Pennsylvanians on Medicaid risk losing health coverage when COVID emergency ends
Many will lose Medicaid coverage nationwide, but Pennsylvania’s plan is out of step with other states, which advocates say will lead to greater losses.
Listen 1:53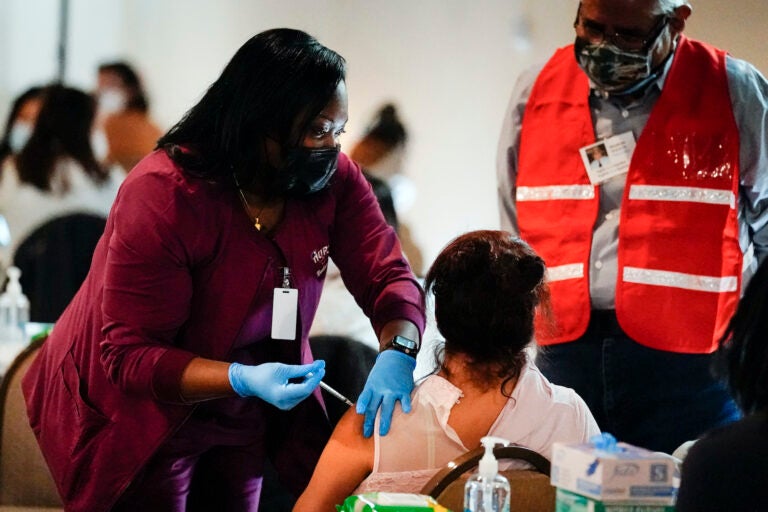
A health worker administers a dose of a Pfizer COVID-19 vaccine during a vaccination clinic at the Grand Yesha Ballroom in Philadelphia, Wednesday, March 17, 2021. (AP Photo/Matt Rourke)
The COVID-19 pandemic has changed everything. What should we know about how you approach the world now? How has the pandemic changed your social life, your work life, your interactions with your neighbors? Get in touch here.
For the past two years, people on Medicaid in Pennsylvania have been guaranteed continued health coverage — even if they’re no longer eligible.
That’s because of a provision in the Families First Coronavirus Recovery Act, which requires that states keep everyone on Medicaid as long as the country is under a public health emergency.
But that emergency status is likely ending soon — and state officials predict at least 500,000 Pennsylvanians will lose their health insurance when it does.
Under normal circumstances, people have to reapply for Medicaid each year and many end up losing coverage annually in what is known as “churn”: While some individuals lose coverage due to legitimate eligibility changes (a new salary that exceeds income requirements, or relocation to another state), studies suggest that forcing people to enroll annually leads to loss of coverage due to simple administrative and procedural issues.
“We are really, really worried about that, because when people lose their medical assistance for these procedural reasons, they are left without any access to health care,” said Maripat Pileggi, attorney with Community Legal Services in Philadelphia, who helps people appeal their denied eligibility claims.
The Biden Administration will announce on April 16 whether or not the public health emergency will be renewed, and for how long. Pennsylvania health officials said they expect one more 90- day renewal before it is terminated, meaning the requirement for continued Medicaid coverage would end in July.
The uninterrupted coverage has led to a whopping 20 percent increase in Medicaid coverage rates in Pennsylvania between January 2020 and January 2022 — a bump rivaled only by the increase seen in 2015 when Pennsylvania expanded Medicaid to include larger income brackets.
In Philadelphia, which has the largest share of Medicaid patients in the state, enrollment jumped by more than 100,000 people, from 649,812 in January 2020 to 755,385 in January 2022.
There are currently 3.5 million people enrolled in Medicaid in Pennsylvania, or roughly 1 in 4 people across the commonwealth. All of their applications will need to be recertified within the year. Of those, the Pennsylvania Department of Health and Human Services estimates there are roughly 500,000 Pennsylvanians receiving Medicaid who will be deemed ineligible based on income changes.
The recertification process is lengthy and involved. DHS workers must track people down who may have moved during the pandemic, determining eligibility through a variety of verification documents like pay stubs, referring people to a different program if they are ineligible for Medicaid, and ensuring rounds of paperwork are mailed back completed and on time.
Despite the enormous administrative burden, Pennsylvania is planning to go through all the recertifications in just six months — a time frame wildly out of step with the plans of other states across the country and which advocates say could lead to massive loss of coverage and headaches for state workers.
“We know from the past that when state agencies attempt to do too much medical assistance processing over two short of a timeframe, huge backlogs are created,” Pileggi said.
She explained that while states do their best to renew people who are eligible automatically, that often doesn’t happen. It’s common for paperwork errors to result in people losing coverage — even before the pandemic, she said, roughly half of Medicaid renewals would result in a procedural termination.
Pennsylvania is not alone in facing this problem. The expiration of the federal public health emergency means every state is facing the deluge of recertifications. According to a recent Kaiser Family Foundation poll, just seven states plan to recertify in six months or less. The remaining 41 surveyed estimated they would take between 9 and 12 months. Pennsylvania was listed as “undetermined” on the survey, but in an interview with WHYY News, DHS officials said they planned to get the job done in six months.
The Centers for Medicaid and Medicare Services recommends states take the full year allotted, and also stipulates that states shouldn’t try to recertify more than 11 percent of their enrollees each month — a threshold that DHS officials say they think they’ll clear if they hold to the six-month period.
DHS employees themselves admit that an expedited timeline will bring additional challenges.
“The more condensed the time frame is for moving through this transition, the more pressure and strain it puts on,” said Zach Sherman, executive director for Pennie — Pennsylvania’s state-based health insurance marketplace. “I think people would unnecessarily follow through the cracks, as well.”
When asked, DHS officials did not provide an explanation for why Pennsylvania was aiming to complete the task at such a clip, other than that being the time the office estimated it would take.
But there’s pressure from Harrisburg to move even faster. In February, Rep. Seth Grove (R- York) introduced a bill that would require the recertifications to be completed within 60 days.
Sherman conceded that this time frame would be very tight.
“If we had all the people coming over who will come over through this process in two months, that’s going to be a crash on our systems,” he said.
With the requirement to keep people on Medicaid, came federal funding to pay for them. That, too, will dry up at the end of the fiscal quarter when the public health emergency expires. But advocates say that’s not a good excuse to push people off too fast: They’ll end up reapplying and it will create more work for DHS workers at County Assistance Offices, the local processing centers which handle renewals. Plus, Pileggi said, clients will likely get sicker while their coverage lapses, making them more expensive for the state to treat and care for in the long run.
DHS workers doing the actual recertifications are already under strain, said Steve Catanese, president of SEIU Local 668, which represents CAO [County Assistance Office] workers. “Candidly, we’re not sure that the DHS time frame is realistic,” he said , noting that the union had already requested overtime authorized from DHS due to existing backlogs and increases in applications for a range of benefits throughout the pandemic, but that the request has been ignored. “We would expect recertification to take considerably longer, delays in benefits processing to occur, and worker stress to increase if they are not provided with the resources and support necessary to succeed,” said Catanese.
This is not the first time hundreds of thousands of individuals have been hurriedly kicked off of Medicaid. In 2011, under former Governor Tom Corbett, there was a similar rushed recertification process in Pennsylvania, leading to a significant purge of enrollees, including many children.
One option that individuals did not have in 2011 is that if they were found to be ineligible was a referral to Pennie, Pennsylvania’s health care marketplace, made possible by the Affordable Care Act. But the affordability of those plans is in jeopardy, too. If Congress lets the increased subsidies for marketplace plans lapse, more than 35,000 Pennie customers would lose an additional $250 a month.
“For a lot of folks, that amount of money on a monthly basis is really going to be the difference between being able to afford coverage,” Sherman said.
In general, that’s why having more time to process renewals is preferable to advocates like Pileggi.
“We are buckling in for what we expect will be a real deluge of new Medicaid cases,” she said.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.




![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)



