Pa. coronavirus recovery: State and Philly Health Depts. urge caution amid surge in cases
Consider canceling family holiday gatherings, says Philly Health Commissioner Farley. Be mindful of flu season, state Health Secretary Levine says.

Pennsylvania Health Secretary Rachel Levine. (Commonwealth Media Services)
Updated at 4:20 p.m.
The Pennsylvania Department of Health reported on Tuesday 2,751 additional positive cases of COVID-19, bringing the statewide total to 198,446, with a total of 8,696 deaths since the coronavirus pandemic began. Daily increases are now comparable with what was seen in April, the department said, and today’s increase is the largest daily one to date.
Philadelphia’s Department of Public Health reported 340 additional positive cases Tuesday, bringing the number of confirmed cases to 42,924. Five additional fatalities were confirmed in Philadelphia, for a total of 1,864.
In Philly, higher case numbers but lower death rates
Case rates are up in Philadelphia and everywhere else, city Health Commissioner Dr. Thomas Farley noted Tuesday.
“There are all-time highs in daily case counts for Pennsylvania as a whole and for the United States as a whole,” he said. But there’s good news, too: The city is seeing fewer deaths for every case identified than it did in the spring.
In April and May, Philadelphia saw one death for every 15 cases reported; this fall, the rate is much lower, at one death for every 60 cases. That’s partly because the health care system is finding more asymptomatic or mild-symptom coronavirus cases, as testing availability increases; it’s also because hospital treatment appears to be improving, and because positive cases tend to be in younger people who are less at risk of death from the virus. It might also be linked to the unconfirmed theory that widespread mask wearing can decrease case severity, said Farley.
Still, the commissioner urged caution amid rising case counts, and noted that future city policy decisions would be based on those counts as well as hospitalization and death rates.
City officials recommend canceling holiday plans
As cold weather approaches and Philadelphians retreat indoors, the coronavirus might follow a similar pattern as other respiratory illnesses like the flu. “With that in mind, we anticipate further rapid increases of this infection in Philadelphia,” said Farley, “which means we’re entering a difficult, dangerous period of the epidemic — possibly the worst period of the entire epidemic.”
The city plans to increase testing availability by opening a small number of additional testing sites, and will no longer be reaching out to every individual positive case in contact-tracing efforts. Rapid testing will be more readily available as well, Farley said.
Something the commissioner does recommend: canceling holiday gatherings.
“We’re not going to get past this epidemic by Thanksgiving, or by Hanukkah, or by Christmas,” Farley said Tuesday. “Family gatherings right now are simply very dangerous … these are not normal times.”
Gathering with anyone not in your immediate household, Farley said, could potentially spread the virus.
Philly schools continue hybrid learning
The Pennsylvania Department of Education recommends remote learning after a threshold of either 100 cases per 100,000 population over a seven-day period, or 10% positive community case rate. Philadelphia barely reached the first threshold this past week, Farley said, but has not reached the second.
Given the rate of community spread, the city’s schools are not currently required to offer remote learning. That may change if cases continue to rise.
As cases signal fall surge, state officials urge caution
With daily case increases now paralleling the spring surge of the COVID-19 pandemic, numbers may indicate another wave of rapidly spreading coronavirus cases.
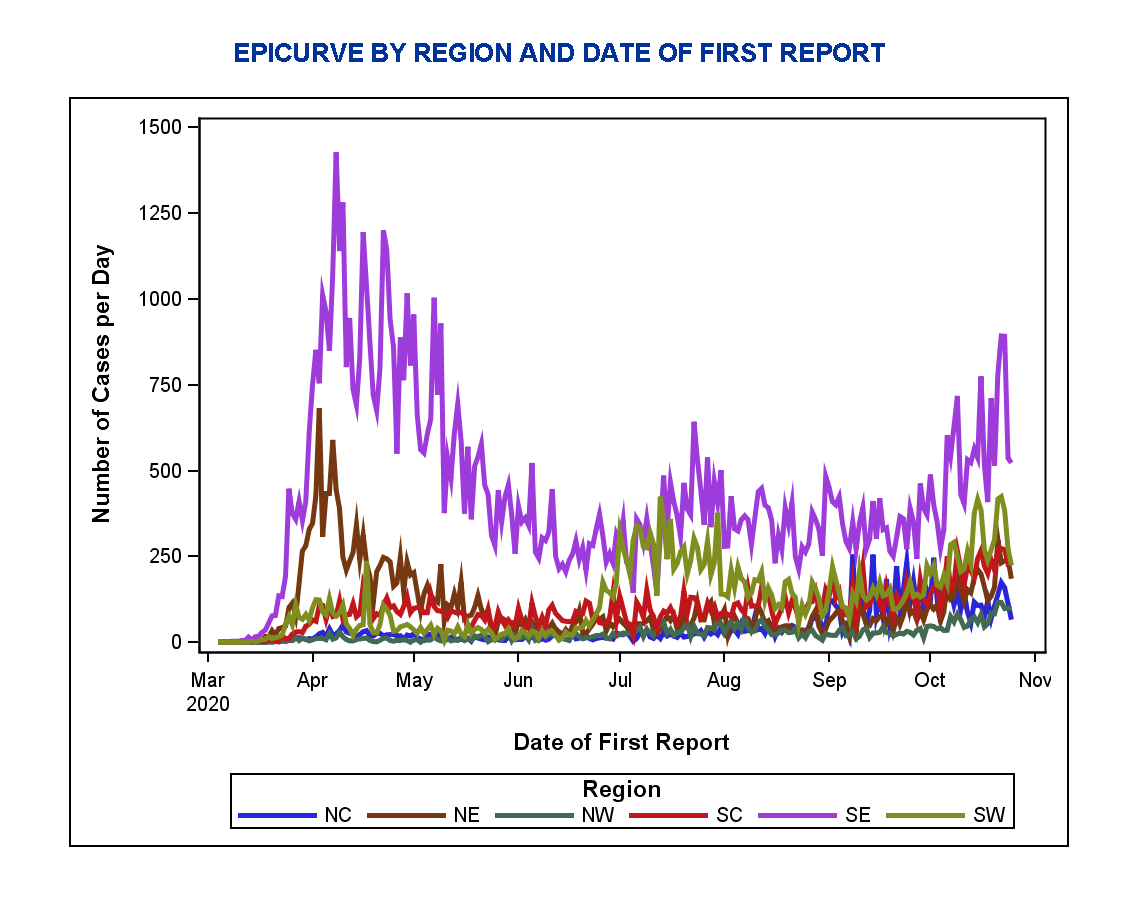 The state’s health care systems are now better prepared to address the virus than they were earlier this year, Health Secretary Dr. Rachel Levine has pointed out. But she said in a release Tuesday that Pennsylvanians “must all do [their] part” to prevent a rise in hospitalizations as cold weather and flu season approaches.
The state’s health care systems are now better prepared to address the virus than they were earlier this year, Health Secretary Dr. Rachel Levine has pointed out. But she said in a release Tuesday that Pennsylvanians “must all do [their] part” to prevent a rise in hospitalizations as cold weather and flu season approaches.
Gov. Tom Wolf’s administration has encouraged Pennsylvanians to hand-deliver mail ballots immediately, reiterated guidance on hand-washing and mask-wearing whenever possible, and updated a list of travel recommendations for state residents returning from other states. Officials are also asking that residents download the COVID Alert PA app to make exposures more easily trackable.
Pa.’s outbreak plan for nursing homes
Most long-term care facilities aren’t set up to deal with the effects of a pandemic, particularly one that disproportionately affects immunocompromised and elderly populations. That means that when COVID-19 outbreaks occur, the effects can be rapid — and deadly.
The state’s Regional Response Health Collaborative is intended to coordinate clinical, operational, and educational support to long-term care facilities facing coronavirus outbreaks. In Southeastern Pennsylvania, that support is provided by medical experts from Penn Medicine, Jefferson Health, and Temple Health.
“When a facility is identified at risk or has positive test results, we are notified to do a rapid response mission to identify what the facility might need,” Kristen Vogl of Jefferson Health said in a press call Tuesday. “A rapid response consists of quickly assembling subject matter experts from across Jefferson to address key areas, whether it’s infection control and prevention, PPE, or behavioral health.”
“Each facility is extremely different, there’s no two that are alike … it really takes a lot of time to figure out what the needs are,” said Laura Porter of Penn Medicine.
Every day at 10 a.m. and 3:30 p.m., leaders from the Regional Response Health Collaborative, the Pennsylvania Emergency Management Agency and the Department of Health meet to discuss requests for resources, COVID-19 facility cases, and other support needs. Combined, the agencies can provide a level of support that the long-term care facilities couldn’t match on their own: testing capacity, a response team of trained medical experts, and more.
But that support could go away. The program is set to expire Dec. 1, although state Human Services Secretary Teresa Miller said her department is trying to extend it until the end of 2020, and is working with federal partners to allocate additional funding so that support for the collaborative can last as long as the pandemic does.
“This program could disappear just as it’s needed most,” Miller said. “It’s strengthening our response and our preparedness for COVID, it’s keeping people safe, and it’s saving lives … we’re now at a point where we have a system that’s working [and] we cannot lose this resource.”
It’s become clear that the pandemic will not be over by the time the funding expires. And if the program does end, it’s unclear what state support for long-term care facilities will still exist.

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.




![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)