Planning to test and travel for the holidays? It might be trickier than you think
Which test should you go for? Can you even schedule one? How long should you isolate before your test, and afterward? There’s a lot to consider.
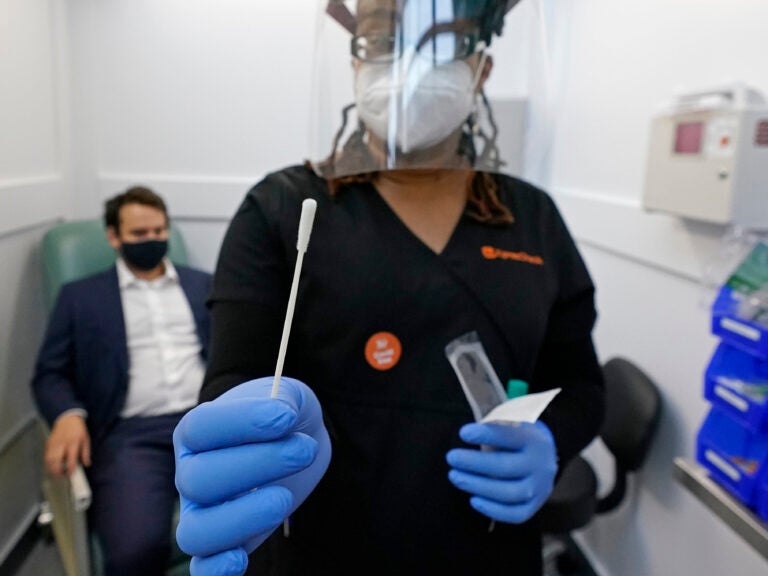
A medical assistant holds a swab after testing a man on Wednesday at the new COVID-19 testing facility at Boston Logan International Airport. (Elise Amendola/AP Photo)
The national spike in coronavirus cases means more Americans may be staying home for the holidays this year.
The Centers for Disease Control and Prevention issued a strong recommendation to avoid Thanksgiving travel, and city Health Commissioner Thomas Farley has been pretty clear that he concurs.
“Cases are surging in Philadelphia,” Farley said on WHYY’s Radio Times Wednesday as he urged people to “please” celebrate Thanksgiving with immediate household members only. “Getting together over a meal right now is very dangerous.”
Other public health experts are already recommending similar precautions for the entire holiday period.
Whether you’re determined to go or still undecided, here’s what you need to know about traveling and testing — and about assessing the relative risks involved.
Schedule a test well in advance of your trip
In the last week, the Food and Drug Administration approved emergency use authorization for a prescription-only, entirely-at-home test, but that’s not yet widely available. In the meantime, some places in the region require a doctor’s referral for testing, which you can get by contacting your primary care provider. Other test sites don’t require a referral but do ask that you schedule an appointment, usually online or over the phone. The few spots that don’t require appointments or proof of symptoms have been swamped in recent days, so either go early or be prepared to wait.
You might have to wait after the test, too. Facilities managed by Penn, Jefferson, Temple and Children’s Hospital of Philadelphia process their results at local labs, as Billy Penn reported earlier this year, which means a faster turnaround. But most urgent care facilities, pharmacies, and community testing centers send samples to be processed at national labs such as LabCorp, Quest and Bioreference. Since the country’s surge of COVID-19 cases means higher test volumes at those national labs, sites that use them might take longer to deliver results.
Then there’s this question: Which test do you go for: The lab-sample PCR (polymerase chain reaction) or the rapid-result antigen?
“Information on testing continues to evolve, [and] there’s multiple types of antigen and PCR tests out there,” said Vybe Urgent Care president Peter Hotz. Vybe offers both, but “the antigen test has a slightly higher false-negative rate … which is why we’re predominantly using antigen testing [for] larger-scale, faster-turnaround, lower-cost testing.”
A false negative would indicate you don’t have COVID-19 when you actually do. That’s why “the gold standard is the PCR test,” said Susan R. Weiss, a microbiologist at Penn who studies coronaviruses. The experts WHYY News consulted agreed: Ask which test you’re getting before you go, and if you have the time to wait, a PCR test usually provides a more accurate result.
Increase your likelihood of an accurate test
If possible, quarantine for several days before testing — it increases the chance that your test will be accurate.
On average, it takes four to five days after infection for the SARS-CoV-2 virus to start replicating in your body at a rate that can be detected by the test … sometimes even longer, since the coronavirus’s incubation period can last up to 14 days. That means if you were exposed to the virus a day or two before testing, you could test negative and still develop symptoms a few days later.
So the best way to ensure an accurate result is to isolate and wait.
“[Both] antigen and PCR tests don’t pick up cases very well on the second or even the third day after infection; it’s never perfect, but in those early days after infection, they miss a lot,” said Penn biostatistician and epidemiologist Michael Levy. “If you can quarantine for three days or four days and then get tested, that’s probably the best strategy. If you can quarantine even longer, that’s better … the more you can stay away from contacts, especially inside, that’s the safest thing to do.”
Some doctors recommended waiting for two to three days, others recommended three to five, and at Weiss’s lab, they asked exposed workers to wait six days. But all the experts interviewed for this article agreed that the wait time before testing is critical.
“It never makes sense to me to get right off the plane and get tested by any of these techniques,” Weiss said.
Isolate after testing, too
Stay quarantined after testing and before you get your result, and be cautious about exposure afterward as well, since a negative test result doesn’t mean you won’t get infected in the following days.
Regardless of your test result, you shouldn’t travel if you have active COVID-19 symptoms, the CDC advises. If you have the option of either driving or flying, pick the former, Levy said; avoiding congregate settings, like potentially crowded airports, lowers your risk of transmission.
Stay masked up and socially distant whenever you can; that means avoiding airplane meals, Weiss added.
And plan to gather outside, if possible. It might make for a colder holiday, but the increased airflow means it’ll be a less risky one.
Most of all, understand that making any travel plans, no matter how cautious, adds an additional level of risk — not just for you and your loved ones, but for anyone you may come in contact with along your route. Every COVID-19 transmission event can lead to more, public health experts said.
“I’m going to miss Thanksgiving with my family, and I think a lot of us are,” said Levy. “But someday in 2021, I’m going to celebrate everything — it’s going to be Halloween, Thanksgiving, Hanukkah, Christmas, everything.
“And I would tell people to look forward to that everything-we-missed-day coming next year. And maybe it’ll make things easier.”

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)



