Rutgers study proposes novel approach for treating traumatic brain injury
More than 2 million are hospitalized in the U.S. every year for traumatic brain injuries. Long-term effects can include epilepsy, depression, and impaired cognitive function.
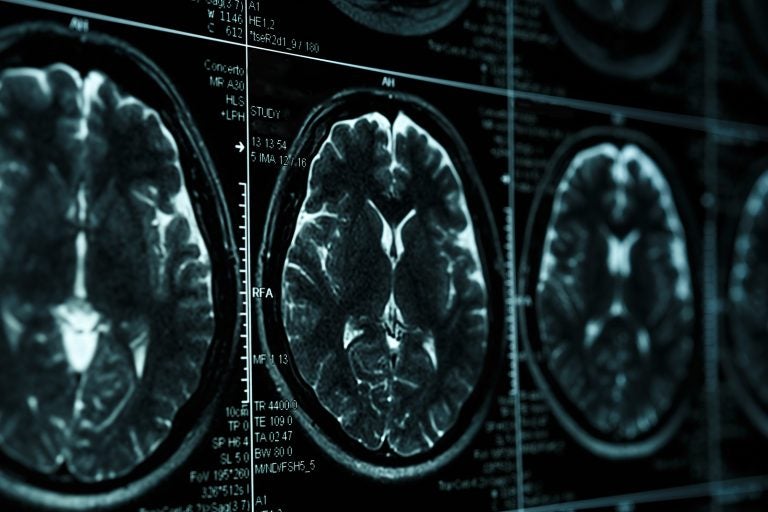
Damage caused by traumatic brain injuries isn’t just the result of the physical blow, but it is connected to the release of a neurotransmitter called glutamate. But the brain has a natural defense against damage caused by glutamate — a compound called cypin. (Bigstock/DedMityay)
A team of Rutgers University-led researchers have discovered two molecules that they say could be the basis for developing new drugs to treat traumatic brain injuries.
The findings are the result of a 10-year study that recently appeared in the journal Neurobiology of Disease.
“I think that this opens up a whole new way of thinking,” said lead author Bonnie Firestein, a professor of cell biology and neuroscience at Rutgers. “Because, if you want to help somebody who’s had a traumatic brain injury, not only do you want to spare their neurons, you want to make sure that their brain is connected properly.”
More than 2 million people are hospitalized in the U.S. every year for traumatic brain injuries. Long-term effects can include epilepsy, depression, and impaired cognitive function.
Damage caused by traumatic brain injuries isn’t just the result of the physical blow, but it is connected to the release of a neurotransmitter called glutamate, Firestein said.
“Under normal circumstances, a little bit of glutamate is really good,” she said. “The problem is, if you have too much of this glutamate released, it starts killing off your nerve cells.”
Nerve cells, also called neurons, are responsible for sending and receiving information in the brain. Together, they form advanced circuits necessary for memory and learning. When glutamate is released, it not only destroys neurons, but also the connections that form those circuits.
But the brain has a natural defense against damage caused by glutamate — a compound called cypin.
“When you have more of this compound cypin, these cells are more resistant to being killed by glutamate,” Firestein said. “So the question is, can we somehow activate this protein?”
To answer that question, the research team began testing different compounds to see which — if any — were able to boost cypin action. After identifying two that fit the bill, the team experimented with cells to see if adding the two compounds, which Firestein called “activators,” could counteract damage caused by glutamate.
“And we found that, in the cells that were treated with the activators, these neurons not only survived, but they also had the correct electrical properties,” she said.
In other words, they were able to maintain the connections that are necessary for learning and memory. A test in mice confirmed that, with the approach, their memory recovered.
The next step, said Firestein, will be trying to develop these two compounds into drugs that can be tested on humans. If successful, these drugs could represent a real step forward in the treatment of traumatic brain injury.
“Previous treatments have offered sparing of nerve cells in the hope that they will reconnect properly, and you will regain your memory,” Firestein said. “So we’re going a step further, where we’re trying to not only help your brain cells survive, but also help them function properly.”
The most immediate boost would be to learning, memory, and great mental clarity. But Firestein said she hopes that the benefits will extend even further.
“My hope is that by studying these compounds and studying how to reconnect the brain and keep the brain functioning, it would then feed into other areas of this person’s life,” she said. “They’re happier, they’re functioning better, they’re moving better, they don’t have as many negative sensations. Because the ultimate goal is not just to have better learning and memory, it’s to have a fuller life.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.