Home care industry strained by pandemic
The field of home health care has suffered added pressures during the pandemic. Experts caution that the vaccine rollout will not solve underlying issues around wages.
Listen 4:16
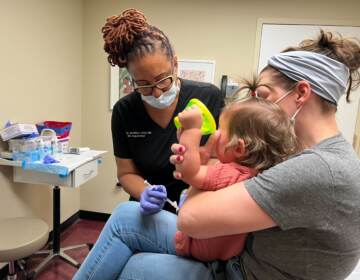
Ray Wall, a licensed practical nurse, positions Steven Sebastianelli in his bed. Wall visits Sebastianelli’s apartment every day to assist him in daily living activities. (Madison Karas/WHYY)
Ray Wall would have preferred to wait things out a bit before getting the COVID-19 vaccine. He wanted to see how others reacted to the shot before getting it himself. But as a nurse, the 47-year-old Philadelphian felt a professional responsibility to get it as soon as possible. So when he was notified that there was a slot for him, he took it.
“I did it against my own beliefs and my own interests of wanting to wait,” Wall said on Jan. 29, a few hours after his first dose. “So I did go in there with a little bit of mixed emotions, but ultimately leaned into what was right and that it was to go ahead and get it as early as I possibly could.”
Wall is the primary nurse for Steven Sebastianelli, a 30-year-old who has spinal muscular atrophy type 2. Wall spends up to 80 hours a week at his client’s apartment in Nicetown, Philadelphia. He takes care of medical needs, and assists Sebastianelli in most activities of daily living, like positioning, feeding and dressing.
Wall and Sebastianelli have been a team for over a decade, but the pandemic has disrupted their daily routines.
In April of last year, the two were interviewing candidates to join Sebastianelli’s round-the-clock rotation of nurses. Then Wall got sick with COVID-19.
“I was like Oh, crap, I’ve got COVID” Wall said. “Which leads me to think maybe Steven also had it. Did I get it from him? Did he get it from me? Did we get it from one of the other nurses?”
Wall’s illness and subsequent quarantine meant Sebastianelli had to rely on backup nurses. This created two worries for the pair: finding nurses to cover Wall’s hours and wondering about the additional risk of exposure.
“There’s no two of me,” Wall said. “There’s not, in-home care, there’s not nurses waiting in the wings to fill a void when there’s not a nurse for a patient.”
And Sebastianelli was worried about whether his fill-in nurses had been exposed to the virus. “There’s so much uncertainty of what’s going to be brought in that it becomes a level of exhaust,” he said.
As the vaccine rollout begins reaching home health care workers in Pennsylvania’s combined Phase 1A and 1B distribution, the chance at a vaccine comes after nearly a year of added complications around caregiving during the pandemic. For workers and clients alike, it’s another wake-up call to longstanding issues in the industry.
The PHI National Workforce Data Center, a research center on direct care professionals, projects more than 341,000 unfilled jobs in home health care in Pennsylvania by 2028.
While need for home health care grows in caring for people with disabilities and people who are aging, the field still struggles with low wages, training, transportation and high turnover, said Philip McCallion, director and professor at the School of Social Work at Temple University.
On top of this, workers frequently report that they don’t feel respected and are not viewed as essential caregivers like other medical professionals, he said.
“We have not given this group who are a very critical workforce, enough attention and enough respect for the really critical job that they’re doing,” McCallion added.
Home health care workers provide personal care for particularly vulnerable populations. They have to navigate transportation between clients and worry about exposing themselves and their own families to the virus. For those with young children, the pandemic added yet another wrinkle.
Lisa DiMeo, owner of SYNERGY HomeCare in Center City says many of her 50 home health care workers couldn’t cover shifts for clients because they couldn’t find childcare.
She says that led to a type of shortage she hadn’t experienced before.
“We were doing our best to not to put them too many places, but it was definitely an all hands on deck kind of situation, where we had to really scramble to get those cases covered,” DiMeo said.
While it’s not uncommon for home health workers to care for multiple clients, during the pandemic, the typical coordination around transportation and balancing different cases became another fear around exposure as workers visited various homes, apartment buildings and long-term care facilities.
For some in the field, the added pressures and risks meant their job was no longer worth it.
Jasmine Henderson, a 30-year-old home health aide in West Philadelphia, has a one-year-old son. Last summer, she stopped working in home health care after four years.
When she returned to the industry last fall, she asked her care agency to assign her to one person.
“Just one person, because like I still have a whole family at home too,” Henderson said. “So I’m not going from this house, to this house, to this house, because you never know who was in there before you, did this person get tested? And just, no.”
She began working with Altonya Sheppard, a 44-year-old social services worker in Southwest Philadelphia, who had already had at least three other home health aides since the pandemic began in March 2020.
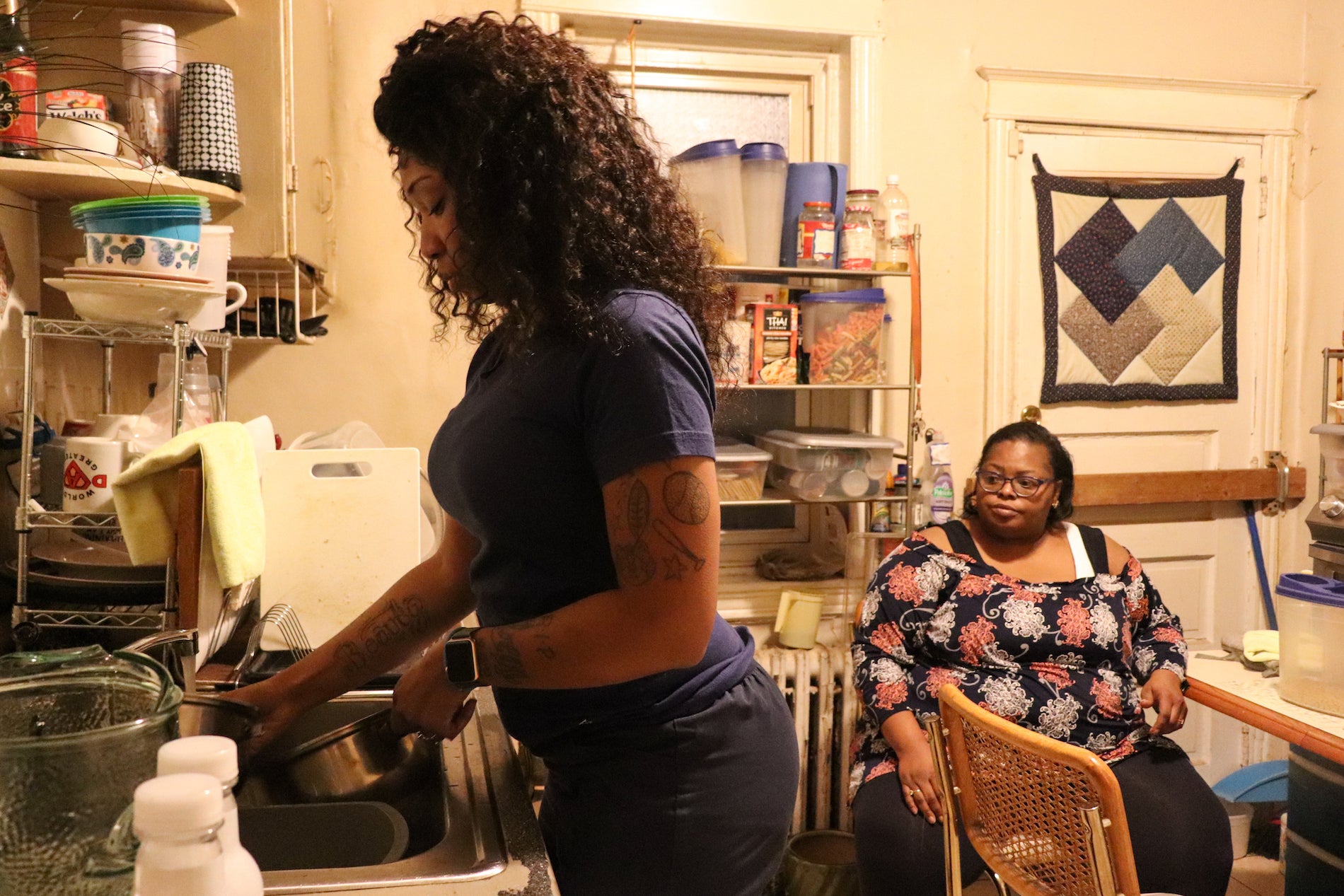
“I was a little hesitant at first about having somebody new coming in because of the pandemic, but she got here she had a mask on and, you know, asked like, do I have hand sanitizer and all that kind of stuff, so I knew that she was pretty much being careful,” Sheppard said.
As schools begin to reopen and the vaccine rollout continues, Lisa DiMeo hopes some of the challenges around coordinating care ease. Clients are requesting vaccinated home health care aides and her workers are beginning to get inoculated after weeks of waiting.
“It’s just going to get better and easier for us as this comes about and I was really very nervous as I was trying to get appointments, over and over again and I wasn’t able to,” DiMeo said. “And I was calling the city and pushing because here we are in group 1A, and we’re still not vaccinated, but I’ve now heard that several people have gotten appointments, including myself, so it’s starting to look a lot better for us now.”
Still, McCallion hopes the pandemic will be a wake-up call to finally address long-standing problems in this critical industry. Better wages, compensation for transportation between clients, and more opportunities for career advancement would be key.
“Their care means that we don’t need to use more expensive alternatives, we should be thinking about that, as we think about appropriate levels of compensation, as well as thinking about appropriate levels of training,” McCallion said.
For people like Sebastianelli, who’s received at-home care most of his life and will continue receiving care during and after the pandemic, he wants people to think critically about improving home health care.
“If there’s a shortage, if there’s this challenge of people not feeling fulfilled in the position of taking care of people how can we fix that?” Sebastianelli asked. “If there’s a problem, how can we ask the questions people aren’t asking?”
 WHYY is one of over 20 news organizations producing Broke in Philly, a collaborative reporting project on solutions to poverty and the city’s push towards economic justice. Follow us at @BrokeInPhilly.
WHYY is one of over 20 news organizations producing Broke in Philly, a collaborative reporting project on solutions to poverty and the city’s push towards economic justice. Follow us at @BrokeInPhilly.

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.




![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)