Using race to diagnose anemia in pregnancy led to poor birth outcomes for Black patients, study shows
For years, national medical guidelines have defined anemia differently for Black patients. A new study shows this could be increasing birth disparities.
Listen 1:11
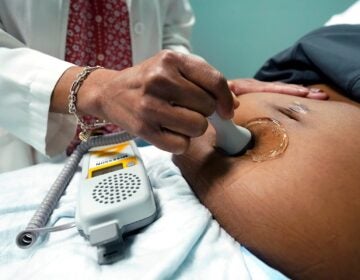
A medical professional holds a stethoscope on a pregnant person's belly. (VadimGuzhva/Bigstock)
For years, national medical guidelines have defined anemia differently for patients who are Black. Notably, over the years researchers and clinicians have observed significantly lower levels of iron in Black women.
Anemia, or low red blood cell count, is even more common during pregnancy because the body has to supply enough iron for itself and the developing baby. To account for the lower blood count levels among Black patients, doctors have used lower cutoffs to define when a Black patient can be considered anemic (compared to patients of other races) and subsequently receive treatment for the condition.
For at least the past decade, the guideline from the American College of Obstetricians and Gynecologists, or ACOG, said that pregnant people were considered anemic if their hemoglobin level was less than 11 in the third trimester. “But for Black women, that cutoff could be 10.2,” said Rebecca Feldman Hamm, an assistant professor of obstetrics and gynecology at the University of Pennsylvania.
Hamm said some doctors and health systems are now worried that race-based guidelines like this one may be exacerbating preexisting health disparities. In 2019, Black women were already 50% more likely to give birth prematurely than white women, according to the Centers for Disease Control and Prevention. And Hamm noted that Black patients are more likely to be anemic at the time of delivery than white patients are.

Prior to 2018, Penn Medicine did not have a standardized guideline for treatment of antepartum anemia. “[In 2018,] we created a guideline at Penn based on the ACOG recommendations around anemia and pregnancy to try and increase utilization and treatment for women,” said Hamm. “And we used different race-based cutoffs.”
But shortly after implementing the race-based guideline for anemia, Hamm said she and her team quickly saw potential negative effects. So she and some colleagues wanted to analyze whether the new guideline was affecting Black patients and their birth outcomes.
After looking at the records of 1,300 patients, self-identified Black patients who had no diagnosed anemia (with the race-based cutoff) during pregnancy were 65% more likely to have anemia at time of delivery compared to non-Black patients. The researchers also saw that both Black and non-Black patients who had less than 11 grams per deciliter (g/dL) hemoglobin at delivery had higher odds of requiring a blood transfusion. The findings are published in the journal Obstetrics & Gynecology.
Hamm said that when she and her colleagues analyzed the data of patients who had a starting hemoglobin level between 10.2 and 11, these were patients for whom the national guideline considers anemic if you are not Black, but does not recommend treatment for anemia if you are Black. And when Hamm analyzed the birth outcomes of the Black patients who fell within this range, she said they had a significantly increased risk of coming into delivery with anemia, despite not being considered anemic earlier in their pregnancy because of the race-based guidelines. The study showed this increased risk was associated with the fact that the health system was treating their anemia differently based on race.
“But when we looked at the group [of women with a hemoglobin level below 10.2], which is the group that women of all races were being treated and being called anemic [by the guideline], that disparity did not exist,” said Hamm. “The hemoglobin going into delivery ended up being very similar between races.”
Hamm said the study’s findings show that using different definitions of anemia by race is likely perpetuating long-standing health disparities, creating an uptick in Black women showing up to delivery with anemia, and increasing the risk of morbidity associated with that outcome. In addition, anemia creates significant complications, including increased risk of babies growing small, stillbirth, fatigue, and even postpartum depression.

Sindhu Srinivas, a senior author of the study and the director of obstetrical services at the Hospital of the University of Pennsylvania, said that after the results of the study were available, Penn Medicine officially changed its guideline in summer 2020. Penn is now considering all patients to be anemic if their hemoglobin levels are below 11 g/dL during any period of pregnancy. And the American College of Obstetricians and Gynecologists followed suit with an updated guideline that no longer uses race.
According to Srinivas, the impetus for the race-based anemia guideline came from the concern that clinicians had about potentially overdiagnosing Black women with anemia by using a higher cutoff. Clinicians still don’t understand why Black women are more likely to be anemic.
“Are Black women [a lot more] anemic than other races? Is that truly abnormal or do Black women naturally have a lower hemoglobin?” asked Srinivas. “But I think we’re beginning to understand that changing the definition to account for observed differences and thereby impacting treatment because of that difference is not the right approach and may even perpetuate some of those differences.”
Trending away from race-based guidelines in medicine
The change in treatment guidelines for anemia at Penn Medicine comes in the midst of massive change in recent years around race-based guidelines throughout medicine. In 2017, some students and advocates at Harvard University convinced Beth Israel Deaconess Medical Center in Boston to drop its use of race in how kidney function is measured.That landmark decision spurred many health systems across the country to do the same.
And in 2020, David Jones and fellow researchers published an article in the New England Journal of Medicine that analyzed 13 clinical algorithms that use a patient’s race in various medical practices, from kidney medicine to pulmonology, obstetrics, urology, and cardiology. What they found was that many of the tools meant to account for racial health disparities actually had a negative effect on Black patients’ health outcomes.
“A bunch of the tools operate in such a way that they direct resources towards white people,” said Jones, a medical historian and a professor of the culture of medicine at Harvard University.
Jones said there’s a general practice in medicine in which researchers observe a clinical difference in a specific racial group. But before establishing why that difference exists, like the higher prevalence of anemia among Black women, they simply acknowledge the difference and create treatment guidelines or diagnostic tools — one to use with white people and one to use with Black people. For example, in urology they use what’s referred to as a STONE score to predict the likelihood of kidney stones in patients who present to the emergency department with flank pain. The score assigns patients who are white a higher score, suggesting more risk.
“But what that means is if you show up in the emergency room with exactly the same symptoms, a white person is going to be given a higher score and given more attention from the ER staff potentially than the Black person would,” said Jones. “So when you unleash a tool onto the world, which [when] used as directed concentrates health care resources preferentially on white people versus Black people, it’s hard not to look at that with concern.”
And that’s been the growing consensus among many doctors and health systems across the country. Hamm, of Penn Medicine, said the next step of this research is to follow if and how dropping race from the anemia treatment guidelines positively affects the birth outcomes of Black patients in her health system.
“The hope is that by standardizing those definitions and, hopefully, now treating anemia far more greatly in the Black population, we will be able to improve outcomes for Black women at labor and delivery,” she said.
—
Support for WHYY’s coverage on health equity issues comes from the Commonwealth Fund.

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.