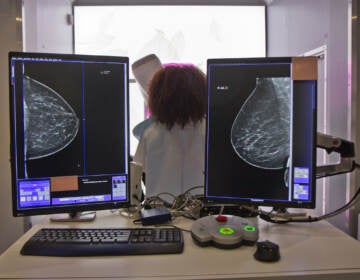
Black and white women have the same genetic risk of breast cancer, Penn study finds. So why are Black women more likely to develop the disease?
The findings of a new study from the University of Pennsylvania challenge past, smaller studies that found Black women face a greater genetic risk than white women.

Participants in the Avon Breast Cancer Walk pass the Capitol in Washington. (AP Photo/J. Scott Applewhite)
A new study from the University of Pennsylvania finds Black and white women have the same gene mutations linked to breast cancer risk. The findings challenge past, smaller studies that found Black women face a greater genetic risk.
For years, doctors have observed a higher and earlier prevalence of breast cancer in Black women before the age of 50. Experts say it has also been shown that Black women are more likely to have a more aggressive kind of cancer known as triple-negative breast cancer, which has a poorer survival rate.
Dr. Susan Domchek, executive director of the Basser Center for BRCA at the University of Pennsylvania and an author of the new study, said for years, clinicians and researchers didn’t know if these racial disparities were due to genetic differences in Black and white patients.

“And some small studies had suggested that this might be true,” said Domchek, “in addition [to] a study done by one of the commercial testing laboratories.”
However, Domcheck says these studies had biases, including that they were small. And in the case of the commercial testing laboratory, there was what Domchek describes as ascertainment bias, meaning that if it took more risk for Black women to get testing, it may look like they had more genetic susceptibility.
In the 1990s, researchers discovered that if you had a mutation in commonly shared genes called Breast Cancer1 (BRCA1) and Breast Cancer 2 (BRCA2), you had a much higher likelihood of developing breast cancer. And there was a strong association found between BRCA1 and developing triple-negative breast cancer in particular.
In 2020, Domchek and her colleagues at Penn wanted to see if there was truly a difference in the likelihood of Black women developing these breast cancer mutations compared to white women. They analyzed data from seven population-based studies in the CARRIERS consortium, a group of 17 large epidemiology studies in the U.S. focused on women in the general population who develop breast cancer. And the researchers measured the prevalence of pathogenic variants (PVs) in 12 genes known to confer breast cancer risk.
Dr. Katherine L. Nathanson is deputy director of the Abramson Cancer Center at Penn and another author of this study. Nathanson says while previous studies aimed at establishing the supposed higher genetic risk of Black women for breast cancer studied people with family history of cancer and other kinds of high-risk individuals, the CARRIERS study was a prospective study, meant to address the bias of those past studies.

“What that means is that women [across racial and ethnic groups] were enrolled at young ages and followed over time to see whether or not they developed breast cancer and other diseases as well,” said Nathanson. “And then you look at what the relative rates of mutations are in the people with breast cancer and without breast cancer.”
Nathanson says this overall study included about 32,000 women with breast cancer and 32,000 women without breast cancer from 12 studies that were not limited to patients with a family history of breast cancer or early onset disease. And what they found is that among the Black and white women studied, there was no statistically significant difference in PVs by race: 5.65% of Black women versus 5.06% of non-Hispanic white women had PVs in the 12 genes.
The researchers also found that younger age and ER-negative breast cancer were risk factors in the most impactful genes, including BRCA1, BRCA2, and PALB2, for both white and Black women.
In addition to challenging previous studies suggesting Black women have a greater genetic risk of developing breast cancer, these findings buck the notion that race should be an independent factor when considering genetic testing.
“And what that really led us to say is that we shouldn’t be factoring race and ethnicity into our decision about who to do genetic testing on,” said Domchek. “But what’s really important to note is that there are huge disparities in medical care between Black women and non-Hispanic white women.”
According to Domchek, Black women and white women with the same level of risk of having a specific genetic mutation don’t get tested at the same rates. And one of the major reasons is that Black women are not recommended by their doctors to do this at the same rate white women are. Domchek and Nathanson stress the importance of closing the genetic testing gap, and ensuring that Black patients have equal access to genetic testing that all patients do.
Domcheck says there are also patient concerns that contribute to this gap in testing, including misconceptions about future costs of breast cancer treatment.
“If an individual has, for instance, a triple negative breast cancer, the vast majority of the time it is covered by insurance with no or very low copays,” said Domchek. “But I think that there are women who are in a lower socioeconomic status who are worried about cost.”
And then there are fears about how patient data will be used by various health systems. Domchek says information collected from genetic tests are extremely useful for treating early stage breast cancer and can impact what drugs a doctor prescribes you for your cancer and surgical decision-making.
To help close that gap, the Basser Center launched its Black & BRCA initiative in 2020 to bring tailored resources and support to the Black community for genetic counseling and testing. The outreach effort provides tools to collect family history, address misconceptions, and educate providers.
Nathanson says even after this study, it is still not clear why Black women get earlier-onset breast cancer than other racial groups. There might be unidentified biologic factors that contribute to this disparity, including reproductive and environmental stressors, but more research needs to be done to better understand their roles.
“There are certainly places in Africa where women have very high rates of early-onset breast cancer,” said Nathanson. “So are there additional and other genetic risk factors that we have not as of yet identified in the African population that may be associated with [this] risk?”
Nathanson and Domchek are now involved in efforts to use electronic health records to identify people at risk for breast cancer and facilitate referral for them.
“One of the things about the electronic health record is it’s sort of agnostic to things like race and ethnicity,” said Nathanson. “And so you can identify patients with certain clinical characteristics, such as a diagnosis and an age of onset and facilitate referral for all those patients.”
Nathanson says the end goal is to ensure clinicians and the hospital system are identifying patients at risk in an efficient way, referring them for care as soon as possible, and providing support to physicians.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.