Safe injection sites are one answer to the opioid crisis
With 1,200 overdose-related deaths in 2017, Philadelphia is suffering some of the worst effects of the nation’s opioid crisis.

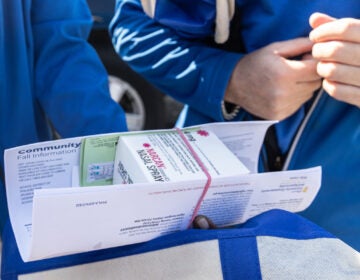
Sarah Evans, a senior program officer at the Open Society Foundations, speaks to Philadelphia's opioid task force in March 2017 about Vancouver's safe injection site. (Katie Colaneri/WHYY)
A quarter century ago, the activist group ACT UP urged Philadelphia officials to establish a syringe exchange to address the exploding HIV infection rates among people who inject drugs. The concept was simple — provide new, clean needles in exchange for used ones, because more than half of the HIV cases were due to drug use.
The idea of syringe exchange was unpopular politically and socially, but then-Mayor Ed Rendell signed an executive order in 1992 legalizing the possession of syringes in Philadelphia, overriding both state and federal laws. Despite cries that drug use and crime would increase, the syringe exchange was established and is now one of the largest in the country.
The effect? The latest statistics from the Philadelphia Department of Public Health show that only 5.5 percent of new HIV infections are among people who inject drugs, with no resulting increase in crime. Clearly this is a public health win.
Today we face a new public health emergency that requires similar courage. With 1,200 overdose-related deaths in 2017 — a dramatic increase from around 450 just four years earlier — Philadelphia is suffering some of the worst effects of the nation’s opioid crisis. Fueled by pure-grade heroin that has often been cut with fentanyl — a synthetic opioid up to 100 times more potent than morphine — this rate is four times the city’s homicide rate in the same time period. It is even more than the 953 AIDS deaths in 1994, at the height of that crisis. Every day, at least three Philadelphians die of an overdose. These people are our brothers and sisters, mothers and fathers, and children.
And so, like 25 years ago, the time again calls for a bold public health strategy. Supervised injection facilities serve as locations where people can inject drugs in the presence of medical professionals so that overdoses can be responded to immediately and resources, such as treatment information, can be provided. Like syringe exchange, this form of harm reduction acknowledges that, in the absence of stopping a negative health behavior, it’s important to provide resources that help people engage in that behavior more safely. We must keep people alive if we have any hope of helping them.
Earlier this year, the city announced the findings of the Mayor’s Task Force to Combat the Opioid Epidemic, supporting the establishment of a safe injection site in Philadelphia, making it the first such site in the country. The backlash to this proposal was immediate, citing similar concerns to those expressed about syringe exchange.
But consider the facts. A recent report estimated that just one location in Philadelphia could prevent between 24 and 76 overdose deaths in a year, saving between $12 million and $74 million — presumably, multiple sites would increase those numbers. Reports from Vancouver, which has had a safe injection site since 2003, show no increase in crime and a 35 percent reduction in overdose-related mortality within 500 meters of the facility. More importantly, it has seen an increase in the number of people provided medical care, drug treatment, and potentially life-saving education on diseases like HIV and hepatitis C.
Harm reduction works. It meets people where they are and ensures that, if and when they are ready to stop using, they can. But it takes perseverance and commitment. If history repeats, the public will warm to the idea of safe injection sites, as they did to syringe exchange. In the meantime, we should support the city’s vision to establish a safe injection site and have the courage to stand up to the opposition.
This is a city that can make it work, like we did 25 years ago, by adopting a bold, life-saving public health strategy to address the opioid epidemic.
—
Sarah Bauerle Bass is associate professor of social and behavioral sciences and director of the Risk Communication Laboratory in Temple University’s College of Public Health.
A version of this op-ed was published on the Temple University website.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.