What you need to know about the Johnson & Johnson vaccine
This vaccine requires only one dose and uses slightly different technology to fight the virus. Like you, WHYY’s Health Desk Help Desk wanted to know more.
Listen 5:19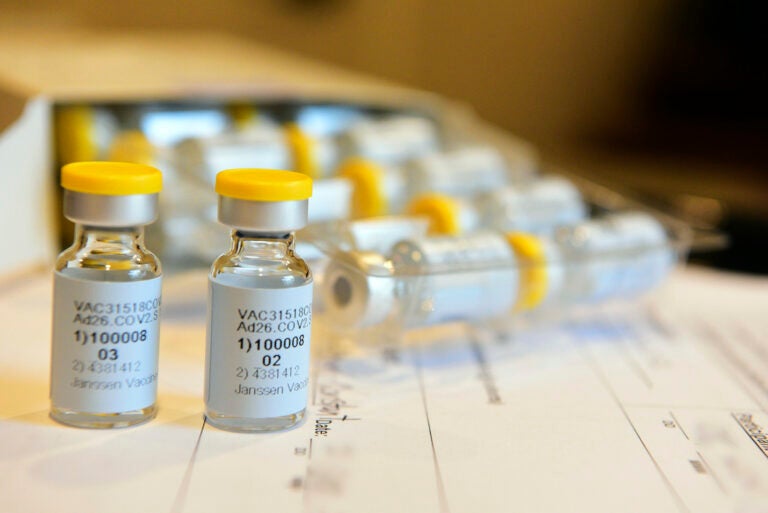
This September 2020 photo provided by Johnson & Johnson shows a single-dose COVID-19 vaccine being developed by the company. (Cheryl Gerber/Courtesy of Johnson & Johnson via AP)
Ask us about COVID-19: What questions do you have about the coronavirus and vaccines?
This is one of a series of articles in which reporters from WHYY’s Health Desk Help Desk answer questions about vaccines and COVID-19 submitted by you, our audience.
Doses of Johnson & Johnson’s coronavirus vaccine for people ages 18 and older was first authorized for emergency use by the Food and Drug Administration in late February. The FDA and the Centers for Disease Control and Prevention called April 13 for a pause in use, “in an abundance of caution,” after six women experienced a rare and severe type of blood clot after receiving the vaccine. But on April 23, U.S. health officials lifted the pause after scientific advisers decided the vaccine’s benefits outweigh the risks.
The government uncovered 15 vaccine recipients who developed the highly unusual kind of blood clot, out of nearly 8 million people given the J&J shot. All were women, most under age 50. Three died, and seven remain hospitalized.
But ultimately the FDA and CDC decided that J&J’s one-and-done vaccine is critical to fight the pandemic — and that the small clot risk could be handled with warnings to help younger women decide if they should use that shot or an alternative.
What’s in the vaccine, and how does it work?
The vaccine, produced by Johnson & Johnson’s Janssen Pharmaceutical Cos. unit, is created using similar, but slightly different technology than is used in making the Pfizer and Moderna vaccines.
Those two use messenger RNA to direct the body to make the virus’ spike protein. Moderna and Pfizer’s vaccines enclose their mRNA in lipid nanoparticles, for which manufacturing facilities have had trouble ramping up production, contributing to bogged-down supply chain issues.
Johnson & Johnson’s vaccine also delivers the body a recipe for creating the spike protein, but it uses DNA instead of RNA. That DNA is encapsulated in an inactivated adenovirus — the virus that causes the common cold — that cannot replicate in the body.
Once the cells create the spike protein found on the coronavirus, the immune system responds, conferring protection if the person is exposed to the real virus.
Vaccine recipients cannot catch COVID-19 or a cold from any of the vaccines because they do not contain live virus.
What else makes the Johnson & Johnson vaccine different?
Johnson & Johnson’s vaccine is effective after only one dose, while Moderna and Pfizer both require two. Because of that, health officials in some jurisdictions are considering offering the Johnson & Johnson vaccine to those who may be hard to reach or who are otherwise unlikely to get a second dose.
“I think in terms of one shot versus two shots, you can start thinking about underserved communities where it may be harder to follow up and ask people to come back for second shots,” said John Wherry, director of the Institute for Immunology at the Perelman School of Medicine at the University of Pennsylvania. “You think about populations that are more transient that are harder to track.”
Both the Moderna and Pfizer vaccines require cold storage that makes delivery complicated, while Johnson & Johnson’s vaccine can be kept at normal refrigerated temperatures. Wherry said that opens up possibilities for delivery to rural America, farther from major medical centers that have the necessary cold chain for the other vaccines.
I’ve heard the Johnson and Johnson vaccine is less effective. Is that true?
In clinical trials, all three vaccines were 100% effective at preventing death, and are effective at preventing severe illness from COVID-19, which health experts say is their most important attribute.
The Johnson & Johnson vaccine was 85% effective at preventing moderate to severe illness in trials. It is 66% effective in preventing symptomatic illness 28 days after vaccination, compared to about 95% for the Pfizer and Moderna vaccines. But it’s important to remember that 66% is still a high number — the flu vaccine reduces the risk of illness by between 40% and 60%.
“This is an extremely good vaccine, the efficacy is very high by standards of most vaccines,” said Wherry. “If we had said a year ago that we would have a vaccine that has the characteristics of the Johnson & Johnson vaccine by the end of February next year, we would have all been overjoyed.”
The Johnson & Johnson vaccine appears to protect against several variants of the virus. The FDA says efficacy “demonstrated in the clinical trial reflected protection against several emerging SARS-CoV-2 variants of concern, including the Wuhan-H1 variant D614G (predominant in the United States), the B.1.351 variant (predominant in South Africa), and a P.2 variant (predominant in Brazil).” The company has applied to British regulators for permission to distribute the vaccine there; a variant known as B.1.1.7 is common in the United Kingdom.
Will the Johnson & Johnson vaccine be targeted to any particular population?
Philadelphia officials have decided to dedicate the Johnson & Johnson vaccine for those who are “hard to reach.” That includes people who are homebound, people with limited mobility, and people experiencing homelessness. If supply of this vaccine increases, however, the city will consider expanding eligibility.
Pennsylvania will allocate the Johnson & Johnson vaccine to public and private school teachers and staff, including bus drivers, to reopen schools as soon as possible. The vaccine will first be offered to pre-K and elementary school teachers and staff, and those who teach children with disabilities and English-language learners.
Delaware is urging people to accept whatever vaccine they can get first, and it is not targeting any particular population for the Johnson & Johnson vaccine.
New Jersey plans to distribute the Johnson & Johnson vaccine to underserved communities, including communities of color, and vulnerable populations like people experiencing homelessness, those living in senior housing, homebound seniors, low-income residents, and people with disabilities.
Will authorization of the J&J vaccine help speed up the process?
Officials say they’re hopeful the Johnson & Johnson vaccine will speed up the process because it requires only one dose. The Biden administration announced Wednesday that it anticipated there would be enough vaccines for all adults in the United States by the end of May — as opposed to the end of July, the previous forecast.
The Moderna and Pfizer vaccines require two doses, which can take about six weeks to complete. In addition, the Johnson & Johnson vaccine has simpler storage requirements, which means it can be distributed to much wider geographic locations.
A single dose also could mean a much simpler distribution process, because providers don’t have to worry about follow-up and tracking patients, or run the risk of giving someone’s second dose to the wrong person.
What about side effects?
Side effects are slightly milder and less commonly reported than with the Pfizer and Moderna vaccines. The most common side effects are fever and fatigue.
“I think it’s important to distinguish side effects from adverse events. Adverse events are things a drug causes that are unintended and are usually detrimental. The adverse-event profile of all these vaccines is excellent. It’s very infrequent that someone has an allergic reaction to Pfizer and Moderna,” Wherry said. He stressed that these vaccines are, in fact, designed to produce side effects.
“The side effects that we’re seeing with the vaccination are a reflection of your immune response working. It doesn’t necessarily mean stronger side effects are giving you better protection from disease. But it does tell you that your immune response is engaged and is starting to do something in response to the vaccination.”
Wherry added that when you have chills and a fever for 24 hours, it’s not pleasant, but it is a sign your immune response is responding to the vaccine and an indicator that you’re generating lasting antibodies that will protect you in the future.

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.




![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)





