How well are contact tracing apps working to alert us to COVID in Pa., Del., and N.J.?
Now that people have been using the apps for a while, states are measuring how useful they actually have been, and what could make them better.
Listen 1:27
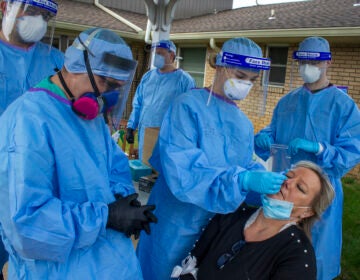
Joseph Ortiz, a contact tracer with New York City's Health + Hospitals battling the coronavirus pandemic, uses his tablet to gather information as he heads to a potential patient's home Thursday, Aug. 6, 2020, in New York. The city has hired more than 3,000 tracers and the city says it's now meeting its goal of reaching about 90% of all newly diagnosed people and completing interviews with 75%. (AP Photo/John Minchillo)
Ask us about COVID-19: What questions do you have about the coronavirus and vaccines?
A few weeks ago, a friend of Jill Fredel’s got an alert on her phone through the COVID Alert DE app, saying that she had been close to someone who tested positive for COVID-19.
Fredel is the director of communications at the Delaware Department of Health and Social Services, and she worked with her friend to think of where she might have been close enough to someone else for the app to send an alert. They realized it must have been at the grocery store.
“That person she passed in the grocery store would never have been able to name her as a close contact, they wouldn’t have known each other’s names,” Fredel said. “That is exactly how we hoped COVID Alert DE would work.” The friend quarantined until she could get a COVID-19 test, which came back negative.
Pennsylvania, Delaware, and New Jersey launched COVID-19 exposure notification apps last year, along with many other states. The apps use Bluetooth technology on smartphones with Apple’s and Google’s operating systems to track whether someone was close to another person who later tested positive for COVID-19, to find and alert more people who might have been exposed to the coronavirus.
Now that people have been using the apps for a while, the states are measuring how useful they actually have been, and what health officials could do to make them even more effective at preventing the spread of COVID-19.
Researchers say these tools are important to study because they could be helpful not just in this pandemic, but for any in the future.
“I think we’re in the infancy of contact tracing apps,’ said Christophe Fraser, infectious disease epidemiologist at Oxford University, speaking at a webinar on exposure notification tools organized by the National Institutes of Health earlier this month.
“I think we can imagine a future … where the current pandemic just wouldn’t have been able to spread with … rapid testing, immediate contact tracing, and rapid learning of how transmission works.”
At the NIH webinar, scientists talked about possibly using these same tools to stop the spread of flu, tuberculosis, and measles.
In the current pandemic, the biggest question about the apps is: How many cases of COVID-19 were prevented because an app got someone to quarantine or get tested in time?
That’s a difficult question to answer, because the apps, by design, do not collect any information about the people who downloaded them.
“They preserve privacy so well that we don’t really get much data,” said Joanna Masel, a data scientist at the University of Arizona who has studied these apps.
There are ways around that. For instance, Masel and her team studied how effective the University of Arizona’s COVID-19 alert app was by adding questions to the manual contact tracing process: asking how many had the app, whether they entered a code after a positive COVID-19 test, and whether they had ever gotten an alert.
In a preliminary study, Masel’s team researched use of the app during a campus outbreak last year. They found that enough people used it, that it led to faster contact tracing, and therefore it was a useful tool.
Oxford University’s Fraser and a team in the U.K. also recently concluded that the National Health Service COVID-19 exposure notification app stopped hundreds of thousands of infections from October to December last year. Millions of people downloaded that app in England and Wales.
“’The public health message is clear: Please use the app, it works,” Fraser said in a statement. “The epidemiological outlook remains concerning, and using the app can contribute to reducing infections until we are all vaccinated.”
Pennsylvania, Delaware, and New Jersey are measuring effectiveness partly in terms of how many people have downloaded the apps for the respective states, out of an estimated number of adults in their states with smartphones.
The goal that the states are aiming for is 15% of the target population, based on an unpublished study from Fraser at Oxford and other researchers modeling the effectiveness of exposure notification apps, and other tools, in stopping transmission of COVID-19 in Washington state. That study found that if 15% of the population used exposure notification tools, the number of infections and deaths would go down by 8% and 6% respectively, “effectively complementing traditional contact tracing.”
Pennsylvania’s app has reached roughly 5% to 6% of the target population, Delaware has reached 13%, and New Jersey has reached 11%.
The states are also measuring how many people who tested positive have logged those results in the app, as well as how many people got alerted from those logged results, and how many of those called a state contact tracer back.
The states are thinking of ways to encourage more people to download and use the apps, such as by adding information on vaccine phases and providers, which Pennsylvania has done. That could get more people to download the apps because a lot of people call the New Jersey Department of Health or go to its website to look up information on vaccines, said Thalia Sirjue, the department’s deputy chief of staff. The health department in Delaware is also considering this.
Another idea for how to make the apps more effective at preventing coronavirus transmission is to automatically send out codes to someone who tests positive, so they can log that result in their app. Right now, whenever someone in Pennsylvania, Delaware, or New Jersey tests positive, a state contact tracer gets in touch with them to give them a code to enter. That becomes a problem when there are so many cases that contact tracers cannot reach them all.
Colorado has already made this an automatic process. A case study found it made a big difference, said Stephanie Hannon, senior director for product management for exposure notifications at Google, at the NIH webinar earlier this month.
Hannon pointed out that with human contact tracers sending codes out for positive tests, Colorado could send about 17 codes a day; with an automatic system, the state sent more than 4,000 codes a day. It also meant a lot more people uploading positive COVID-19 tests to the Colorado app.
“You get incredible results,” Hannon said in the webinar. “The key message is automation.”
That message gets a little more complicated because sending someone a code automatically may not be as effective as a phone call from a human, said Meghna Patel, deputy secretary for health resources and services at the Pennsylvania Department of Health.
“When you actually have someone on the phone walking [you] through the steps, there was a higher compliance,” Patel said.

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.




![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)