVID-19.
“So the risk seems to be at least a little bit lower — why that is, I’m not sure. It may just be statistics, that we don’t have as many previous COVID people getting vaccinated,” he said.
If you get the vaccine too close to a COVID-19 infection, an inflammatory response might be provoked that would make you feel pretty sick again. That’s considered a side effect — not an adverse event, Wherry said. Though people with no previous COVID infections typically get stronger side effects after the second dose of a vaccine, people who have had previous infections often get side effects after the first dose.
What if I become infected between two vaccine doses?
The recommendation is to complete the series of vaccinations, but to wait until you are fully recovered from COVID-19 before getting your second dose.
If I had COVID-19, should I get one mRNA dose instead of two?
There have been a number of studies that suggest that if you previously had COVID-19, getting just one dose of an mRNA vaccine is sufficient to boost your immunity levels up to the maximum level, or the level that’s achieved following two doses among people who have never had COVID-19.
But those studies are still in the early stages, and the Centers for Disease Control and Prevention still recommends that people with previous infections get two doses.
If I’ve had COVID, what are the vaccination pros and cons?
Wherry said you could get stronger side effects from the vaccine than other people, but that this is not something to be afraid of. For about 24 hours, you might experience symptoms similar to those COVID-19, he said.
On the flip side, some people with long COVID issues have reported some of the symptoms disappearing after they got the shot.
People with previous COVID-19 who get vaccinated also have a greater immune response than they did before.
“Studies have shown us that the immune response is more vigorous, you have higher levels of antibodies, and more neutralizing antibodies that stay around for a longer period of time after vaccination as opposed to natural infection,” Maragakis said.
Most importantly, getting vaccinated will provide better protection against variants.
“We also have the variants that are now circulating and are clearly causing second infections in those who have had the infection before, and even in some cases, breakthrough infections for people who are vaccinated,” Maragakis said. “So to give yourself the best chance to fight off the virus, vaccination is definitely the answer.”

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.




![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)