Updated Pa. guidelines say all ERs should treat addicted patients with medication
The guidelines say all emergency departments in the state should be ready to treat patients who are already addicted with medications that prevent painful withdrawal symptoms.
Listen 1:15
Emergency Dr. Jeanmarie Perrone (right) joins Pennsylvania Secretary of Health Dr. Rachel Levine to announce new prescription guidelines for emergency room doctors dealing with opioids and opioid addiction. (Emma Lee/WHYY)
In an effort to curb opioid addictions, Pennsylvania has announced updated guidelines for doctors prescribing opioid medications in the emergency room.
The new advice reflects state law limiting opioid prescriptions for people discharged from the emergency room to no more than a seven-day supply and recommends other medications for first-line pain treatment.
“These guidelines are intended to improve patient outcomes, and to supplement, but not replace the individual physician and provider’s clinical judgment,” said Rachel Levine, Secretary of Health for the Commonwealth of Pennsylvania.
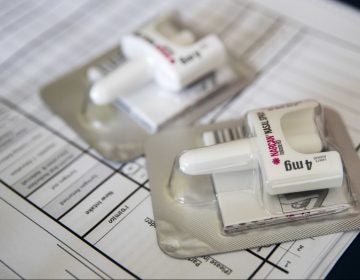
But besides looking to prevent avoidable addictions to opioid painkillers, the guidelines say all emergency departments in the state should be ready to treat patients who are already addicted with medications that prevent painful withdrawal symptoms and help people stop using illegal opioids: specifically, medications such as Suboxone that contain the drug buprenorphine.
Currently, not all emergency rooms regularly prescribe these medications when people show up there after a drug overdose.
Jeanmarie Perrone, a professor of emergency medicine at the Hospital of the University of Pennsylvania, led a committee of physicians who authored the updated guidelines.
“Everyone agreed that this was the responsibility of every state emergency department,” she said.
All hospital emergency rooms encounter at least some patients struggling with addiction, she added, ranging from people looking for help with their addiction to those needing treatment for ailments related to injection drug use. Many of them don’t go to the doctor otherwise, she said.
“So it’s really our only touch with these patients, and if we can’t be treatment ready then, then we really can’t help people,” Perrone said.
Doctors need to complete a special training course to get a waiver from the federal government that allows them to prescribe buprenorphine for patients to take home. The requirement has created an obstacle to expanding access to medication-assisted treatment in an emergency room setting.
Perrone said the University of Pennsylvania Health System was encouraging emergency physicians to get the certification by giving them time off to complete the eight-hour course and paying for the required fees. The number of them working in the system’s Philadelphia hospitals who can prescribe buprenorphine jumped from half a dozen to about 50 as a result of that effort, Perrone said, representing about two-thirds of all of the emergency physicians working there.
The guidelines were also updated to stress the importance of sending overdose survivors home with the naloxone, the opioid-overdose antidote, even when doctors can’t prescribe buprenorphine.
“We have absolutely learned in this crisis that it’s impossible for someone to get into treatment and then recovery if they’re dead,” Levine said.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.