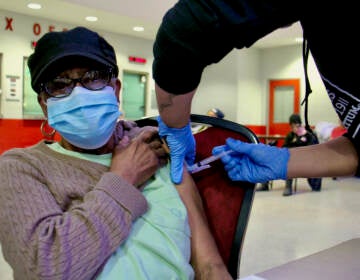
Should I get an omicron booster shot? Delaware Valley experts share what you need to know
New COVID-19 booster vaccines are making their debut this fall, and they’ll be available to most adults.
Listen 3:12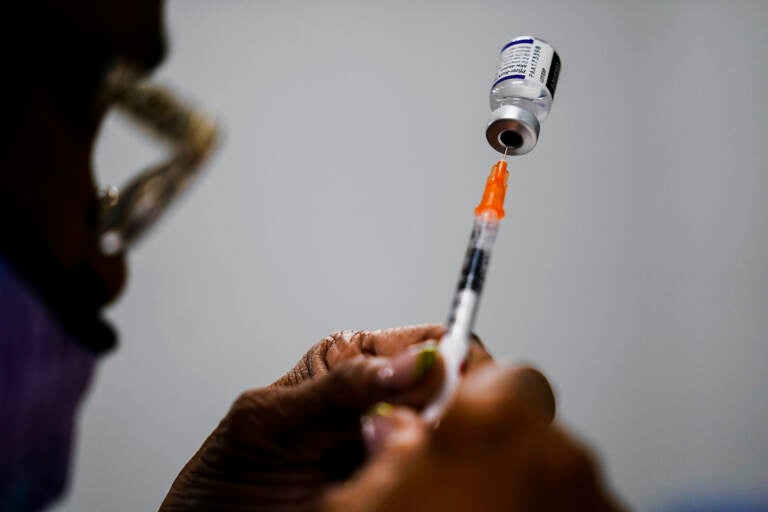
A syringe is prepared with the Pfizer COVID-19 vaccine at a vaccination clinic at the Keystone First Wellness Center in Chester, Pa., Dec. 15, 2021. (AP Photo/Matt Rourke, File)
This is one of a series of articles in which reporters from WHYY’s Health Desk Help Desk answer questions about vaccines and COVID-19 submitted by you, our audience.
New COVID-19 booster vaccines are making their debut this fall, and they’ve been modified to target specific omicron variants that are causing the majority of new cases in the United States.
The boosters — made by Pfizer and Moderna — won approval from the U.S. Food and Drug Administration last week. The Centers for Disease Control and Prevention followed by granting the vaccines emergency use authorization Thursday.
The CDC and health experts in the Delaware Valley region providers say the new doses could be available as early as this week at local health offices and pharmacies.
“I think the goal here is to give everybody the vaccine that better matches what’s circulating in the population in order to not only protect against severe disease and death, but also reduce infection,” said Dr. Thersa Sweet, an epidemiologist at Drexel’s Dornsife School of Public Health.
How are these boosters different from the original vaccines?
The updated vaccines are not much different from the original COVID-19 shots, Sweet said. Both Pfizer and Moderna continue to use mRNA technology.
The original doses, which will still be used for primary vaccination series, are monovalent, meaning they contain a component for just the original strain of SARS-CoV-2.
The new booster doses are bivalent vaccines, which means, in addition to the original strain, they contain a second component for the omicron subvariants BA.4 and BA.5.
“We know that these variants are highly contagious,” Sweet said. “They’re much more contagious than the original strain that circulated two and a half years ago. So, for those of us that have been vaccinated with the original strain, we definitely still have protection against severe disease and death, but our protection against infection is limited.”
This was the first time the FDA authorized COVID-19 vaccines without requiring them to be tested in humans. Instead, experts on federal advisory committees reviewed data from trials in mice, as well as human data on how a booster targeting a different variant — BA.1 — fared.
Dr. Marci Drees, chief infection prevention officer and hospital epidemiologist for ChristianaCare, said vaccine makers had to consider safety and efficacy of the vaccines, as well as the rapid changes in new variants.
“It’s about a balance. Do you want to wait until, say, November when they have human data? And they actually did some modeling that suggested that if we did that, we’d see over 100,000 more hospitalizations and some 10,000 more deaths,” Drees said.
“Or, do we try to get them [boosters] out sooner to really prevent that wave from having such an impact?” she added. “And the FDA … they felt very comfortable [saying] ‘let’s protect people against what’s circulating now, and we feel that it’s a safe approach.’”
In a White House briefing Tuesday, Dr. Anthony Fauci said the country is likely moving towards a vaccine program similar to influenza, “with annual, updated COVID-19 shots matched to the currently circulating strains for most of the population.”
Who is recommended and eligible to get a bivalent vaccine dose?
The bivalent booster doses are for people who’ve already completed a primary series of COVID-19 vaccination, either a two-dose regimen by Pfizer, Moderna or Novavax, or the single shot of Johnson & Johnson.
Age eligibility for the updated boosters depends on the vaccine manufacturer. People 12 years and older can get a Pfizer booster, while the Moderna doses are cleared for people 18 years and older.
While the bivalent boosters are cleared for a large swath of the population, Dr. Paul Offit said the focus should really be on people who remain most at risk of becoming severely ill and hospitalized.
This includes older residents, people with chronic health conditions, and those who are immunocompromised.
Offit is an infectious disease physician, director of the Vaccine Education Center at Children’s Hospital of Philadelphia, and a voting member of the FDA’s Vaccines and Related Biological Products Advisory Committee.
“The group that in many ways is most at risk of being hospitalized or dying are those over 75 years of age, who are a highly vaccinated group,” he said. “But the fact is, as you get older, your immune system also gets older and is less capable of responding. So, they might benefit from that boost as compared to a younger population.”
What if I recently tested positive for COVID-19, or just got a monovalent vaccine dose?
The CDC recommends that people wait at least two months after a recent coronavirus vaccine dose before getting a bivalent booster, and three months after a COVID-19 infection.
However, some vaccine experts like Offit suggest waiting even longer, from four to six months after someone’s last exposure to the virus or a previous COVID-19 vaccine dose.
“If you’ve been naturally infected or [recently] vaccinated, you’ll develop this vigorous antibody response,” Offit said. “So, if you give the [bivalent] vaccine too soon, it really sort of neutralizes the effect of the vaccine. You don’t really get the boost that you want.”
When and where can I get a bivalent booster shot?
Drees said there’s no reason to delay getting a booster dose when someone becomes eligible. States and cities were able to pre-order doses last month in anticipation of federal authorization.
Philadelphia ordered 30,000 Pfizer bivalent booster doses and 11,000 from Moderna. Department of Public Health officials say they’re expecting vaccine deliveries this week. Local providers can request their individual vaccine supplies through Philavax.
Officials at the Pennsylvania Department of Health said they’re expecting 215,000 doses of Pfizer and 83,000 of Moderna from pre-ordering to be distributed to providers throughout the state.
The New Jersey Department of Health stated that 234,200 doses of the new boosters had been allocated to the state, and as of Aug. 30, orders had been placed for 88,500 doses.
In Delaware, health officials said the state had pre-ordered 4,200 doses of Moderna and 8,700 of Pfizer as of Aug. 25.
What other vaccinations can I get this fall?
The fresh wave of COVID-19 boosters is coming at a time of year when other diseases like influenza tend to circulate.
In addition to becoming up to date with COVID-19 vaccines, health experts recommend that everyone 6 months and older get a flu shot this year.
“I always tell people to try to time their flu shots in late September or early October just to give that kind of maximal protection to what’s hopefully the height of flu season,” Drees said.
It’s safe and effective for people to get a flu shot and a COVID-19 vaccine or booster at the same time, according to CDC guidelines.
Drees added that because flu and COVID-19 vaccines do not contain live virus, there’s usually no immune system interferences.
Flu activity during the pandemic so far has generally been mild, likely as a result of pandemic precautions and isolation. However, many experts are predicting a harsher season this year as pandemic precautions drop off and people get together.
“It’s going to start getting cold, we’ve got students going back to school, people are going to be crammed inside buildings,” Sweet added, “and so, we’re all going to be sharing the same air.”
Routine childhood vaccinations, which are often a requirement for children to attend school, should also be a priority, Sweet said. An infection from a disease like measles, which can be prevented with an MMR vaccine, can be dangerous, she added.
“We know that measles infection produces a profound immunosuppression afterwards,” Sweet said. “So, if your child gets infected with measles, down the road they’re going to be immunosuppressed, and they could pick up some other bug — a diarrheal disease or flu — and they could get really, really sick.”
While many vaccines can be given at the same time, Drees said there may be some special considerations for people who get a monkeypox vaccine, which does contain live virus.
“If you just got a COVID vaccine and now you’ve been exposed to monkeypox and need the monkeypox vaccine, then certainly go ahead and get it to protect yourself,” she said. “But otherwise, you should try to space those out if you can.”
The CDC suggests that people wait about four weeks from their monkeypox vaccine before getting a COVID-19 booster dose.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.





![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)