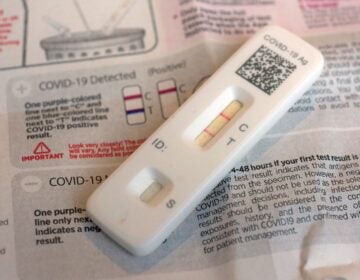
Scarcity of coronavirus testing, lack of demographic data could hamper Pa.’s efforts to reopen parts of the state
Pennsylvania lacks key information about the coronavirus outbreak due to the continued scarcity of testing and a systemic failure to gather patient data from tests.

(Tim Tai/The Philadelphia Inquirer)
This article originally appeared on Spotlight PA.
–
Pennsylvania lacks key information about the coronavirus outbreak due to the continued scarcity of testing and a systemic failure to gather patient data from tests administered so far, shortcomings that could hamper the immediate response and later efforts to reopen the state.
In order to understand how COVID-19 works and how far it has spread, health experts say more people need to be tested, including those not in high-risk groups.
Even for those who have been tested, the state doesn’t have complete and reliable demographic data needed to inform how resources should be deployed, such as the number of tests performed in any given county, or the age, gender, and race for all of those who’ve been tested.
“It’s like flying blind,” said Ezekiel Emanuel, chair of the University of Pennsylvania’s Department of Medical Ethics and Health Policy. “It’s critical to know where you need to concentrate your resources and what people are experiencing.”
After significant strides in late March and early April, as private health systems brought tests online, the number of tests administered per day plateaued at about 7,000 this week, according to state data. In total, Pennsylvania reported 113,019 tests completed as of Friday, which represents less than 1% of the state’s population of 12.8 million.
Experts say that’s not nearly enough testing capacity to be able to make informed decisions about allocating resources or to begin reopening the state in a measured way. Scaling back social distancing will rely on a robust testing framework — both for people who actively have the virus, and those who have recovered and may have antibody protection.
Number of new coronavirus tests reported daily
A look at Pennsylvania’s testing capacity since March 6, 2020.

Donald Burke, an epidemiologist and former dean of the University of Pittsburgh’s Graduate School of Public Health, said Pennsylvania would need to increase its testing tenfold in order to answer key questions about the disease and its trajectory.
“We’re going to have to live with this epidemiological purgatory where we have some disease but not too much and where we have some social distancing but not too much,” Burke said.
The lack of testing among low-risk groups means there’s very little data about what percentage of the public is infected but not experiencing symptoms. The fear is that those people could unknowingly infect many more, which is why Gov. Tom Wolf has shut down much of the state’s economy and ordered all but essential workers to stay home until the end of April.
Without reliable data on infections, Burke said it will be difficult to make informed decisions about when and how to scale back social distancing, and, later, when to ramp it up again for an anticipated second wave in the fall and winter.
Increased and better testing needs to be in place at least by the summer, he said.
The state recently drew scrutiny for being unable to release the racial makeup of COVID-19 cases, saying that data had not been consistently reported to it by health systems.
Nate Wardle, a spokesperson for the Department of Health, said the state also lacks key demographic data about the age, gender, and underlying health conditions of people tested for the coronavirus. Hospitals report information on the age of COVID-19 patients at their facilities but laboratory data — where the vast majority of testing takes place — is often incomplete.
Wardle said physicians provide information on patients to labs when they perform a test. But the labs, in turn, do not always provide the same information to the state.
“This is not a COVID-19 specific issue,” he added.
While Wardle said the state is “looking at a number of different options to get us to have access to demographic data,” it’s unclear whether the information can be obtained retroactively.
But this isn’t just a problem for the state Department of Health.
Emanuel pointed to Centers for Disease Control and Prevention data that similarly lacked key information, such as age, gender, and race. Of the first 4,226 coronavirus cases the CDC reported, a third lacked information about whether the patient was hospitalized. Nearly half lacked information about whether the patient lived or died.
In Philadelphia, the city’s health department had racial data for just a fraction of cases and vowed to begin collecting more information about those who are tested.
Councilwoman Helen Gym said that is important to understanding disparities such as why the city’s wealthiest zip codes tended to have the most testing. Positive cases there may reflect greater health care access rather than the actual spread of the disease, she said. And, she said, lower-income residents are less likely to be able to work from home and avoid close contact.
“It’s not enough to give us aggregate data because it doesn’t tell you anything,” Gym said. “It creates a disproportionate sense of who is impacted and, thus, where resources should be allocated.”
Despite the ramping up of new testing locations statewide, it’s still difficult for people who believe they may have been infected to know for sure. And that uncertainty, health experts say, increases the likelihood that COVID-19 will spread undetected both now and in the future.
Marlise Yameogo, a 19-year-old college student from Steelton, said she did all the right things when she came down with symptoms of COVID-19 two weeks ago: She self-isolated, went to an urgent care center, and even sat outside in her car waiting to see a nurse.
The nurse told her she didn’t meet criteria for a coronavirus test even though she had shortness of breath, a fever, and a severe headache that kept her up at night. And a testing facility told her she needed a referral.
“Talking is a little bit complicated,” she said Monday, after taking a moment to catch her breath. “I’m very tired. Very tired. It’s like I have to stop, take a breath, wait, and start again.”
Yameogo finally got a referral to get tested on Wednesday. A nurse she spoke to via remote video told her that it would take the lab a few days to schedule an appointment and that she would have to drive an hour and 40 minutes to Williamsport.
Meanwhile, her 52-year-old mother has started exhibiting mild symptoms and her brother, a cross-country truck driver who was not symptomatic, is back on the road.
“I didn’t want him to go back out because he might have been exposed,” Yameogo said. “I just don’t know.”
Ebbing Lautenbach, a professor of epidemiology at the University of Pennsylvania, said it would be ideal to test a wide swath of people, including those with no symptoms, and to collect as much information about those people as possible.
But because of very real limitations in testing capacity, he said, it’s reasonable for providers to target at-risk groups.
“Unfortunately, there are a lot of questions we don’t have great answers for,” he said. “But we will. It’ll just take more time.”
So far, the focus has been on diagnostic tests that show whether a person has the virus. Those will remain an important part of helping the state track the virus and responsibly roll back social distancing. In Japan and Singapore, for example, officials saw recurrent waves of infection after local outbreaks were thought to have waned.
The state has not released a breakdown of how many tests are conducted in commercial labs, but is “in active discussions” on releasing additional data, Wardle said. At the moment, the state lab in Chester County can test 300 samples per day versus the recent daily average of 7,000 new tests being reported.
Burke said it’s almost certain that many COVID-19 cases went undetected.
Testing priorities could soon shift toward detecting antibodies in addition to the active virus as another part of the strategy to allow certain people to safely go back to work.
In theory, Burke said, individuals who have been exposed to the virus have a certain level of immunity, though the extent of that protection is still somewhat unknown. This week, officials in Chester County announced a plan to administer antibody tests to 10,000 emergency response, health, and long-term care workers as a way to inform safe staffing procedures.
But as Yameogo’s case shows, getting even a diagnostic test remains an arduous task.
While some of her symptoms have dissipated — she doesn’t think she has a fever anymore, although she doesn’t own a thermometer — she’s now suffering from chest pains in addition to a headache and shortness of breath.
She planned to give the lab in Williamsport a few days to get back to her and go to an emergency room only if her condition worsened.
“You don’t know if the road you’re taking is the right road,” she said. “There’s no clear steps. You just got to guess. You call all these people and they don’t know. It’s too much work, especially for someone who’s not feeling very well.”
100% ESSENTIAL: Spotlight PA provides its journalism at no cost to newsrooms across the state as a public good to keep our communities informed and thriving. If you value this service, please give a gift today at spotlightpa.org/donate.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.




![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)