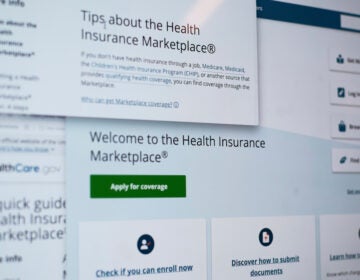
How my mom saved my life after doctors missed my brain bleed
As a budding school teacher was having a stroke at age 22, medical professionals kept explaining her symptoms away and sending her home. Until her mom stepped in.
Listen 13:55
As a budding school teacher, Mimi Hayes (right) was having a stroke at age 22, medical professionals kept explaining her symptoms away and sending her home until her mom (left) stepped in. (Courtesy of Mimi Hayes)
This story is from The Pulse, a weekly health and science podcast.
Subscribe on Apple Podcasts, Stitcher or wherever you get your podcasts.
I went on a blind date. OKCupid, I think.
He was your typical finance bro: crew cut, one of those fleece vests. We ordered appetizers. My head was throbbing like crazy. All I could think about was getting through this and getting home. My mom picked me up after because my car had broken down that week.
I was 22 at the time, living with my mom in Aurora, Colorado, just about to start my first job as a high school teacher. Mom and I are kind of partners in crime. Speaking of crime, we watch a lot of “Forensic Files” late at night together. She falls asleep to the sound of incriminating evidence.
“I just kind of brushed it off as, ‘Oh well, she’s doing it again,’” my mom said. “`She’s just not taking care of herself, and she’s going in 5,000 directions, which has been an issue with Mimi since day one.’”
But then things got worse. About a week later, I got sick on my way to school and had to pull over on the side of the road to throw up. Mom took me to urgent care that day.
“They said, ‘Oh, it’s vertigo,’” my mom recalled. “So I think they just said get some over the counter Dramamine.”
That stuff you take when you’re carsick. Well, I took that, and that didn’t help. Next up was my primary care doctor. Mom came along to that appointment too. There, they said it had something to do with fluid in my ears. I needed to see a specialist.
Mom got crafty. She decided to get me on the family inversion table and had my older sister flip me upside down for about 10 minutes, to get the supposedly blocked fluid out of my ears.
It was the weirdest feeling: All of my guts felt like they were in my head, like not in a normal way. I got so terribly sick after that first flip, I couldn’t move my head without puking.
My sister rushed me to the nearest ER. They didn’t have any answers. As far as they were concerned, I was dehydrated. A nurse missed my vein and an entire bag of IV fluid leaked into my lap, and she accused me of pissing myself.
Next, I saw the neurologist.
”And he literally did this, you know, follow my fingers,” my mom said, describing how the doctor waved one finger in front of my face. “[Mimi’s] saying, ‘There’s two fingers, there’s two fingers.’ And then he walked away, and that was all he did.”
He had only been holding up one finger. I had been seeing double, but that neurologist didn’t see my double vision as too concerning.
In the morning, Mom made me call my doctor and tell her what happened, but I kept getting a nurse and she told me to just get some rest. At that point, Mom snapped.
Mom is not the type to roll over. Picture Queen Khaleesi in “Game of Thrones” when she goes all fire and brimstone. She left work and burst into our house and took me back to the ER, this time at a different hospital.
When we arrived, there was a very quick, brief triage, questions about, you know, am I bleeding. It just felt like I didn’t deserve to be there. Because I was so sick and I didn’t know what was going on.
I was also worried that my mom was going to cause a scene. And she did.
“I immediately informed them that I’d already talked to my attorney, and that we weren’t leaving until they figured out what was wrong with you,” my mom said. “And so I was lying through my teeth.”
She had no attorney.
Finally, we got in to see a nurse, and she did that same neuro test, holding her finger in front of my eyes — except she was doing it wrong. She wasn’t moving her finger. My mom leaped into action.
“And I said, ‘No.’ And I had seen the neurologist the day before do the neurological exam with his finger,” Mom recalled. “And so I did the exam. I literally pushed the lady out of the way. That’s how crazy I was.”
When my mom did the neuro test, my eyes were all over the place, wiggling and not able to follow her finger. They finally agreed to give me an MRI. The scan revealed a circular blood spot on my brain, a ruptured clump of cells called a cavernous angioma sitting in my cerebellum on the right side. That’s when they said the words “hemorrhagic stroke” for the first time.
And then the nurse quickly left the room. And I had a panic attack. Was I about to die right now on this little metal table? How long can you live with a bleed in your brain anyway?
My bleed was contained inside that clump of cells. At least for the time being. The clump had perhaps been there since I was born, and now it had filled with blood. They sent me home with some steroids and told me to check in in a few weeks.
I didn’t get better. I got worse. The brain bleed continued to grow. Eventually, I wasn’t able to walk or see straight. I needed brain surgery to remove the bleeding clump of cells, and then months of rehab, to relearn how to walk, talk, and do third-grade math problems.
My mom saved my life that day. But what if she hadn’t been there? What if they didn’t catch it at all? I could’ve ended up permanently disabled. Or worse — I could have died. I couldn’t help but feel angry. How come everybody but my mom dismissed my symptoms?
“I think there’s no doubt from what you’ve said that what you experienced would probably be classified as a medical mistake or a medical error. It’s the kind of error we would call a ‘diagnostic delay,’” said Matthew Wynia, director of the Center of Bioethics and Humanities at University of Colorado’s Anschutz Medical Campus.
Wynia studies breakdowns in the health care system.
“And so if you are dealing with a young person, the odds that they’re going to be having a stroke compared to, you know, a 70-or an 80-year-old, are really, really small. They’re not zero though, as you know, but they’re quite small. And so the barrier to jumping straight to, you know, a CT scan or an MRI scan is considerably higher,” he said.
For physicians, this can be a balancing act, Wynia said.
“At what point do you pull the trigger and say, OK, we ought to get the MRI scan, knowing that 90 or 99 times out of 100, it’s not going to show anything useful, and a few times out of 100, it might actually end up being harmful.”
There’s some interesting psychology on this, too. Wynia called it “premature closure,” or the process of finding evidence to support your opinions and downgrading anything that might go against that.
“You know, this is a young woman, she probably has a migraine. OK, so now I’m just looking for things that confirm it to migraine, and anything that disconfirms that I’m going to downplay or downgrade in my mind.”
Subscribe to The Pulse
And while approximately 795,000 people in the U.S. have strokes each year – and 15% of those are young adults and adolescents — they often don’t have any of the typical symptoms.
I talked about that with Amelia Boehme, a neuroepidemiologist at Columbia University.
“So something that’s been quite interesting to me, is there was a recent publication in 2017 that showed about 35% of people between the age of 18 and 35 who were admitted for a stroke did not have any stroke risk factors.”
There’s all these risk factors you usually have before you have a stroke.
“Hypertension, diabetes, hyperlipidemia, atrial fibrillation, patent foramen ovale, which is a small hole in your heart,” Boehme said.
Doctors use the acronym “BE FAST” to identify traditional stroke symptoms: balance, eyes, face, arm and speech test.
I only had the B, balance, and E, eyes, parts.
And we also know very little about the outcomes for young stroke victims, how they recover, and what their quality of life is, said Laura Stein, a professor of emergency medicine at Mount Sinai in New York.
“I can give you statistics about rates of recurrent stroke or rates of heart attack in young people who are hospitalized with these conditions, but I can’t tell you anything about their self-report of quality of life after stroke, about really meaningful things like fatigue, depression, anxiety, ability to go back to every single thing that they were doing,” Stein said. “That’s the kind of data that we really don’t have. And that’s the kind of stuff that’s really meaningful to young people who have their entire lives to live with the experience that they’ve had.”
I was really fortunate to have physical, occupational and speech therapy right after my surgery. But I wanted to know, how were other survivors doing? And where were they?
In an unlikely place, actually. Instagram.

I had been posting pictures about my brain injury for Brain Injury Awareness Month. I was about three years post-stroke. I was living in New York City then, and fulfilling the typical starving-artist stereotype as a stand-up comedian, a nanny, and like five other jobs I can’t even remember.
During March, I posted a picture of myself with noise-canceling headphones, because sound was bothering me on the New York City subways.
“And I just remember I like … I … broke down, all I wanted to do is give you a hug. Because I knew exactly what you were going through. I knew it. Exactly what you were feeling,” Joe Borges, a podcaster and fellow stroke survivor, told me.
In 2016, he was in a parking lot when he had the worst headache of his life. He is still sensitive to sounds like I am.
“I reached out because I saw somebody who was like me, and I needed to connect with somebody like me because I really felt alone. And it was the most isolating time in my life. And I had no idea, because, brain injury, that you had this impact on my life, Mimi.” Joe said. “I’ve been saying like, really grandiose things, but it changed my life. It genuinely changed my life.”
Joe lives out in Los Angeles, and we’ve never met in person. Yet we’ve laughed together, cried together, and given each other our most vulnerable selves.
What started as a way to find people like him has led Joe on a mission: to support and uplift survivors on their roads to recovery and let them know that they are not alone. Joe sends upwards of 30 messages a day to survivors on social media. To give them hope, ask them about their struggles, and to connect them with other survivors in their cities.
“We’re bonded by tragedy, but we’ve become like family by choice. You know, I want everybody to feel this because it’s necessary. It’s necessary to grow and move forward in recovery. You know, even people who are seven, eight, nine, 10, 15, 20 years out, they still have room to grow in recovery. There are people I talked to — some woman, she was like, ‘I’m 14 years out. I had no idea that there were so many people out there.’ It’s like, yes, she feels like she’s recovering all over again. It’s amazing … This is where the focus should be.”
Joe and I are lucky. We’ve recovered in ways that many don’t.
My recovery isn’t over just yet. Maybe it never will be. It’s been six years and I still struggle with fatigue, brain fog, and some double-vision in the mornings. It feels a small price to pay, everything considering.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.