Pennsylvania could make it harder for doctors to prescribe buprenorphine
Pennsylvania Senate may tighten rules on doctors using buprenorphine.

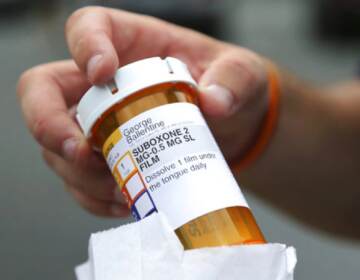
Suboxone, an oral film prescribed for the medication-assisted treatment of opioid addiction and dependency, is pictured in this Tuesday, Feb. 21, 2017 photo. (Charles Krupa/AP Photo)
The Pennsylvania Senate is considering a bill that would further regulate the drug buprenorphine, which is used to treat opioid addiction because it curbs cravings and stems withdrawal symptoms.
Studies have shown that those who take buprenorphine — also known by its brand name, Suboxone — are more likely to stay in treatment and less likely to die. But it can also be misused — technically, buprenorphine is a low-grade opioid, and there is a substantial black market for it.
Lawmakers pushing the bill say it will allow for doctors overprescribing buprenorphine to be regulated more closely, but opponents worry it will only limit treatment for patients who need it.
The bill would require that, in order to prescribe buprenorphine, physicians be licensed by the state and pay a $500 fee. Doctors are already required to be certified on a federal level by the Substance Abuse and Mental Health Services, or SAMSHA.
“Those who prescribe Suboxone/buprenorphine are able to do so through a special license from the federal government; however, they do so with no state oversight,” State Sen. Michele Brooks wrote in her February memo introducing the bill.
Neither Brooks, who represents a western Pennsylvania district, nor co-sponsor Sen. Thomas Killion, from Delaware /Chester counties, was available to comment on the bill.
The federal waiver process involves an eight-hour training and an initial 30-patient prescribing cap that many in the addiction medicine field argue is already too arduous, given the demand for treatment.
“I think that adding barriers to a process that already has too many barriers, in my opinion, is going to really cost lives,” said Jeanmarie Perrone, a professor of emergency medicine at the Hospital of the University of Pennsylvania. “We have a pretty substantial shortage of Suboxone providers, and this is undoubtedly going to add a level of complexity to new prescribers who are thinking about adding this to their practice,” she said.
There are currently 2,251 doctors in Pennsylvania certified by SAMHSA to prescribe buprenorphine.
Perrone said that although she understood the intentions of lawmakers hoping to cut down on unscrupulous prescribers, in fact the new requirements would dissuade doctors who might otherwise consider adding Suboxone to their slate of treatment.
“It might be a primary-care doctor who might say, ‘OK, I’m going to do a half-day a week of Suboxone because I know we need it in our community,’” Perrone offered as an example. “But that clinician is not going to take on that half-day a week if that includes additional levels of regulation and training that just make the whole process administratively burdensome.”
The bill would also require that patients receiving the drug be in an addiction treatment program licensed by the state. The idea is to weed out patients who aren’t taking recovery seriously and are instead selling their prescriptions on the street. But Perrone said she’s seen lots of patients do well on Suboxone without being in counseling programs.
“Many of the people who are working and taking Suboxone wouldn’t have the time to participate in a several-day-a-week treatment program,” she said. “The more we try to tell people what they need, the more we will run into people who will leave programs or therapy because they can’t fit all those requirements.”
Elsewhere, recent efforts have tended toward removing barriers to buprenorphine access, not adding them: Emergency rooms are starting people on maintenance buprenorphine after they’ve overdosed; jails and prisons are increasing access to the drug; and legislation was introduced on a federal level in Congress, proposing to eliminate the SAMHSA “X” waiver for providers altogether.
“This certainly moves in the opposite direction,” Perrone said of the Pennsylvania bill. “It needs to be a low-barrier drug, not a high-barrier drug.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.