How do COVID-19 vaccines affect people who are immunocompromised?
If you have certain conditions, or are taking certain medications, parts of your immune system may function less effectively. Here’s what we know.
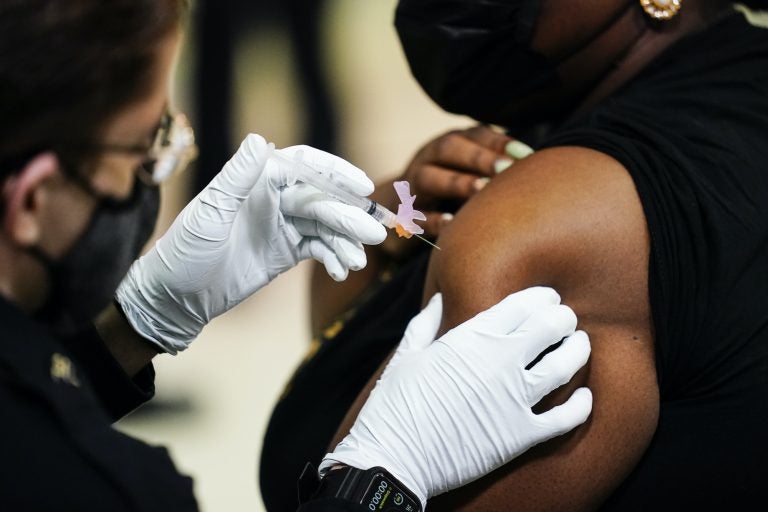
A member of the Philadelphia Fire Department administers the Johnson & Johnson COVID-19 vaccine to a person at a vaccination site setup at a Salvation Army location in Philadelphia, Friday, March 26, 2021. (AP Photo/Matt Rourke)
Ask us about COVID-19: What questions do you have about the coronavirus and vaccines?
This is one of a series of articles in which reporters from WHYY’s Health Desk Help Desk answer questions about vaccines and COVID-19 submitted by you, our audience.
Hannah McIntire commutes from Philadelphia to New York City for work during part of the week.
While returning home on Amtrak last week, she said, some passengers refused to wear masks. The conductor, it seemed, wanted to be as nonconfrontational as possible, opting to use the loudspeaker to remind customers to wear their masks, McIntire said. But some people still didn’t do it.
McIntire, 29, is fully vaccinated, but she still had reason to be concerned. She takes a TNF blocker for two autoimmune conditions, Crohn’s and ankylosing spondylitis. The medication increases people’s susceptibility to infection because it suppresses the immune system by blocking a substance in the body that can cause inflammation and lead to immune-system diseases.
Out of fear the maskless passengers would become belligerent and spread respiratory droplets more as they yelled, McIntire said, she didn’t confront them. She stayed put, hoping that wearing her own mask offered protection.
“Should I move away from them? What should my response be? Because Amtrak is back to full capacity. Now, there’s a lot of things that are increasing in terms of being back to normal,” McIntire said.
“I basically haven’t changed a lot of what I’ve been doing throughout the pandemic. I’m still masking, we haven’t had folks over to our home or anything like that,” she said. “I haven’t gone to a restaurant since the beginning of the pandemic.”
Shelley from New Jersey also is fully vaccinated. But like many leukemia patients, blood tests showed she didn’t produce the antibodies likely needed to prevent COVID-19 infection.
Shelley asked WHYY News to omit her last name because she hasn’t told everyone in her family about her cancer diagnosis. She said she’s concerned about how effective the COVID-19 vaccine is for her, and wants to know how to protect herself.
“I have to proceed, still in a lockdown. And the fact that other people are moving around more freely, and especially without masks, I don’t know how it’s going to be. I don’t go to many places, but I do have to go to the supermarket,” Shelley said. “The bottom line is the world opening up makes things less safe for me, even though I’ve done my best to be safe.”
She said she was very excited to receive the vaccine, but after finding out that she didn’t produce antibodies, she feels depressed because her life can’t get back to normal for a while.
“I don’t like to be frightened of other people, that they could inadvertently give me a disease that I don’t have anything to fight it off with. I would like to get together with my family and friends, which I have not been able to do,” Shelley said. “Unless there’s herd immunity, I’m really beat. I can see that the states, counties, municipalities, are trying different things to lure more people to get the vaccine. But that would be great if there were ways to change people’s minds.”
Based on what health experts and scientists know about conditions and treatments that affect immune response, there is some concern that the COVID-19 vaccine will not protect people who are immunocompromised. But more research needs to be conducted. Here’s what we know and don’t know about vaccines for this population.
Why might the vaccine be less effective for immunocompromised people?
Generally speaking, other types of vaccines, like the flu shot, also can be less effective for people who are immunocompromised.
In clinical trials so far, the effectiveness of the COVID-19 vaccine has correlated with the production of antibodies. That doesn’t mean antibodies are the only function involved in a person’s protection from the virus, but so far, research finds that it’s the strongest correlation.
In people who are immunocompromised, there are certain parts of the immune system that function less effectively. For some, the compromised aspect could be parts of the immune system that help make antibodies, which can prevent COVID-19 infection. But for other people, other aspects of the immune system may not be as highly functioning. For example, HIV patients are often missing T cells or a subset of T cells.
Some cancer patients lose immune cells known as B cells that make antibodies. Prescription drugs that treat some autoimmune diseases, like multiple sclerosis and some rheumatological diseases, also eliminate B cells. So these patients may not make antibodies from the vaccine.
But antibodies aren’t the be-all and end-all. The COVID vaccine also induces T cells, another arm of the immune system.
T cells don’t prevent infection like antibodies do. But T cells do work once a virus starts to infect a few cells, and should be able to eliminate the virus from those cells. So while the COVID-19 vaccine might not prevent infection for immunocompromised patients, it could prevent severe disease and the need for hospitalization.
“There’s some data from patients who have contracted COVID-19 that indicate that T cells do prevent or limit disease severity,” said John Wherry, director of the Institute for Immunology at the Perelman School of Medicine at the University of Pennsylvania. “So there’s some hope in at least some immunocompromised patients who can still mount other types of immune responses like T cells, that maybe they won’t have perfect protection, but disease severity might be limited, maybe they won’t get sick if they get infected.”
How the COVID-19 vaccine works will depend on the kind of condition a patient has and how it suppresses the immune system.
“So a cancer patient will behave differently than a patient with inflammatory bowel disease who’s on what we call a TNF blocker. And those will be different from a transplant patient on broad-spectrum immunosuppression,” Wherry said.
“So I think the key is that, unfortunately, the devil’s in the details, and we need scientific data in each of these different types of immunosuppression. But the early evidence from just a small number of studies emerging is that even when patients don’t make antibodies, they usually make other types of responses to the vaccine.”
What do studies show so far?
There’s not a lot of data available yet. There have been some studies of cancer patients, particularly those with leukemia and lymphoma, that show they can mount some types of immune response to the vaccine, but they don’t make high levels of antibodies.
Several years ago, the Leukemia & Lymphoma Society started a patient registry to compile and compare medical records of blood cancer patients to look for patterns of patient outcomes and treatment side effects. As the COVID-19 vaccines started to roll out, doctors and patients wanted to know if blood cancer patients would respond to the vaccine because of the reduction of certain white cells. In March, the society launched a clinical study of patients’ antibody response to the vaccine.
The trial has enrolled about 7,500 people, and has reviewed the blood tests of about 2,500 people — including Shelley from New Jersey. The results of the study are embargoed, but it’s well known that many blood cancers are B cell-affected and that B cells create antibodies.
“So, it’s no surprise that we’re seeing a lack of response in blood cancer patients who have B cell cancers, just because of their B cell cancer. And then if they’re being treated, to think about it, the treatment is to essentially wipe out B cells. So if treatments that are being given wipe out those cells, the possibility of making antibodies is much less. And that’s the trends that we’re seeing in this study,” said Dr. Larry Saltzman, executive research director at the Leukemia & Lymphoma Society.
Saltzman himself was diagnosed with chronic lymphocytic leukemia. Eighteen months ago, he began CAR T therapy to cure his cancer, but because the therapy essentially got rid of all his B cells, he doesn’t have any antibodies.
It’s not only a concern for patients with blood cancer. For example, a treatment called rituximab that wipes out B cells is also used for multiple sclerosis.
“Any treatment that affects a person’s immunity, meaning the treatments themselves cause immunosuppression, are likely to cause a problem with the production of these antibodies for COVID. So this is a bigger problem than just blood cancer,” Saltzman said.
Scientists don’t yet know if antibodies are the only option for battling COVID-19. The society also is enrolling 1,000 people in a T-cell study to research if those can help people fight off the virus.
“There’s no absolute positive or negative at the moment of, ‘If you made antibodies and you have a certain value in the lab test, is that enough or not enough?’ That’s what we’re trying to study,” Saltzman said. “And in the meantime, it’s challenging because there’s some guidance from the CDC to say that if you had two vaccines, you can essentially go back to your regular life. But the problem is that we have a subset of patients, like cancer patients and other illnesses, that had two vaccines and didn’t make any antibodies.”
The Leukemia & Lymphoma Society is not only checking antibody tests to see who has created an immune response to the vaccine, it’s asking people to share their medical records — that will allow researchers to dig deeper, to look for patterns.
“Maybe there’s a particular flavor of blood cancer or a particular kind of treatment that is better or worse from this. So it’s not just the one point getting an antibody test. It’s a study to look for patterns of what makes things better or worse. And I think that’s the power here,” Saltzman said.
“So we’re in this for the long term. In other words, this registry is focused on COVID at the moment, but it’s really a long-term project to look at the successful treatments and lessening side effects for, in our case, blood cancer.”
There’s also some clinical trial data of HIV patients showing vaccines induced their immunity. Wherry said some of that data comes from South Africa, where not all HIV-infected individuals are on effective treatment for disease. He said that meant there was the expectation at least some of those trial participants would be partially immunocompromised. At least some of the vaccines looked like they induced pretty good immunity in those individuals, though not as good as in HIV-negative people.
Wherry said scientists are still waiting for larger sets of data among rheumatological patients, and among multiple sclerosis patients. A couple of studies have emerged just in the past few weeks that show while antibodies can be reduced, there may still be some other immune responses, he said.
Which immunocompromised people should be most concerned?
The easiest way to answer this question is to group medical conditions into clusters, Wherry said.
Of the most concern are those who have complete immunosuppression, such as bone marrow transplant patients and people who have had certain solid organ transplants whose immune systems are intentionally suppressed so they don’t reject the organs. Transplant patients are highly immunocompromised and must be concerned about all sorts of infectious diseases.
Next on the list are people with specific B cell deficiencies, such as those with B cell leukemia and lymphoma. Patients with multiple sclerosis and a couple of other types of rheumatological disease, like rheumatoid arthritis, are in this same category because they might be treating their condition with a drug that eliminates B cells. A lack of B cells prevents patients from making new antibodies when they get the vaccine.
The next category includes people with non-B cell defeating immunosuppression, such as those with inflammatory bowel disease or rheumatoid arthritis who are receiving TNF blockers that increase susceptibility to infection. These people can be at risk for infections such as tuberculosis and can be predisposed to developing cancer.
There’s not a lot of research about how TNF blockers reduce the effectiveness of the COVID-19 vaccine. However, some studies show that while autoimmune drugs in general can reduce the vaccines’ effectiveness, reductions in antibodies were more modest for people taking TNF blockers than other kinds of medications.
“Every patient’s going to have their own unique story in terms of where they are in their disease control and other comorbidities and things,” Wherry added.
I’m a recovered cancer patient. Should I be concerned?
Usually, although not always, the immune systems of recovered cancer patients return to some level of normality. So they should mount a good response to the COVID-19 vaccine.
If I don’t have antibodies, can I receive an infusion of antibodies?
There are well-known treatments called monoclonal antibodies that can be used to treat COVID-19 patients. A clinical trial from AstraZeneca is pretreating patients with monoclonal antibodies, to see if they will serve as a preventive treatment. That will take a year or more to study, so it’s not readily available treatment.
Is there anyone who should not get the vaccine?
Wherry said he is not aware of a population that should not receive the COVID vaccine.
“The question is, is there a benefit? What’s your risk-benefit equation here for these vaccines? Well, we’ve all heard of a very small number of anecdotal, what I call adverse events. They’re extremely rare with this vaccine. The side effects, people feel like they have the flu for a day or two. They’re not actually sick. It’s the side effects of the vaccine, that’s something different than the adverse events. So the risks of the vaccine are actually quite low,” he said.
“And when you have a patient who may not make antibodies, the question is, is there some benefit? We’re not sure, but you definitely mount immune responses even if you don’t make antibodies. So I think at the moment the recommendation is that those other immune responses may still provide you protection from severe disease. And so most patients should get the vaccine.”
If I don’t produce antibodies, is there any point in my getting the vaccine?
The Leukemia & Lymphoma Society encourages everyone to get the vaccine, regardless of any study that shows there may be a lack of antibody response. That’s because people’s bodies have three facets of fighting infections: B cells, which create antibodies; T cells, which can kill bacteria or viruses; and cellular immunity, which kills foreign invaders.
“For people who have had any kind of vaccine or shot or tetanus shot or COVID shot, if you get a sore arm, that’s happening because of cellular immunity. So we’re recommending everybody get the vaccine, because there’s these three components that we don’t yet have figured out as to say which one of those is more important than the other and can help protect against this,” Saltzman said.
If I don’t get side effects, does this mean my immune system didn’t respond?
Saltzman said after he received the second dose of the Moderna vaccine he had a fever for four days. So he thought he had a significant response to the vaccine. But when he took the antibody test, he didn’t have any antibodies.
“But having said that, I still believe that I had a cellular immunity reaction because if I ran a fever for four days, something was reacting to the fighting or having the vaccine work. And again, I have no idea about T cells, what was going on there. So I think that people who say they’re well off because they had a response to the vaccine, I do think that’s a good thing. However, you’ll hear people who got the shot and it was like nothing, and then they had their blood testing done, and they got tons of antibodies.”
As COVID rules lift, how should I protect myself?
Wherry and Saltzman said people should continue to take COVID-19 seriously. Cases still are high, and even people who are vaccinated can carry asymptomatic infection.
Immunocompromised patients, especially blood cancer patients, who are diagnosed with COVID-19 also become much sicker, with a much greater risk of hospitalization and up to a 55% chance of death.
“The virus has not gone away. Certainly, as we loosen restrictions, we may see numbers bump up a little bit. As travel starts to increase, certainly in the rest of the world, there are major problems in a lot of areas, and problems in other countries, in other continents, will come here. So I think people should still be very vigilant,” Wherry said.
He advised immunocompromised individuals to know the vaccination status of their friends and family, and to keep an eye on the local trends in COVID-19 in their area. If incidents of new infections start rising, they should consider their activities more carefully.
Masking is also very important, Wherry said.
Saltzman said he, too, has remained vigilant.
“A friend of mine asked me if I wanted to go to a San Francisco Giants baseball game. I live in Northern California. I turned it down primarily because even though the baseball park is going to have limited attendance, let’s call it 30% … and I may be able to sit in a pod away from other people, to get into the stadium is a crunch of people going through magnetometers, and when the game is over, it’s a crunch of people all leaving the stadium at the same time,” Saltzman said.
“And so my advice for people who are immunocompromised is not to put themselves in those kinds of situations. Being outdoors with some friends in a social environment is probably fine. I would be careful about putting myself in a situation where there are known individuals who have decided not to get vaccinated.”
In public situations where you don’t know who is vaccinated and who isn’t, Saltzman said he recommends wearing N95 masks and medical gloves.
He also advises people who aren’t immunocompromised to understand that not everyone is protected by the vaccine, and to wear their masks and maintain physical distance when asked.
What about catching COVID from my unvaccinated kids?
Wherry said parents should keep an eye on their children’s symptoms, limit play groups to social groups where the parents are vaccinated, check if teachers and day care workers are vaccinated and ask what the schools or facilities’ COVID policies are. And again, wear masks.
The good news, Wherry said, is that while kids do get COVID-19, younger children don’t seem to be as big a vector for transmission of this infection as, for example, with influenza or respiratory syncytial virus.
“So caution and attention is warranted. But I don’t think that it should be something that parents worry too much about at this point,” Wherry said.
If I’m immunocompromised, when can my life get back to normal?
That’s likely to occur when spread and new infections in your local community are very low, Wherry said. But identifying what “low” means is the difficult part.
“There are always infections in the community (flu, RSV, strep, etc.) that could be concerning for immunocompromised folks,” he said. “I think when we reach these levels or lower for SARS-CoV-2 might be a starting point. If or when we get to herd immunity [likely 70-80% fully vaccinated], we can likely feel a little more comfortable, but local communities might be better or worse on this trajectory.”
Saltzman said he doesn’t want people who are immunocompromised to get too despondent.
“I’ve heard people say, ‘Oh, I have no antibodies, my life’s terrible, it’ll never get back to normal,’ and I tell them that we’re inching back towards normal. And I think if we all hang with this, we will get back to a semblance of being able to do what we like to do.
“We just have to be careful,” he said.

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.







![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)


