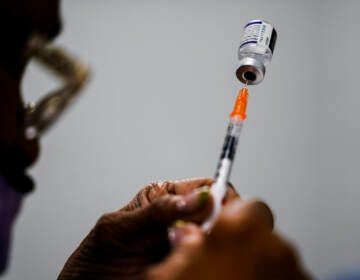
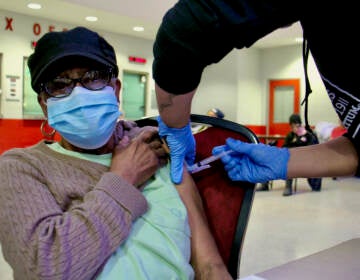
What will a COVID vaccine booster do? How do we know the timing is right?
As the federal government plans COVID-19 booster shots to strengthen waning immunity, WHYY’s Health Desk Help Desk shares what you need to know.
Listen 5:33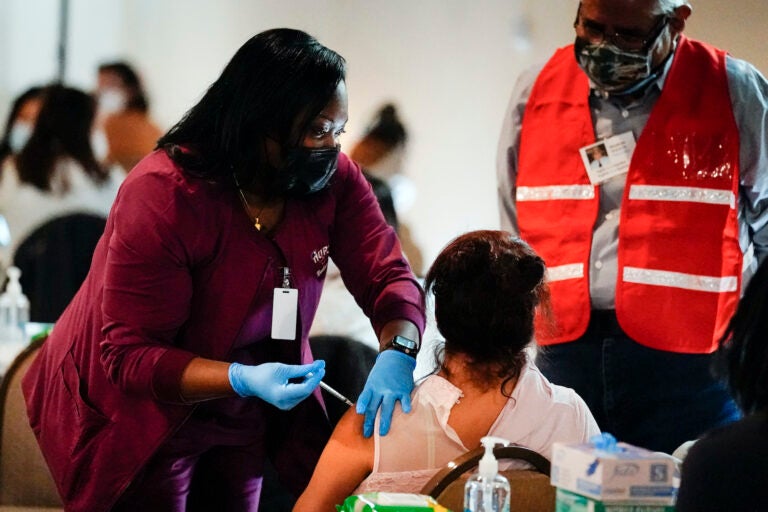
A health worker administers a dose of a Pfizer COVID-19 vaccine during a vaccination clinic at the Grand Yesha Ballroom in Philadelphia, Wednesday, March 17, 2021. (AP Photo/Matt Rourke)
Ask us about COVID-19: What questions do you have about the coronavirus and vaccines?
This is one of a series of articles in which reporters from WHYY’s Health Desk Help Desk answer questions about vaccines and COVID-19 submitted by you, our audience.
Six months after your second dose — that’s the vaccine-booster timeline the White House is likely to recommend for people who got the Pfizer or Moderna shots, according to a Wall Street Journal report last week.
It’s also two months earlier than the Biden administration recommended in its announcement about booster shots just two weeks ago. The administration and COVID-19 vaccine producers plan to start distributing booster doses at the end of September.
Pfizer said Wednesday it has started the process of applying to the Food and Drug Administration for approval to offer a third dose of its two-shot vaccine. Moderna is expected to do the same, according to the Associated Press.
Scientists and health experts are divided on what the best timing for boosters actually is. Here’s what we know right now.
What led to the White House booster recommendation?
Though research is continuing, early data using different methodologies suggests that immunity from the vaccines wanes at about eight months or earlier as the coronavirus’ delta variant spreads. That’s one of the reasons why there have been some breakthrough infections, health experts say.
The Centers for Disease Control and Prevention released two studies last week: one focusing on health care workers that found effectiveness declining by almost 30 percentage points, and another in Los Angeles that found 25% of new infections between May and July were among fully vaccinated people (though hospitalizations were mostly among the unvaccinated).
A study out of the U.K published last week that evaluated positive COVID-19 tests showed that protection after two shots of the Pfizer vaccine decreased from 88% at one month to 74% at five to six months.
Last month, Israel was one of the first countries to approve a Pfizer booster for older people, after its studies found vaccine protection against severe illness had waned, especially for seniors. Boosters there have reduced the risk of infection in people over age 60 by 86% and against severe infection by 92%, Israel reports.
Last week, both Pfizer and Johnson & Johnson announced they have non-peer-reviewed data showing their boosters increase protection from COVID-19. J&J’s study suggests boosters after six months increase antibody protection ninefold. Pfizer says its booster after five to eight months increases antibodies by three times.
The vaccinations’ original dosages are still very effective, though. They are protective against hospitalizations, serious illness, and death. Data shows that the unvaccinated are hit hardest by the pandemic: It’s estimated that 97% of hospitalizations and 99% of deaths are occurring among those who have not been vaccinated. Though the occurrences are rare, a small proportion of vaccinated people can still get serious illness and be admitted to the hospital.
So the vaccines are a bit like insurance.
“The current part of this pandemic is very clearly a pandemic of the uninsured, but it’s not exclusive to the uninsured. And so we’re trying to bring back into alignment a much stronger immunity among those who have already gotten the vaccine,” said Dr. Gabor Kelen, director of Johns Hopkins University’s Department of Emergency Medicine, who is known for his research in emerging infections.
Data on breakthrough coronavirus infections should be put in context, said Dr. E. John Wherry, director of the Institute for Immunology at the Perelman School of Medicine at the University of Pennsylvania. The mRNA vaccines (Pfizer and Moderna) are 95% effective against the original strain of the virus, meaning 5% of vaccinated people could still catch it. Almost 200 million people in the United States are fully vaccinated. Though 5% is a small portion of the total, people might be alarmed if they looked only at the raw number, or 10 million, Wherry said.
“So we’re seeing this kind of denominator problem, where everybody knows somebody who’s gotten the vaccine, got infected, and gotten sick. And that’s creating a little bit of confusion about whether vaccines are still working,” he said.
The idea is not that vaccines prevent any and all infection. What the vaccines actually were intended to do is prevent disease, hospitalization and death, Wherry said, and they still do.
The recommendation’s timing: Pros and cons
Recommendations for boosters should be distinguished between individual need and the need for a nationwide policy, Wherry said.
For certain individuals, booster vaccines could have some benefit and likely won’t cause any adverse reactions.
“It’s going to top off the antibodies a little bit, they increase your protection slightly, and it really doesn’t have a considerable downside, because if you didn’t have a severe adverse event after two doses, the likelihood of having a severe adverse event after a third dose is much lower,” Wherry said.
He agrees that immunocompromised people should get access to boosters now. Studies show that people whose immune systems are suppressed produce few to no antibodies after getting the COVID-19 vaccine, and that boosters do help them to produce more. Older people also would benefit from boosters because vaccines do not work as well in that population. Those groups also are at increased risk for severe illness if they contract the coronavirus.
But Wherry argues that while everyone else will likely need boosters at some point, now is not the time. There are a couple reasons why.
The big-picture question is: “Will boosters prevent disease?” Wherry argues boosters are unlikely to change the burden of disease nationally. He also said more data about breakthrough infections and how boosters would dampen the spread of the disease needs to be collected before making booster recommendations for the rest of the population.
“What we know so far is that boosters do seem to increase the amount of antibodies that you have. We don’t know how durable that increase is going to be, and we don’t necessarily know how much that’s going to impact prevention of infection, separating infection from disease,” Wherry said.
“I think the jury’s still out at this point. We have a couple of key pieces of missing data. We have no national approach to asking, of all the people hospitalized with COVID, how many of them are vaccinated versus how many are unvaccinated. And if we don’t know that, we can’t track to see whether that ratio is increasing — that is, more vaccinated people ending up hospitalized. That, to me, would be the most important piece of information at this point.”
A better use of resources, Wherry said, would be getting the unvaccinated vaccinated, because they are the source of the vast majority of new infections, the burden on hospitals, health care costs, and mortality.
“As a policy decision, I think it’s a little bit early because the resources and attention that go to boosting healthy people maybe could be better spent trying to get higher vaccination coverage in the unvaccinated,” he said.
Other health experts argue that the limited data available is enough to recommend boosters. Kelen points to data out of Israel showing breakthrough infections with more serious symptoms.
“So we have to consider that when you roll this out, you can’t wait for the absolute perfect moment where there’s some tripwire in the data. It’s suspicious enough,” Kelen said.
“Many of us, myself included, are actually at that shelf life that’s expired at around eight months — it’s kind of like a `best before’ date — and we are really looking forward to the opportunity to get our immunity boosted back up with the anticipation that it’ll be stronger, even against the delta virus,” Kelen said. “And some of the precautions that now have to be reimposed for vaccinated people might be able to be relaxed as we get a large number of vaccinated people boosted back up.”
Dr. Stanley Weiss, professor of medicine at the Rutgers New Jersey Medical School and professor of biostatistics and epidemiology at the Rutgers School of Public Health, goes as far as saying that, if anything, the recommendation for boosters came too late.
“It’s been clear to many of us that the delta variant and other variants pose great dangers, we’re seeing that evolving in these statistics almost every day. So there is some urgency in achieving better protection,” Weiss said.
The World Health Organization has called for a two-month booster moratorium, arguing that people who don’t yet have access to vaccines, such as those in countries with limited resources, should be vaccinated first. Some countries have only 1% of their populations vaccinated because of access issues.
On the other hand, Kelen said, the U.S. has a lot of unused vaccine inventory because fewer people have gotten the shots than health officials had hoped for.
“Given that some of the vaccines sitting on shelves might expire soon, the kind of effort of boxing it up and making sure that it’s good and shipping it and figuring out exactly where it goes becomes a little bit problematic,” Kelen said.
“But I’m very sympathetic … to the perspective of the World Health Organization. This is a virus that doesn’t look out to see who you are. Rich country, poor country, rich person, poor person. It’s finding everybody,” he said.
“Until we get herd immunity, throughout pretty much almost the entire world, this virus is going to find people who are not vaccinated in particular. And it’s clever — and that through natural selection, it can mutate so that it continues to evolve and evade whatever immunity the vaccines have given us,” Kelen said. “The problem is we didn’t vaccinate enough people fast enough. And so these kinds of variants emerged and now are a big problem.”
Is it normal for immunity from vaccines to wane this quickly?
Kelen and Wherry said the effectiveness of the COVID-19 vaccine is beyond original expectations, even with the waning levels of immunity. They said because the vaccine has had so much media attention, expectations from the general public were set too high.
“Ninety-five percent protection is just an absolutely amazing number for Moderna and Pfizer when you think that when we were first developing vaccines, we were hoping for 70%, and we were going to accept 50% as very reasonable. And so here we are in the very upper echelons of protection,” Kelen said. “Coronaviruses mutate, and as delta did, mutate just enough that as immunity wanes, the immunity is imperfect to completely combat it. For some people, obviously not others. It is still pretty effective.”
Wherry said it is normal for vaccine effectiveness to wane over time.
“We have a few that give you lifelong immunity, but many of them we need boosters at, sometimes 10 years, sometimes yearly, depending on the vaccine … every 10 years in the case of things like diphtheria, tetanus, and then often just a second time in your life for something like the chickenpox vaccine.”
And there are breakthrough infections following other inoculations, too.
“Our yearly flu vaccine is a great example,” Wherry said. “Maybe not the most efficacious vaccine, in general, but we get it every year. It prevents an enormous number of deaths and disease. But you can still get infected after you get it. Your symptoms will be milder, most of the time you won’t end up hospitalized, and most of the time won’t end up dying.”
The COVID vaccines still are very effective against the original strain of the virus. But the delta variant is more difficult to fight.
“The issue is that the delta variant is much harder to control. And therefore, one needs a higher level of immune protection against it than we needed against the original strain for which the vaccines were developed,” Weiss said. “So the vaccines are still giving excellent protection against the original … but the evolving strain in the United States is now overwhelmingly delta, and you are not adequately protected against delta from the original vaccinations as time passes on and your immune system begins to wane.”
Health experts don’t know yet how often people might need boosters.
What about those studies showing waning immunity?
All the studies measure effectiveness in different ways, Wherry said, so they need to be explained within context.
For example, he said, some studies do not distinguish severity of infection, or hospitalization, among breakthrough infections. They monitor for all infections, even mild ones.
“Even in those people that got infected after having been vaccinated, they are protected from the worst consequences of being infected. That’s really the main goal of vaccines. We wish we were not getting any infections, but very few vaccines give us true sterilizing immunity that prevents any infection whatsoever,” Wherry said.
“It’s the first time we’ve been monitoring this closely. So we’re picking up events that are of relatively little medical consequence. Certainly for the person infected who gets maybe a fever and feels kind of crummy for a couple of days, it’s a consequence to their productivity. But it’s not a long-term consequence to them like it is if they were not vaccinated and they might die, or end up with long COVID, or be in the ICU for two weeks.”
A second example, he said, is the study out of Israel, which also saw increased infections among people who were vaccinated in the beginning of the rollout.
“At the beginning of the vaccination campaign, both in Israel and here, the people who were vaccinated were frontline health care workers and high-risk individuals who are likely to be highly exposed. So it’s not an apples-to-apples comparison because they’re likely to have been exposed a whole lot more than people who were vaccinated at the end of that study,” Wherry said.
“I don’t want to make it sound like the science that’s emerging is not useful, or that all of it has caveats. They’re all sort of pieces of a very large puzzle, and we have to assess them in context, so we get a better picture of what the puzzle is,” he said.
“Seek out good, trusted experts to listen to, and recognize that every time we have new data, that may change how the experts are thinking about what that puzzle really looks like,” Wherry said. “So don’t be afraid of hearing experts like [National Institute of Allergies and Infectious Diseases director Dr. Anthony] Fauci adjust their recommendation based on new data coming out. That’s the scientific process. That’s exactly what we want to happen.
“That’s not changing our minds,” Wherry said. “It’s actually being better informed as better and better data comes out.”
Both Wherry and Kelen said it’s not surprising that among older people, immunity from the vaccine wanes over time, because as a person ages, the more difficult it is to stimulate the immune system. Older people will be among the first people eligible to get boosters, an order of eligibility similar to when the vaccines first rolled out.
Wherry recommends that people of advanced age or who have other medical concerns talk to their doctors.
“I think what is really good about the FDA approval [of the Pfizer vaccine], and by some of this discussion about boosters, is you’re now putting some of the ability to make those decisions in physicians’ hands. That’s where I think we should be,” he said. “I think this is something that we should be dealing with at the level of the individual patient based on the patient’s characteristics and potential needs. I also think we may soon get to a point where we can actually do some evaluation clinically of whether your immunity has waned or not.”
What if I got the J&J vaccine?
Johnson & Johnson released findings of its own non-peer-reviewed study last week showing that its booster shot was effective in a clinical trial. For now, recipients of the J&J vaccine must sit tight.
Early data also suggests that mixing vaccines might provide some benefit, but mixing will not likely be recommended in the U.S. soon.
Do boosters target variants?
There are some ongoing clinical trials researching boosters that target specific variants of the coronavirus. But the boosters available now are essentially the same vaccine that you already received. The experts say it’s worthwhile to get a booster because it still enhances immunity to all variants.
More information is needed, but Weiss said it’s very likely that boosters targeting specific variants would be helpful.
“We do know from some studies that getting an additional booster led to a significant increase in measures of immune protection,” he said. “So that’s why we think this is a rational way to go. It’s not yet clear how over time we may need to alter those types of booster vaccines or what frequency. We’re still relatively early in this worldwide pandemic, and things are rapidly changing around the world with the evolution of new variants every day.”
Can boosters play a larger role in the battle against COVID-19?
Boosters will play a vital role, Kelen and Weiss said, because people with breakthrough infections, symptomatic or not, can spread the virus. Studies suggest that people who have been vaccinated and get COVID-19 have just as much viral load in their noses as unvaccinated people.
But boosters alone won’t be enough to tackle the pandemic, they said, because there’s still not enough people vaccinated to approximate herd immunity.
Scientists originally estimated 70% of people would need to be vaccinated to reach herd immunity. But because the delta variant is more contagious, it’s likely 85% to 90% of people will need to be vaccinated, Kelen said.
Young kids also aren’t eligible to be vaccinated yet, though clinical trials are underway.
“Both need to happen; the boosters need to kind of ‘patch up,’ as it were, these breakthrough infections among those of us who were vaccinated,” Kelen said. “But the current pandemic is raging among the unvaccinated. And so we need more and more of those people to be vaccinated.”

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.





![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)