How a Pa. health system reduced opioid prescriptions by more than half
Hospitals around the country are looking at whether patients need so many opioids prescriptions. It turns out most of them don't.
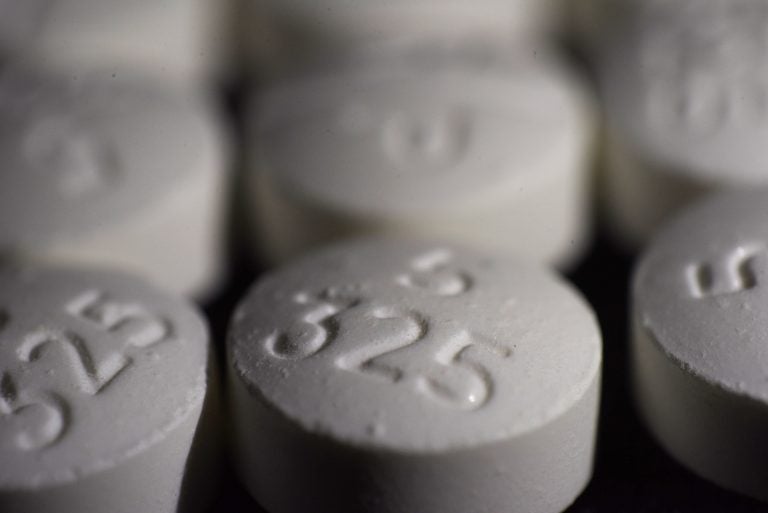
This photo shows an arrangement of pills of the opioid oxycodone-acetaminophen in New York. (Patrick Sison/AP Photo)
In 2016, more than 40 percent of opioid overdose deaths in the U.S. involved a prescription opioid.
So hospitals around the country are thinking hard about whether they should be prescribing as many opioids as they do. Geisinger, a health service organization serving patients in Pennsylvania and New Jersey, has managed to reduce its prescriptions by more than 50 percent over the past few years.
Back in 2012, Geisinger realized its patients were not really satisfied with the way their pain was being controlled. Health workers looked through the electronic database and realized that, in some cases, doctors were prescribing more opioids than their patients needed. Paradoxically, that can sometimes make the pain worse.
Michael Evans, the chief pharmacy officer at Geisinger, said the organization showed those doctors what they had found.
“And, most of the time, the reaction from the prescribers is, ‘Wow, I had no idea I was prescribing like that,’” he said.
The pharmacists worked with doctors to come up with better ways of treating pain, depending on the cause.
In cases of patients with lower back pain, physical therapy proved more effective than medication. And when doctors determined painkillers were a necessity, they went through a longer list of alternatives before prescribing opioids.
It turned out, a lot of patients didn’t need opioids after all.
Other hospitals also successfully reduced opioid prescriptions. Ten hospitals in Colorado cut the use of opioids in emergency rooms by 36 percent on average using the same methods as Geisinger: coordinating care with pharmacies and clinical staff, and developing alternative procedures and less addictive medicines.
Cara Welch, director of communications for the Colorado Hospital Association, said the plan is to expand the approach to all its hospitals before the end of the year.
That idea came from St. Joseph’s University Medical Center in Paterson, New Jersey. U.S. Sen. Cory Booker, D-New Jersey, introduced a bill last month to give out grants to hospitals and emergency departments that want to try similar programs.
Dr. Stefan Kertesz, a professor of medicine at the University of Alabama at Birmingham, said prescribing fewer opioids to people who don’t need them is a worthy goal. He said, however, there’s a bigger problem.
“Our health profession schools have typically provided poor training in both pain and addiction, and they’ve typically provided a narrow window in which we tend to consider people one problem at a time,” he said. “But the folks who are most vulnerable and caught in the crossfire of our opioid policy typically have a combination of medical illness, psychological illness and potentially current or past addiction.”
It’s vital to train more psychologists, nurses, and health professionals who can take care of people who have been on opioids for a long time — and also suffer from other health conditions, he said He pointed to an initiative from the U.S. Department of Veterans Affairs in Utah as an example of what to do. It focuses on veterans with addiction disorders, pain disorders, are homeless, or otherwise need a lot of primary care.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.