Black and Hispanic Americans are most likely to miss health screenings due to COVID-19. A Penn physician is meeting the need.
The numbers have been especially stark for colon and breast cancer-screening rates, which dropped by 90% at the height of the pandemic.

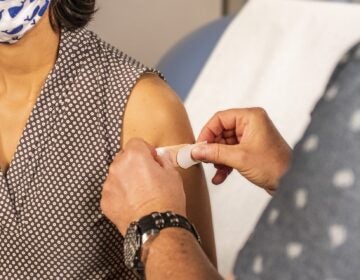
Dr. Carmen Guerra and colleagues partnered with Einstein Medical Center and the Rev. Leroy Miles of Enon Tabernacle Church in Philadelphia to establish a socially distant drive-by FluFIT clinic to simultaneously administer flu vaccines and fecal immunochemical tests for colorectal cancer screening. (Courtesy of Carmen Guerra)
In the early months of the pandemic, doctors’ offices suspended appointments and hospitals cancelled routine procedures as they pivoted focus to managing the coronavirus. Even as those operations have slowly opened back up, the fear of contracting COVID-19 has kept thousands of Americans from getting their standard health screenings.
The numbers have been especially stark for cancer-screening rates, which according to Dr. Carmen E. Guerra dropped by 90% for colon and breast cancer at the height of the pandemic.
Guerra is an associate professor of medicine at the University of Pennsylvania and a health equity researcher who studies cancer-screening disparities in Black and immigrant communities. She said that while colorectal cancer is the third most common cancer in both Black men and women, colonoscopies are the only cancer test that are preventative — meaning screening for colon cancer could also mitigate the risk of cancer down the line.
“It’s an invasive procedure and our most complicated test,” said Guerra. “Most people don’t realize that most cancer screenings just detect cancer once it’s there. But [colonoscopies] remove polyps that look like they want to become dysplastic, which is a term we use for transforming itself into a high-risk lesion.”

According to the American Cancer Society, Black Americans have the highest rates of colorectal cancer when compared to other racial/ethnic groups in the United States. They are 40% more likely to die from this cancer as well. That’s largely due to lack of access to health insurance and high-quality medical care, and to being diagnosed at later stages in the disease.
Even before the pandemic, there were a whole host of structural and social barriers that prevented communities of color across the spectrum from getting screened. A cancer-screening test can be as simple as having a blood test. But for colonoscopies, your colon and rectum must be empty and clean so your doctor can see the entire lining during the test. You might hear this referred to as a bowel prep. That requires time off from work, and access to transportation to and from the procedure. In addition, colon cancer tests require sedation during the procedure, which means you’ll need someone to pick you up when you’re finished.
“Pre-pandemic, underserved communities were having a really difficult time accessing colonoscopy because they [are not] in an economic position to be able to take off work,” said Guerra. “Many communities don’t have the luxury of having a caregiver. They are stretched, everyone in the household is working.”
But then the pandemic swept in, and added another layer of barriers to an already vulnerable segment of the population. Jody Hoyos is the executive vice president of the Prevent Cancer Foundation, which in December, in collaboration with Omnibus, conducted a survey in which 1,200 Black, Hispanic, Asian, and Native Americans were asked questions about their reasons for missed cancer screenings and medical appointments during the pandemic.
Hoyos said the survey found that communities of color, across age and ethnicity, were more likely to have missed appointments during the pandemic than white Americans, with Black and Hispanic Americans about 40% more likely to have missed, postponed, or canceled a health appointment.
“The volume of missed appointments is concerning,” said Hoyos. “We know that the five-year survival rate for cancer is over 80% [when] detected early, but that drops down to 21% if it’s detected in later stages.”
Hoyos also noted that across all groups surveyed, fear of exposure to COVID-19 was the number one reason for missed appointments. For Black and Hispanic Americans in particular, loss of health insurance since the start of the pandemic was the most significant financial barrier this surveyed population brought up.
‘Physicians don’t have the time to solve these barriers’
In 2012, Dr. Guerra reviewed clinical data from Penn Medicine primary care facilities and noticed that residents in West Philadelphia’s five ZIP codes were more likely to have no-shows or cancellations for colonoscopies than non-West Philadelphia residents. In collaboration with the University of Pennsylvania’s Abramson Cancer Center, she and her team proceeded to conduct interviews with community members to better understand why.
Typically, when patients would miss screening appointments, their primary care doctors would simply reschedule the appointments. That did little to solve the problem, Guerra said.
“And that’s when it hit me that physicians just don’t have the time and possibly even awareness to solve these barriers,” she said.
That’s when Guerra and her colleagues decided to create a colorectal cancer screening navigation program, which leverages a workforce of community health workers — who come from the communities they serve — to help patients keep up with medical appointments. Dr. Harold Freeman, a Black surgeon in New York, is the first to have proposed such a program when he noticed Black American women were not coming in for breast cancer screenings.
“And then, ultimately, he was diagnosing [Black American women] with metastatic breast cancer as opposed to his community that’s next door, the Upper East Side of Manhattan, where those patients were coming in with early-stage breast cancer and he was doing surgeries on them,” said Guerra.
Inspired by this model, Guerra and her team sent patient navigators into West Philadelphia. They would call patients who had missed appointments and make plans with them to attend a rescheduled screening together. Navigators were also tasked with collecting more information on why West Philadelphia patients had not shown up to their cancer screenings in the first place. Feedback ranged from not being aware that they were at risk for the cancer and negative beliefs about the procedure’s perceived painfulness.
“But also patients were saying they couldn’t afford the [bowel] prep,” said Guerra. “So what we did was buy the prep for them, and we would mail it to their home.”
Drive-by cancer clinics increased screening rates
The navigation program yielded positive results, greatly increasing rates of screening among West Philadelphians. Guerra and her team expanded the project to other underserved sections of the city, where they administered free stool tests that can identify potential early symptoms of colon cancer.
Then the pandemic hit, and efforts to reach patients in person came to a halt — that is, until the news broke in late August that the esteemed actor Chadwick Boseman had died of metastatic colon cancer.
“And that shocked the world, but I have to say it shocked communities of color even more,” said Guerra. “If someone like him, someone so wonderful, healthy-appearing, and youthful could be taken away from us at an age of 43 from colon cancer, then that led communities [of color] to think that they were also at risk.”
A little over a month after Boseman’s passing, Guerra received a call from Rev. Leroy Miles, an African American pastor at Enon Tabernacle Church, the largest Baptist church in the Philadelphia region. Miles said his predominantly Black congregation was reeling from the news about the actor, and he proposed using the church parking lot to administer colon-cancer screenings.
Guerra and her colleagues jumped at the opportunity, partnering with Einstein Medical Center to establish a socially distant drive-by FluFIT clinic to simultaneously administer flu vaccines and fecal immunochemical tests (FITs) for colorectal cancer screening to almost 200 individuals.

They recruited local health care workers and members of Chi Eta Phi Sorority Inc. to administer flu vaccines donated by the Philadelphia Public Health Department and FITs donated by Polymedco Inc. They established an online registration site, which included a survey to determine screening eligibility and a link to an educational video about colorectal cancer. Participants were asked to complete a questionnaire before and after watching the video to assess their pre- and post-intervention knowledge about colorectal cancer and the likelihood of undergoing screening. Drive-by flu vaccination and FIT retrieval was available on three separate dates, and participants had the option of returning their completed FITs at a church drop box.
“And so I was able to deliver the FIT tests to the community for free, and then I would run them in my office several times a week,” said Guerra. “Of the 192 [tests] that were returned to us, we found 13 individuals who had blood in their sample.”
Blood in the stool is an early sign of colon cancer. So disregarding whether a patient had insurance coverage, Guerra’s team worked with those 13 community members to set them up with diagnostic colonoscopies. She said that if they save just one life, every bit of effort they’ve put into this project will have been worth it.
‘There’s a role here for all of us to play’
The Breast and Cervical Cancer Early Detection Act, which passed in 1990, provided means to every state to screen uninsured populations. That program has really helped to reduce barriers in accessing both breast cancer screening and cervical cancer screening.
“But we don’t have that equivalent for colon cancer, and many of us are calling for that act to be expanded,” said Guerra
Pre-pandemic, physician efforts to increase rates of colon cancer screening were limited to those who were insured. And that’s been problematic, since 27.5 million Americans didn’t have health insurance as of 2018 and many more have lost their coverage during the pandemic.
Hoyos, of the Prevent Cancer Foundation, said outreach and education for the patient population is important, but that bigger pushes are needed on the policy and legislative side to ensure all Americans can afford the health care they deserve.
“What we’re seeing now has been further exacerbated by COVID, but it isn’t new,” said Hoyos. “So there’s a role here for all of us to play, both in the medical community and as people charged with sharing public health information, to help people understand what they can control and how they can be advocates for themselves.”
—
Support for WHYY’s coverage on health equity issues comes from the Commonwealth Fund.

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.