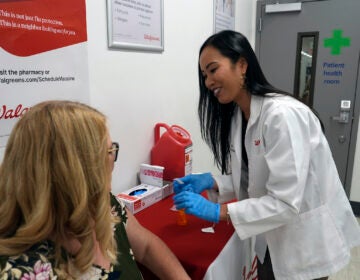
Who’s eligible to get a COVID-19 vaccine booster?
The categories have expanded beyond just people who are immunocompromised. WHYY’s Health Desk Help Desk offers some basic booster answers.
Listen 3:52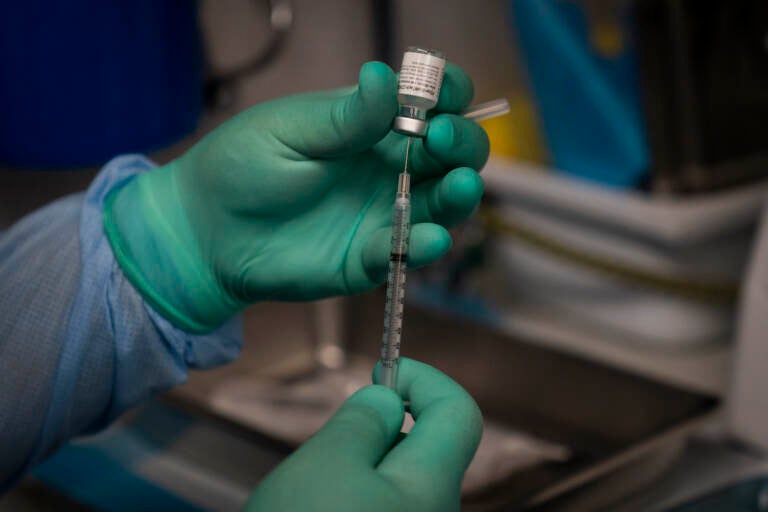
In this Aug. 26, 2021 file photo, Parsia Jahanbani prepares a syringe with the Pfizer COVID-19 vaccine in a mobile vaccine clinic operated by Families Together of Orange County in Santa Ana, Calif. (AP Photo/Jae C. Hong, File)
Ask us about COVID-19: What questions do you have about the coronavirus and vaccines?
This is one of a series of articles in which reporters from WHYY’s Health Desk Help Desk answer questions about vaccines and COVID-19 submitted by you, our audience.
The Centers for Disease Control and Prevention has just approved Pfizer’s COVID-19 booster for certain groups whose immunity from vaccines might wane over time, as well as those who are at greater risk if they contract the coronavirus and those who are most likely to be exposed to the virus.
Who fits into those categories, and why? Where and when you can get a booster? Following are answers compiled by WHYY’s Health Desk Help Desk.
Who is newly eligible for boosters?
- Anyone over age 65.
- Residents of long-term care facilities.
- Adults with high-risk health conditions. These include, but are not limited to: cancer; chronic heart, lung and kidney diseases; dementia; diabetes; Down syndrome; HIV; obesity; pregnancy; organ transplants; and stroke.
- Adults who have jobs that put them at risk for exposure to the coronavirus (such as health care workers and teachers).
- Adults who live in communal settings (such as prisons and homeless shelters).
Individuals in these groups who have had two doses of the Pfizer shot can get the booster six months after the second dose. More than 13 million people ages 65 and older got the Pfizer shot and would be eligible for a booster shot now, the CDC says.
People who are immunocompromised have been eligible for boosters for several weeks now.
Why these groups?
Public health surveillance data suggests that six to eight months after they have gotten vaccinated, there’s a slight increase in the rate of breakthrough COVID-19 infections among people over 65. The most extensive data comes from Israel, where there’s been an increase of COVID-19 hospitalization among vaccinated people over 65. (The data in the United States is not as complete.) Israel is already giving boosters to people over age 65, and the data shows that the booster shots are safe.
“This is seen with a lot of vaccines across the board: that when you stratify by age groups, you tend to have the most robust immune responses in adults, and once you pass a certain age, it’s tough to say exactly what that age is, but you tend to see the immune function tail off a little bit. So it falls in line with other vaccines, what we would expect in terms of immune benefits for older populations,” said Dr. Neal Goldstein, assistant professor of epidemiology at Drexel University.
The absence of safety data in a large number of people under 65 is one of the reasons why there is no booster recommendation for them.
Immunocompromised people and those with certain high-risk medical conditions have a higher likelihood of developing severe symptoms if they get COVID-19. A subset of people who are immunocompromised, such as organ transplant recipients and people on certain cancer treatments, don’t produce good antibodies after getting the vaccine, and that leaves them more susceptible to infection. Studies show that the immune systems of immunocompromised people get a boost after a third dose.
Booster recommendations do not mean that the vaccine isn’t working. In fact, the data shows the opposite is true.
“Vaccines are working incredibly well to keep people out of the hospital and dying,” said Dr. John Wherry, director of the Institute for Immunology at the Perelman School of Medicine at the University of Pennsylvania.
There has been a slight uptick in vaccinated people getting infected and having milder symptoms, however. Wherry said people are expecting too much, because no vaccine is 100% effective.
“The vaccines were never really intended to prevent any and all infection — what they’re intended to do is keep people out of the hospital and keep people from spreading the virus to other people, which they seem to be doing a pretty good job of still,” Wherry said. “So what we may end up with at the end is that our vaccines have turned this virus from something deadly that has killed millions of people to something that gives you a mild common cold.”
Boosters are common for many other vaccines.
“What the booster dose means is that, over time, somebody’s immune response to a vaccine could go down a little bit. And as such, certain vaccines require boosting every now and then. We see this with certain childhood vaccines,” Goldstein said.
“For folks who don’t want to receive the booster shot as of this recommendation, they still have some degree of protection against severe illness from COVID should they be exposed and infected. But the booster kind of gives them another level of assurance that their immune systems are primed to the best possible sense to protect them from severe illness,” he added.
Where and when can I get a booster?
Eligible people can get their boosters now at pharmacies, federally eligible health centers, and long-term care facilities. The region’s many health departments are good sources for details about locations and booster clinics.
In Philadelphia, the Department of Public Health is providing information on eligibility for the booster shot in a blog post and details on the city’s website about how to find the closest clinics.
In Montgomery County, appointments can be made at www.montcopa.org/COVID-19Vaccine for the health department’s four locations: Bethel Community Church of Pottstown; the county Human Services Center at 1430 DeKalb St., Norristown; the third floor of King of Prussia Mall at the Court; and in the Willow Grove Parkside Shopping Center, 2522 West Moreland Rd, Willow Grove.
Many sites in New Jersey have walk-in availability and extended hours. To find a vaccination site and book an appointment online, visit covid19.nj.gov/finder or call the state’s Vaccine Call Center at 1-855-568-0545.
In Delaware, eligible residents also can seek boosters through their health care providers, at pharmacies, or at standing Division of Public Health vaccine sites:
- Blue Hen Corporate Center: 655 S. Bay Rd., Dover, 19901
- Georgetown Plaza: 19 Georgetown Plaza, Georgetown, 19947
- Canby Park: 1920 Maryland Ave., Wilmington, 19805
- University Plaza, 256 Chapman Rd., Suite 100, Newark, 19702
When will everyone else be eligible?
It’s too early to know, the experts said, because health officials are awaiting more data. Wherry said he would guess that more information might be available in about six to eight weeks.
“But … for a healthy middle-aged or young adult, I wouldn’t be too worried about needing a booster as soon as possible. The vast majority of people in that demographic actually seem to have pretty good immunity,” Wherry said.
Goldstein agreed, saying, “We also know from current evidence that the ability of these shots to confer protection has been remarkable. And these folks should not be concerned right now with needing a booster. We don’t see a recommendation for it because we still see excellent protection against hospitalization, excellent protection from severe disease, in these age groups.”
What type of booster can I get?
Currently, health officials are evaluating the Pfizer booster. Data for Moderna and Johnson & Johnson boosters will be published at a later date.
Pfizer was the vaccine that had the first emergency use authorization from the Food and Drug Administration and the first FDA approval. It’s the shot with the largest body of evidence, which is why its booster is being approved first.
It’s expected that health officials will decide on a Moderna booster shot in the near future. The company said this month that it had submitted initial data on its booster to the FDA. The Moderna vaccine uses the same technology as Pfizer.
Johnson & Johnson also has been studying a booster to follow its single-dose vaccine. It has given initial information to the FDA as well.
My original doses were not Pfizer. Can I still get a booster?
Only people who had two doses of the Pfizer vaccine can get a third dose of Pfizer. There’s currently no recommendation to mix vaccine regimens.
How often will I need a booster?
That’s difficult to say, the experts said. It will depend not only on the level of immunity that people get from the booster, but also on how much virus is circulating and how quickly it gets contained in this country and globally.
Is the booster the same as the first two shots?
The booster being recommended is the exact same shot as the first two doses.
The booster the FDA endorsed is based on the initial virus first found in Wuhan, China. The vaccine still works against variants of the virus, even though that protection dips slightly. In the future, there may be boosters targeting specific variants, but they are not available now.
If I had a breakthrough infection, can I still get a booster?
So far, there hasn’t been any official discussion about that, and there have been no studies on that particular situation, in that order.
The University of Pennsylvania has studied how people who got COVID-19 benefit from the first and second doses of the vaccine after recovering from the virus. Early data suggests that vaccination after an infection gives someone strong immunity. But the opposite has not been studied.
Recent studies suggest that breakthrough infections among those previously vaccinated act similar to boosters — in other words, it increases the immune response. One of these studies evaluates breakthrough infections and antibody levels. But it’s not clear whether someone who received the full vaccine regimen and then later got a breakthrough infection still needs a booster.
“The problem with doing a study like that, though, is because breakthrough infections are still so rare at a population level, the numbers we would need to study something like that may not be possible, so we may not see that recommendation with what the FDA comes out with,” Goldstein said.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.




![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)