Chemo drug shortages lead to treatment changes, anxiety, and fear among patients
After Mairead McInerney was diagnosed with an aggressive form of breast cancer, ongoing drug shortages forced her treatment plan to be more grueling than she expected.
Listen 12:17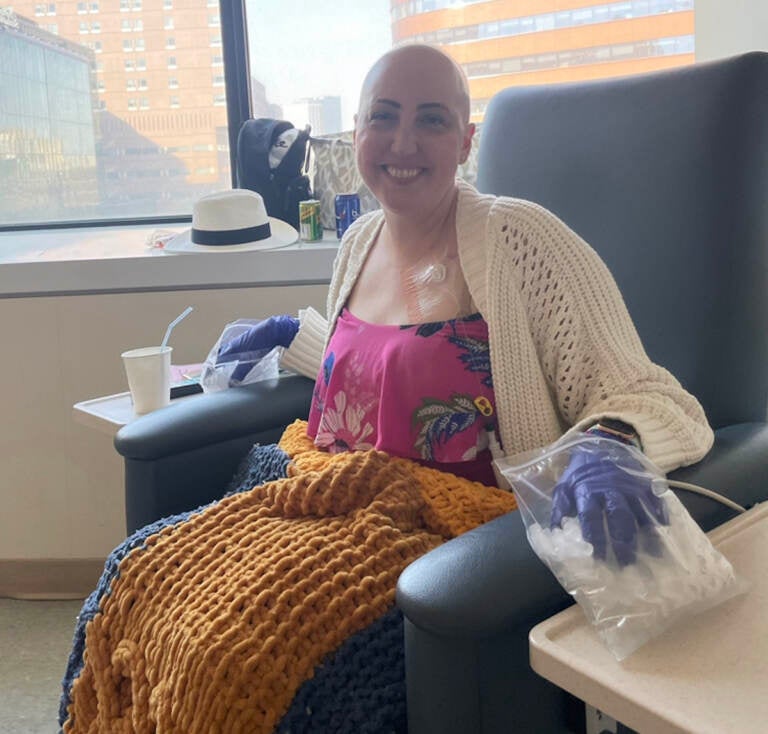
Mairead McInerney endured an arduous chemotherapy plan after ongoing drug shortages affected her treatment protocol. (Courtesy of Mairead McInerney)
This story is from The Pulse, a weekly health and science podcast.
Find it on Apple Podcasts, Spotify, or wherever you get your podcasts.
In December 2022, Mairead McInerney suffered a miscarriage in her 11th week of pregnancy. From there, it was a shockwave of more bad news.
McInerney had also developed a hard lump in her right breast, which she had first attributed to her pregnancy. She decided to get a mammogram and ultrasound, and the lump turned out to be stage three triple negative breast cancer, which is aggressive.
McInerney and her husband tried to process everything that had just happened.
“Here we were in the midst of grieving the loss of our child, sort of wrapping our arms around this aggressive diagnosis,” recalled the Ambler, Pa. resident.
Her treatment team at Pennsylvania Hospital mapped out her chemotherapy plan.
“I still remember sitting there as my oncologist drew out this map. And that map to me almost looked like a marathon. I’ve never run a marathon, but looking at that map, I was like, ‘Oh, my gosh, this is going to this is going to take a long time.’”
Then she received more bad news. The oncologist wasn’t going to be able to follow the standard protocol for her type of cancer because one of the chemotherapy drugs she needed was not available.
“So what he did instead was to flip the protocol. And so it’s been done before and in other places. However, I was his first patient for him to do this,” said McInerney.
She said the pivot meant starting with the hardest part of the chemo protocol.

“So I dove right in. I lost my hair within one week, post the first round of treatment, and it really knocked my blood cells down. My body was really depleted from my white blood cell count.”
As McInerney progressed with her chemo, she started to look forward to the end of her treatments. Then she learned there was another shortage that meant her treatment had to be changed once again. She said the experience was exhausting and stressful.
“It really really rocks you because the cancer’s been out of my control, and now potentially medication is out of my control. And to see your oncology team struggle, because they’re the ones to have to bear these messages, but they’re not in control of this either, that’s heartbreaking, because you know that they’re also feeling helpless with you.”
McInerney worries that the changes in protocol will affect her outcomes and long-term recovery.
“I know we made the best decision with the information and the resources we had at the time,” she said, “but this is still a very new disease. And so the research being done on it is still very new, and I am worried.”
As a licensed clinical social worker, she said she has a lot of coping skills to deal with the persistent anxiety all of this has caused, but it has still taken a massive toll on her. She said that’s true for other patients in her situation.
“It impacts our nervous system, and if you think about it like a glass of water, we keep being filled to the top. And with this type of anxiety, you start spilling over. And here we are to be really focused on healing,” she said. “It really should just not be something that we have to worry about and it should not be something that the physicians have to worry about.”
Subscribe to The Pulse
What’s behind the shortages?
Drug shortages are affecting a lot of people now — from cancer patients like McInerney to people who are trying to fill their Adderall prescription to cope with ADHD. There are also antibiotics and treatments for diabetes that are short in supply.
Clinical pharmacist Erin Fox is the associate chief pharmacy officer at University of Utah Health, a big health system headquartered in Salt Lake City.
She explained that she defines a shortage as when a hospital or pharmacy has to change the way they prepare or dispense a drug because they cannot get the drug they would like to use. This could include changing a patient’s dose, using a completely different drug, or even deferring treatments and delaying procedures.
Fox has been documenting and tracking drug shortages for over two decades, and has seen several serious ones.
“For me, it’s a bit of a Groundhog Day,” she said. “We are in a very similar place to where we were in 2012, 2013 with a lot of oncology drug shortages at the same time. So it’s frustrating to see this happen again for the same reasons.”
She said right now, they’re at a 10-year high in terms of drugs they are tracking that are short in supply, and that it is a bit of a mystery why drug shortages happen.
“Honestly, with most shortages, we don’t have good information, usually, about what is happening. Part of that is because drug companies are not required to publicly tell their patients or their customers exactly what’s going on. They’re allowed to keep it a secret.”
Fox said sometimes it’s staffing problems, extreme weather events that cause damage at a manufacturing plant, or quality control issues. But the whole system is very opaque. Even the people purchasing drugs for hospital systems or pharmacies don’t have much information to go off of.
She added that the worst shortages usually happen with injectable drugs that are used in hospitals and clinics, like with chemotherapy and generic drugs. When hospital systems or pharmacies purchase generic drugs, the only point of information they have is price, said Fox.
“That’s because the FDA rates those products as equivalent. But also the [drug] companies don’t disclose additional information about, maybe they might be doing a better job at quality or redundancy. They might have backup methods to make sure that they never have a shortage. So those companies are not competing on those other factors besides price. And so, unfortunately, these companies undercut each other in price and it’s a race to the bottom.”
She said to imagine shopping on Amazon, but you have no information on a product other than price: no ratings or comments from other shoppers.
Fox said the FDA does provide some information around issues affecting drug production, but it’s very limited. For example, they will post warning letters around bad inspection reports at drug manufacturers, but they are heavily redacted.
“So say you read a warning letter and you think, ‘Oh, I don’t want to buy any drugs from that factory. Let’s not have those at our clinic. Let’s not have those at our hospital.’ It’s impossible to do that because the list of products that are made at that factory is not available. It’s considered to be a trade secret.”
Fox supports a new proposal from The Brookings Institution — a three-pronged approach to addressing and preventing drug shortages in the US. It would allow for generic drug companies to compete on more than price. It would create pathways to ensure hospitals are able and willing to pay more for quality products. And it would ensure that drug manufacturers allocate resources to update and improve their facilities and focus on quality. She said those three things would make quality information more transparent.
“[That] should incentivize those manufacturers to improve quality … Hospitals are already paying more for shortages right now with labor and other costs. This way they would just pay a little bit more and actually get the drugs they need.”
Fox said while it’s frustrating to see this drug shortage unfold, something she calls a public health crisis, she is seeing the issue get more attention than ever before.
“We’ve already had two hearings on drug shortages so far this year,” she said. “And so I’m really encouraged by that. Where we’re at right now is the best it’s been. So I’m optimistic.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.