‘No pulse, no problem’: Learning to live with a life-saving device
When Chris Donges was diagnosed with heart failure in 2018, he was given two options: Wait for a heart transplant or implant a medical device onto his heart.
Listen 11:38
Chris Donges was diagnosed with heart failure in 2018—and when his health dramatically declined, he opted to use a new life saving medical device to help his heart pump blood. (Courtesy of Donges)
This story is from The Pulse, a weekly health and science podcast.
Find it on Apple Podcasts, Spotify, or wherever you get your podcasts.
Chris Donges had always perceived his life as normal. The 30-year-old was in a loving relationship with his girlfriend, Meghan Carter. He was an avid Philly sports fan — meaning he’d often attended 76er basketball games. And on special occasions, he’d travel to the beach, where he spent most of his childhood years.
But Chris’ simple life became a lot more complicated in October 2018 — two days before Halloween.
He was at a 76ers game with Meghan when he decided to grab a quick snack during halftime. He filled his plate with a small salad and two measly yeast rolls — and it was enough to make him sick.
“And I looked at Meghan like, ‘oh my gosh,’” Donges said. “I’m going to vomit. I can’t keep this down.”
Chris and Meghan left the game and drove to a local hospital in Wilmington, Delaware, where they live. Chris thought he would be diagnosed with pneumonia or a really bad cold.
But the emergency room staff ran a few tests and diagnosed Chris with left-sided heart failure.
There are two ventricles in the heart chamber. The right ventricle absorbs blood into the heart, and the left ventricle pumps blood out. The left ventricle in Chris’ heart had weakened over time; therefore, he wasn’t getting enough blood supply to the rest of his body.
“They basically said when they looked at the x-ray, my heart almost looked like the size of a gallon of milk,” Donges said. “That’s what my heart got up to in size.”
Doctors measure this kind of heart failure with something called an ejection fraction — a percentage that measures how well your heart is pumping blood to the rest of your body. The lower the rate, the more serious a condition will be.
Chris’ ejection fraction was hovering around 40 percent — right at the line doctors consider heart failure.
He stayed in the hospital for two weeks because fluid had built up in his lungs.
When the heart cannot pump efficiently, blood can back up into the veins that take blood through the lungs.
Subscribe to The Pulse
Chris’ doctors removed the fluid and would only let him leave the hospital on one condition: He had to wear a LifeVest, a device that monitors life-threatening arrhythmia. Some vests can provide shock treatment when cardiac arrest is measured.
Chris wore the vest for a month — and he seemed to be doing well — until the vest alerted him while driving on I-95.
“My ejection fraction almost fell down to roughly 5 percent,” Donges said. “I felt just pain in the center of my chest, and I couldn’t keep anything down. I didn’t even have anything to spit up, but I just felt that bad.”
Chris pulled over and called 911. He was transported to a nearby hospital. He learned that the pain in his chest was due to a blood clot — a problem his vest wouldn’t be able to resolve.
When the heart can’t pump enough blood to meet the body’s needs, blood flow will slow and cause clots to form.
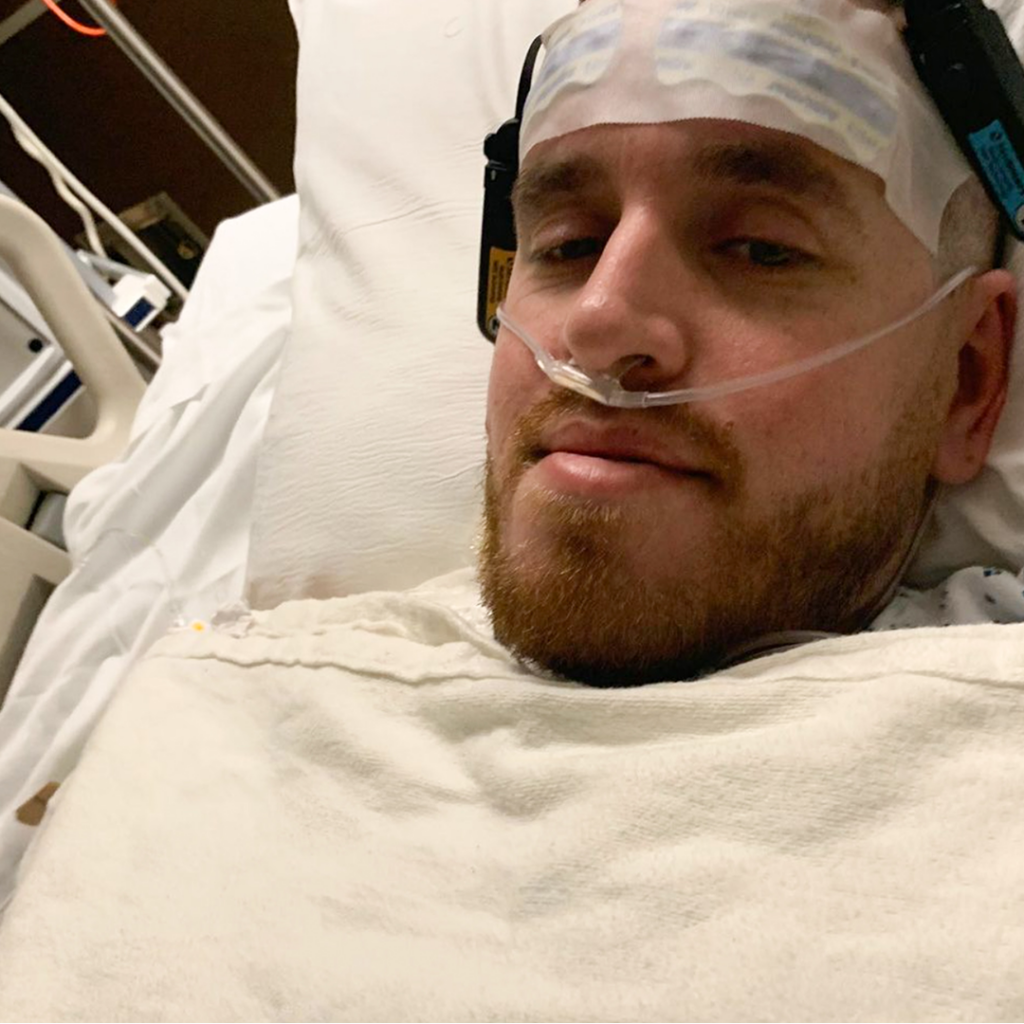
His girlfriend, Meghan, met him at the hospital. She said that Chris’ doctors immediately placed him on life support and later put him in a medically induced coma.
“He had this giant ECMO machine where you saw all these giant tubes of just blood getting pushed around through his body,” Carter said. “He had these little sensors on his head that would monitor his brain activity to make sure everything was still okay there. It was overwhelming, to say the least.”
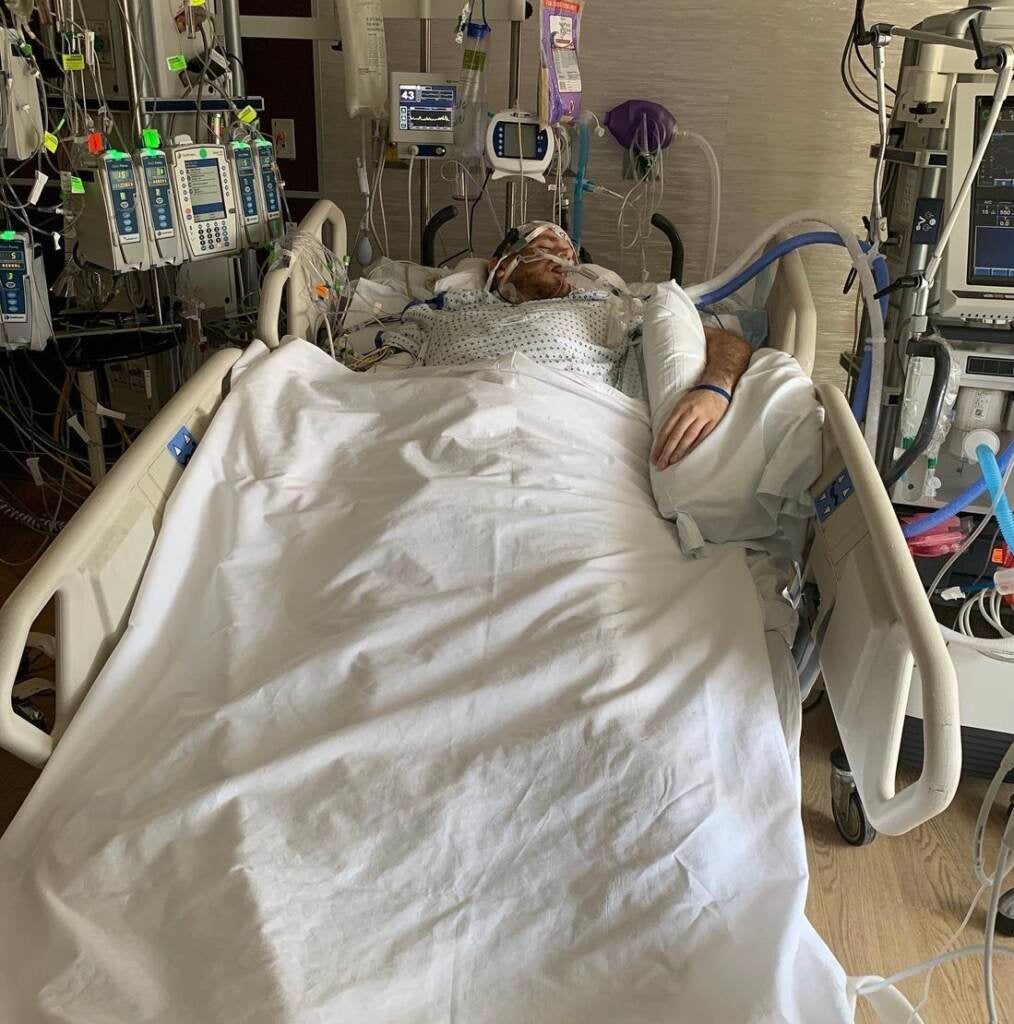
Chris stayed in the hospital for weeks. At first, his doctors thought that if he could regain enough strength, they’d be able to wake him from the coma — but that hope began to wear thin as Chris’ health declined.
By December, Chris’ doctors proposed two options to his family: Chris could be added to the heart transplant list and wait for a new heart. Or they could implant a left ventricular assist device onto Chris’ heart, also known as an LVAD.
Most LVAD patients don’t have a pulse with this device. Still, it can keep them alive for up to six years, according to Abbott — the company that develops the newest LVAD model, the HeartMate 3.
The device is small and functions easily. It looks like the cap you would fasten on a vehicle gas tank. It is surgically implanted on the left ventricle’s bottom section, forcing the heart to contract and pump blood to the rest of the body.
The device is battery operated — meaning the LVAD is connected to a battery outside of the patient’s body with a cord. These batteries can last up to 16 hours. Most patients are given extra batteries to switch out when needed, and they usually carry the battery and its case in a backpack that they wear all day long.
Essentially, the device becomes one with the patient.
Before Chris’ coma, he had no interest in becoming one with any device. But Meghan and his family decided that waiting for a heart transplant would be too risky. Chris’ family decided to go the LVAD route.
His doctors intended to implant the device in December. Chris had to be pretty healthy to endure the surgery without complications because, awake or not, he was still very ill.
And Chris’ health took a turn for the worse when he got pneumonia a few days before Christmas.
“It was the first time I think I cried the whole time for him,” Carter said, “because they thought they missed the window, and I didn’t know what they were going to do.”
Two days after Christmas — Chris’ doctors decided to schedule the surgery. The procedure lasted a few hours. Chris was still pretty fragile, and his doctors wanted to ensure the device worked properly; therefore, he stayed in the coma for an additional two weeks.
“It was crazy,” Donges said. “I remember one of the first things I asked was like the day or time, or that was like one of the biggest shocks to me was going to sleep in December and waking up in January. And like, I started crying because I missed Christmas, I missed New Year.”
Life with a device
Chris’ surgery was a success, but his road to recovery was far from over. He had forgotten how to use the rest of his body. He couldn’t flex his hands, walk, or talk when he first woke up.
His next steps were to start physical therapy at Good Shepherd Rehabilitation in Philadelphia. He participated in exercises like walking around a parking lot or gripping objects.
While Chris was taking his not-so-first steps, Meghan was learning how to be his caregiver.
“They gave us this full binder of information about the HeartMate 3 and how certain alarms would go off,” Carter said.
Because the LVAD is situated inside of a patient’s body, its exit site is considered an open wound that needs to be carefully cleaned one to two times a week. This process is called the dressing change, and it is the most critical part of using an LVAD.
“The biggest concern in that area, since it’s an open wound technically, is the risk of infection, Donges said. “So with those dressings, we roughly change them about once a week. It took some time, but we’ve gotten into a very good groove.”
Chris finally returned home on Valentine’s Day. His family and friends welcomed him home with a grand dinner — and the couple continued physical therapy at home for the next few months. The homecoming was bittersweet. Meghan was excited to have Chris home, but she was also worried about his progress.
“I didn’t really know what his limitations were,” Carter said. “He didn’t know what his limitations were. So, I really just took everything with a grain of salt. I’m just like, ‘OK, what do you feel like doing today?’”
By April, Chris could walk up and down the staircase at home. Even simple tasks like reaching for the TV remote were stamps of progress. Their hard work and patience had finally paid off, and now they wondered if their homebound training could be of good use outside their home.
Although about 250,000 people in the U.S. have advanced heart failure, Meghan said there is little information online about how to live with the LVAD — and travel with it.
So, they decided to sort of be the guinea pigs of this small community. They began an Instagram feed called Life with a Device. The page documents their adventures with the LVAD and helpful information about the device.
The first trip they documented was an impromptu visit to Disney World in Orlando, Florida.
“Disney is just a happy place for adults, children,” Carter said. “It’s just a happy place. And with the help of others, I was able to surprise him.”
But getting to Disney proved to be more difficult than they had imagined. For example, a bomb technician stopped Chris in the Philadelphia Airport. The technician had never seen an LVAD before.
“So, they ran their different tests,” Donges said. “He had these swabs and stuff. He was amazing. But you get a little intimidated when a guy comes up [to you] with bomb technician on his shirt at the airport. And you have these people looking at you.”
Chris and Meghan said they laugh about the incident now.
Today, after living with the LVAD for three years, Chris has gotten the hang of traveling with the device. He is extremely grateful that he went the LVAD route. He says life has gotten better. Chris and Meghan welcomed a baby girl named Logan into the world, and the couple got engaged.
Chris also serves as an ambassador for Abbott — helping potential LVAD patients make the best decision for them. He is not on the heart transplant list because some patients with this condition recover over time. Chris is still young and hopes his heart will regain the strength to pump blood without the device. Until then, he’ll use the LVAD and live life to the fullest.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.







