Racial disparity grows as the coronavirus disproportionately claims Black lives in Pa., Jersey and Delaware
Doctors say that information about the virus’ community-specific impacts will only become more critical as the economy reopens.

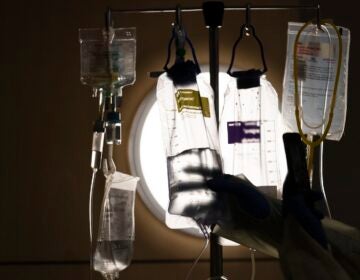
A Black doctor performs a free COVID-19 test in the parking lot of the West Philadelphia Seventh-day Adventist Church. (Christopher Norris for WHYY)
Are you on the front lines of the coronavirus? Help us report on the pandemic.
Black people continue to make up a disproportionate number of the coronavirus cases across Pennsylvania, New Jersey, and Delaware.
The disparity is especially stark in Pennsylvania, where African Americans account for just 11.3% of the state’s population but represent almost a third of the 22,725 COVID-19 cases where the race of the patient was recorded.
Black Pennsylvanians represented 30% of the 2,133 deaths where the race of the victim was known.
Dr. Sharrelle Barber, an assistant research professor at Drexel University’s Department of Epidemiology & Biostatistics, said the differing rates of infection and death between racial groups were significant.
“There are striking racial inequalities, particularly for Blacks,” she said.
The disparity can be credited in part to higher prevalence of common COVID-19 comorbidities, like heart disease or diabetes. But Barber notes that these factors and others are “rooted in structural racism” — from historical disinvestment resulting in more limited access to health care in Black communities to racial segregation pushing Black people into crowded or otherwise substandard housing to the racial character of economic inequality in the region.
“There have been a number of structures that increase exposure. We know that Blacks and Latinos are disproportionately represented among low-wage workers, for example,” she said. “It’s a combination of factors. None of these things can be seen as separate.”
A national and regional trend
The statewide trends in Pa. largely mirror those nationwide, where research has shown the African American mortality rate was, on average, 2.2 times higher than the rate for Latinx people, 2.3 times higher than Asians, and 2.6 times higher than for whites.
Similar patterns were present in New Jersey, where Black residents died at nearly double the rate of white residents. Delaware showed a smaller but still detectable disparity — Black people make up 21% of the state’s population, but about a third of cases and 25% of deaths.
The First State is notably one of just three across the U.S. that releases detailed demographic data about the administration of COVID-19 tests, showing that it had almost doubled the rate of testing among Black and Latinx communities, relative to the white population.
Barber said these figures suggested that at least some localities were compensating for scant testing in Black and Latinx communities early on in the pandemic. But she said the differing testing rates alone were not the root cause of differing racial outcomes.
“Testing alone would not explain the disparity,” she said. “We’re seeing it all over the country. It’s in the South, it’s in Wisconsin, it’s here in Pa. These same racial structures exist everywhere.”
Fighting for information about who is getting sick
Gathering accurate data on racial demographics continues to be a challenge for many states. Pa. was unable to collect demographic data in 62% of all diagnosed COVID-19 cases and nearly half of all deaths. And the state does not currently provide detailed data on deaths or infections among Hispanics.
Dr. Fatima Cody Stanford, an obesity medicine physician-scientist at Harvard Medical School said, during a Wednesday seminar on COVID-19, that difficulty gathering this data could be clouding the full impact of coronavirus.
“We don’t have much countrywide data,” she said. “We’ve had to fight for the data we do have.”
This information will only become more critical as caseloads decline and states begin to take steps to ratchet back from pandemic shutdowns, Barber said. As businesses call employees back to work, Black and Latinx people on the frontlines of the service economy will continue to face greater risk.
“The reopening strategies have not taken equity into consideration and how these steps are going to disproportionately impact Black and brown communities.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.





![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)