Amputees rely on clinics to fit them with prostheses. What happens when a manufacturer owns the clinic?
For the first time, prosthetics manufacturers in the U.S. also own clinics that can recommend their products to patients.
Listen 12:06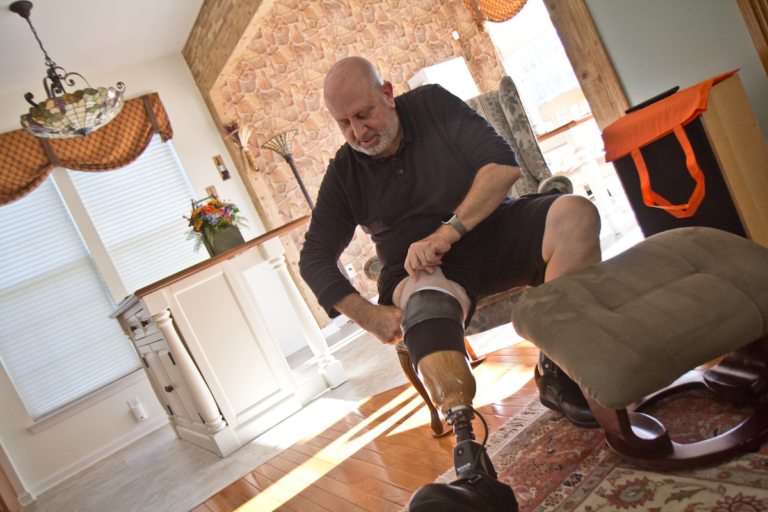
Ed Nathan pulls up the liner, socks he uses to protect his leg from rubbing, and the compression sleeve of his prosthetic limb. (Kimberly Paynter/WHYY)
This story is from The Pulse, a weekly health and science podcast.
Find it on Apple Podcasts, Spotify, or wherever you get your podcasts.
In 2010, when Ed Nathan was in his 50s, a muscle at the back of his calf locked up. It meant that his ankle couldn’t move properly, but Nathan kept walking on it.
“[It] basically turned the bones of the ankle into gravel,” Nathan said.
Nathan has a rare disorder that damages the nerve connecting his brain and spinal cord to muscles and the cells that detect pain. He broke his ankle and didn’t know it. He didn’t feel the pain and it was too late for his ankle. Doctors told him they could try to repair the ankle, but it would never work well, and he would still be in pain.
Nathan decided to amputate and live with a prosthetic limb.
Finding the right prostheses takes time and research.
“When you’re at that point where you’ve just lost a limb or worse, it’s like drinking from a firehose; there’s just so much information coming your way,” Nathan said.
A prosthetist guides patients through that process and helps them find a prosthesis that suits them. For instance, people who want to be active and run on a daily basis would get a different kind of prostheses than someone who mostly walks around their home.
Nathan says the patient-prosthetist relationship becomes personal.
“Changing prosthetists is emotionally difficult unless you’re having a problem with the one you’re leaving … I know people whose prosthetists retired and they’re at wit’s end where to go because nobody else knows their case that well.”

A few years ago, Mary White lost a leg in a motorcycle accident. Her orthopedic surgeon told her she had to find “a prosthetist who can hit the bullseye every single time.” She lives in a rural part of northern New Hampshire and drove for hours to try out several prosthetists. The one that finally fitted her with a comfortable prosthesis is four and a half hours away.
“It’s worth every minute in the car to get there,” White said.
Given how much patients value their relationship with their prosthetists, some worry what could happen with a recent industry-wide change in the U.S.
The two dominant prosthetic manufacturers globally are Ottobock and Össur. Both have bought clinics in the U.S. in recent years, including the one that Ed Nathan goes to.
A large prosthetics manufacturer in the U.S. has not owned a clinic before this, even though this has already happened in some other countries like Germany and France. The number of people affected is also increasing, as some COVID-19 cases lead to blood clots that cut off blood flow to limbs and require amputations.
“If all the small practices get gobbled up by these large prosthetic manufacturers, I’m concerned that amputees are going to be at risk of becoming square pegs that are forced to fit into round holes just because this is what they want to recommend as a prosthetic system. And it doesn’t always work,” White said.
Ed Nathan has been a patient at Ability Prosthetics and Orthotics for years. He said he trusts them when they assured him the change in ownership would not change their clinical work.
“So I’m not worried about them. It’s the next generation that don’t have this sense of ownership and they’re just coming out of school. But they didn’t build the business. They don’t have an emotional stake in the business.”
Subscribe to The Pulse
Jeffrey Brandt, founder and chairman of Ability Prosthetics and Orthotics, said there is “only upside for patients.”
He said being owned by a manufacturer gives the company access to more resources, and a larger network of clinics across the U.S and the world. He said it means his employees can provide better service by learning from more clinics. He can talk about setting up a residency program for students learning to be prosthetists, and he can give his employees more options to advance if they want to step out of clinical work to be more of an administrator or manager.
I contacted Ottobock, the manufacturer that bought Ability Prosthetics, several times. After our initial exchange, they did not get back to me for an interview.
Clinics in the U.S. take these deals for business reasons, explained Eve Lee, executive director of the American Orthotic and Prosthetic Association, which represents prosthetic clinics and manufacturers.
“What is driving this is more of a business function … a growth in the industry, in the profession, and the patients that we serve.” Lee said. “In order to continue to be a viable profession, growth has to occur.”
Prosthetists used to make custom devices in their own small full service shops — make the new limb, fit it, and maintain it.
But these days, prosthetic devices are more sophisticated. Clinics need to order a lot of different parts that require clinical trials and research before a patient can get them. That sophistication also makes it more expensive and complex to run a clinic now versus a few decades ago.
It’s harder for a clinic to stay in business now than it used to be, even compared to a few years ago, said Wendy Beattie, assistant professor of physical medicine and rehabilitation at Northwestern University. Over the course of her career, she has both worked with prosthetics manufacturers on design and practiced at a clinic for more than two decades.
“It’s not enough to provide fabulous patient care if you can’t keep the doors open and the lights on,” Beattie said. “Reimbursements have decreased … meaning that the money that we get paid from the insurance companies, primarily Medicare, and our costs have only increased.”
“Manufacturing costs have skyrocketed because the cost of shipping, the cost of workers have all skyrocketed in the last few years. I think it’s much harder for an individual private practice to be financially stable.”
So, on the one hand, Beattie said, a clinic that is part of a much larger network has a lot more power to negotiate better deals for patients, when it comes to buying parts or insurance payments. However, she also said if patients and clinicians, “are going to have less options regarding what they can fit patients with, I view that as a concern.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.







