How a clinical tool meant to predict kidney function could be hurting Black patients
Is an equation most commonly used to predict kidney health unintentionally contributing to health disparities — and reinforcing racist thinking?
Listen 21:17
Nichole Jefferson (far left) is a kidney patient advocate based in Dallas, Texas. (Photo courtesy of Nichole Jefferson)
This story is from The Pulse, a weekly health and science podcast.
Subscribe on Apple Podcasts, Spotify or wherever you get your podcasts.
Updated Sept. 23
For years, Nichole Jefferson battled a series of health problems as she juggled a stressful job in the tech industry while raising her daughter. Then, in 2003, she wasn’t feeling well and went to a hospital with what she thought was a really bad case of the flu.
“So when I went to the emergency room … I was told, `You have to start dialysis immediately because your kidneys have shut down,’” Jefferson recalled. “I was like, `Wait, what? What are we talking about? Are you serious?’”
Jefferson did dialysis for a number of years before she was able to get a kidney transplant in 2008. And she did well for years after that. But transplanted kidneys typically last for about 10 years. So, close to a decade later, she started feeling ill again, in a way that felt familiar, like her transplanted kidney was shutting down.
“So I begged my doctor to do a biopsy, and he kept saying no because it wasn’t warranted,” said Jefferson. “And I said, `Well, I’ll pay cash out of pocket. I just have a feeling.’”
She and her doctor went back and forth for about six months until he finally gave in. And when the biopsy results came back, they showed that 90% of her transplanted kidney was scarred and not functioning correctly. So once again, Jefferson had to get on waitlists for a kidney transplant at hospitals in her region. She recalled trying to get on a list at a top hospital in Minnesota.
“And they said, ‘We can’t put you on the list because your kidney function is not down far enough,’” Jefferson said.
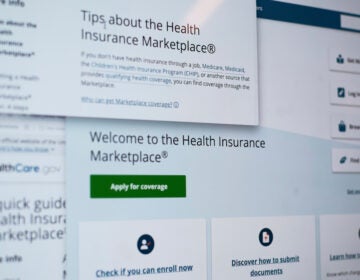
In the United States, a single number determines whether you’re eligible for a kidney transplant. For the last two decades, a clinical laboratory test called eGFR — which stands for estimated glomerular filtration rate — has been used to evaluate how efficiently a person’s kidneys remove creatinine, a waste product they filter out of blood.
The eGFR equation reports a score based on measured creatinine levels while also considering a patient’s age and gender. But that day, Jefferson learned the equation was different for her because she’s Black.
A national task force announced Sept. 23 that it is recommending the immediate implementation of a new diagnostic equation for measuring kidney function that recommends that U.S. clinical laboratories immediately implement a newly refit CKD-EPI creatinine equation that does not incorporate a patient’s race.
Advocates say this will promote health equity and increase access to transplantation for Black patients, who, due to differences in how previous equations measured their kidney function, were not able to get diagnosed or onto transplant lists in time.
What is glomerular filtration rate?
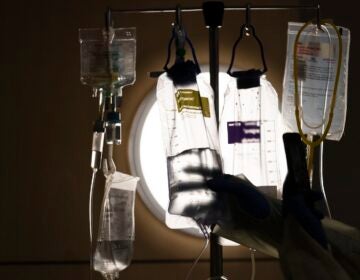
To understand Jefferson’s dilemma, you have to understand a little bit about what kidneys actually do. Healthy kidneys filter about a half-cup of blood every minute, removing waste and extra fluid out of the body via urine. When that filtration function isn’t working, over time there are some telltale signs: swollen feet, nausea, cramps, back pain. When doctors want to assess a patient’s kidney function, they have to check in on the glomeruli, a network of small blood vessels that are responsible for filtering that waste out. And the rate at which they filter the blood is called the glomerular filtration rate, or GFR.
“To actually measure GFR is very difficult because you have to collect a series of blood measurements as well as urine measurements,” said Amaka Eneanya, a nephrologist and assistant professor of medicine and epidemiology at the University of Pennsylvania.

Eneanya said that though GFR is considered the gold-standard measurement for kidney function, it is very time-consuming to collect. It could take an overnight hospital admission to measure. But thankfully, she said, one of the kidney’s other jobs is to reabsorb all the fluid we need to retain in our body and release the rest of the waste and extra fluid through our urine.
So for years, nephrologists have used estimated glomerular filtration rate, or eGFR, equations and looked at one specific waste product in the blood — serum creatinine — in addition to age, sex, and race, to estimate kidney function so doctors can make snapshot decisions about someone’s kidney without the hassle of directly measuring the filtration rate.
But in American medicine, there are only two race variables for these equations, Black and non-Black. And a growing number of kidney experts say that’s a problem.
How did “Black race” become part of the estimating equation?
In the 1990s, Andrew Levey was leading a research project called the modified diet in renal disease (MDRD) study. It looked at people with kidney disease to try to see whether low-protein diets and lower blood pressure goals could slow worsening of the disease. The study had about 1,600 participants and collected their gold-standard kidney function measurements — think constant blood and urine measurements — and their serum creatinine measurements.
“And we realized that we had thousands of observations where we could relate the observed serum creatinine to the measured GFR, and that could help doctors in practice because they’re used to just dealing with creatinine alone,” said Levey, who is currently the chief emeritus in the division of nephrology at Tufts Medical Center.
It was a huge moment for kidney medicine. For the first time ever, researchers were able to compare gold-standard GFR with serum creatinine in patients to see just how well creatinine could predict measured GFR. And in doing that, a clearer picture emerged.
“And the other things that we found that made the biggest difference in the level of creatinine for the same GFR were the age, the sex, and the race of the patient,” Levey said.

Creatinine is essentially a breakdown of muscle in the blood. And Levey and his researchers found that, while easy to measure, on its own it wasn’t a reliable index of true kidney function.
If you’re biologically female, on average you’re less muscular than your male counterparts. Older people tend to be more frail than young people. Eating a high-protein diet or bodybuilding — all these things could affect the amount of creatinine in your blood independent of your real kidney function.
So researchers quickly realized that if they wanted to create an equation that would best estimate the kidney’s filtration rate, creatinine alone wasn’t gonna cut it.
Age, sex, and weight were important, but so was race.
“And they found that Black participants in that study, compared to white participants at the same measured GFR or kidney function, had higher levels of serum creatinine,” said nephrologist Amaka Eneanya.
Higher creatinine levels — more waste product in the blood — typically meant worse kidney function. But this study also showed that creatinine was influenced by things such as how much meat someone ate and how muscular a person was.
For the equations to better predict the gold-standard measurement observed in Black study participants, the researchers introduced a multiplication factor for Black patients that increased their kidney function to make up for those higher levels of serum creatinine in their blood — which at the time researchers attributed to Black people being more muscular than white people, a theory later debunked.

But Eneanya said this Black multiplication factor can have serious life-or-death consequences because it can determine how soon a patient gets a new kidney.
“We’re assigning Black patients to have better kidney function, so there’s a delay in terms of when they can actually get referred to be evaluated for a kidney transplant,” Eneanya said.
Use of race in kidney care met with early criticism
There was pushback against this race adjustment right from the start. Experts, including Levey himself, said the study had a lot of issues. According to Levey, the study only included people with kidney disease, so not very many healthy people. It had a small proportion of Black people in the study cohort. And It didn’t have very many people who were elderly.
And Eneanya said the study didn’t really include people of other races.
“There weren’t a high number, for instance, of Asian participants or Latinx and Hispanic participants,” Eneanya said. “And so they kind of lumped all of those participants together with the white participants. So it really became a Black versus non-Black investigation for these studies.”
And critics of this study say one of its biggest issues was that the researchers never identified why there was this observable difference in serum creatinine between the Black and white people participating.
“That’s the million-dollar question to this day,” said Eneanya. “What they said was … that Black people had higher serum creatinine levels because they’re more muscular than other individuals, other racial groups, and they use very weak and flawed studies to support this assertion.”
Those notions go back to slavery, Eneanya said, when Black enslaved people were seen as biologically inferior to white people. So the criticism mounted. And in the early 2000s, Levey redid the study with funding from the National Institutes of Health. He and a team of researchers formed a group called CKD-EPI. This time, Asian and Hispanic people still made up a very small proportion of those studied, less than 5%, but Black people now made up 30% of the cohort. It was also a much larger study cohort, with close to 8,000 participating, and a range of healthy people as well as people with chronic diseases were included.
And in this new and improved study, Black participants, on average, still had higher levels of serum creatinine than non-Black patients.
When those results were published in 2009, the equation was adopted widely across U.S. health systems as one of the standard ways to estimate kidney function, and the number continues to be adjusted for race to this day.
This calculation, this number, is what stood in Nichole Jefferson’s path when she was trying to get listed for a kidney transplant at a hospital in Minnesota.
Subscribe to The Pulse
When Jefferson tried to present the biopsy of her kidney that showed its true health, the hospital refused to accept it.
“This is one of the places [that is] considered top-notch,” Jefferson said. “And you’re looking at a number and saying, because I’m Black, this is what you’re going [on] and I can’t be listed. So that was very frustrating.”
What is race correction?
Had she been a different race, Jefferson said, she would have been eligible to get on the transplant list at the hospital. In medical practice, that’s commonly known as race correction.
David Jones is a medical historian at Harvard University who studies it.
“One thing that has happened in medicine … largely in the American context, is because we have these old deep intuitions that Black people and white people are different in a way that’s medically relevant, there are many practices in medicine, whether it’s a diagnostic test or treatment guidelines, where they’ve created two versions of the tool, one to use in white people and one to use in Black people,” Jones said.

In summer 2020, Jones and fellow researchers published an article in the New England Journal of Medicine that analyzed 13 clinical algorithms that use a patient’s race in various medical practices, from kidney medicine to pulmonology, obstetrics, urology, and cardiology.
Jones said such use of race in medicine doesn’t always make sense. To begin with, so many different kinds of people are included in the category of “Black:” mixed-race people who mark “Black” on the census; newly arrived African immigrants with distinct genetic ancestry from Black Americans; Afro Latinos.
“When people move between Brazil and the U.S., whatever their identity is, their perceived race will shift,” Jones noted. “Many people in Brazil who identify as white would get coded as Black in the U.S. How can any medical tool that relies on the shifting subjective categories be a meaningful basis for precision medicine? I just don’t get it at all.”
Then there’s the issue of people who are Black and identify as more than one race. When a mixed-race patient approached nephrologist Amaka Eneanya about getting on a kidney transplant list, she asked Eneanya if she could list her race as white to get listed earlier.
“Even though she identified herself as a Black woman, she phenotypically looked like a Black woman, she asked if she could use her white side because that would be a lower eGFR, which would be seen as worse kidney function so she could get listed earlier and gain more wait time,” Eneanya said. “And they did it.”
Eneanya said the woman was well within her right to do so because currently there isn’t an accommodation for mixed-race patients like her.
Jones said race correction in the U.S. is riddled with arbitrary inconsistencies. For example, though nephrologists who treat adults use an eGFR calculator that considers race, pediatric neurologists don’t.
“As if somehow you don’t need to race-correct kidney function until age 18, but once you turn 18 in the U.S., you do start race-correcting,” Jones said.
Toward a racial reckoning in kidney care
In the wake of the Black Lives Matter movement in 2015 and the demonstrations against racism that followed in the years afterward, health systems were having their own racial reckoning too.
Black people are almost four times more likely to suffer from kidney failure than non-Hispanic white people. And once they get to that stage, Black patients spend months longer waiting for kidney transplants than white patients do.
In 2015, some medical students at Harvard who were learning about eGFR started to wonder if race correction tools were contributing to these disparities.
Leo Eisenstein, now a third-year resident in internal medicine at NYU, was a med student at Harvard at the time.
“Our social science faculty were telling us pretty clearly that race was a social construct and not a reliable proxy for genetic difference,” said Eisenstein. “And then as we got to our clinical learning, we were finding out that race was used exactly in that way as a proxy for genetic difference.”
At the same time, a growing body of research was showing that social factors such as housing, education, and income were more responsible for racial health differences than potential genetic differences among racial groups.
“On average, in the United States, Black families have less wealth than white families by a large amount, and that affects everything,” said Jones, the medical historian. “It affects where you live, it affects what schools you go to, it affects what food you eat, it affects what enrichment activities you have access to.”
Jones said that if you find two random 30-year-old men, one white, one Black, you may find observable biological differences.
“And what medicine too often has done has said those differences are because of race … because one is Black, one is white,” he said.
In 2015, Eisenstein co-founded a coalition of students who got together to study and evaluate the use of race in various medical practices, one of those being estimated kidney function equations. In 2017, they convinced Beth Israel Deaconess Medical Center in Boston to drop its use of race in eGFR.
That landmark decision spurred many health systems across the country to do the same. The University of Washington and Vanderbilt University are two of the many medical centers in the U.S. that have abandoned the use of race from their eGFR equations.
Andrew Levey, the researcher who revolutionized kidney medicine with those equations, said this moment pushed him to reflect. When he looks back at the initial 1999 study that introduced race into eGFR, he said, there are some things he wishes his team had done differently.
“As times change, people’s ideas of what was a good idea changes,” said Levey. “We really thought back then in the mid-’90s, when we were doing our study, that we were doing a lot of good by recognizing the differences in creatinine between Black [people] and white [people], because we’d have a better estimate.”
What has become clear, he said, is that they put too much emphasis on the race variable, which now they understand is really a social factor rather than a biological factor.
Will dropping race from eGFR do more harm than good?
Some kidney experts argue that you can’t blame the equations for all the inequities in kidney care. For example, one study found that even Black patients who qualified for transplants with a race-adjusted score were still not getting them. And kidney expert Neil Powe noted that racial disparities in chronic kidney disease existed long before the use of race correcting tools.
“What is not said is that all of those disparities were well documented in the 1980s and early 1990s before the race equations were ever published or used in medical practice,” said Powe, a professor of medicine at University of California, San Francisco. “So those disparities were already there, meaning that the equations could not have caused those disparities.”

Getting rid of the race factor in estimating kidney function could have some negative implications, including how doctors dose medications, Powe said.
“And so if you just drop the coefficient and you lower an African American’s kidney function, you make them ineligible for some very important drugs, drugs to treat diabetes, drugs to treat cancer, drugs to treat pain, for which we already know that African Americans have access and disparities to get those drugs.”
Powe said that could mean Black patients being prescribed medications they don’t need or being denied treatment they do need. It could even incentivize doctors to give Black patients a diagnosis of kidney disease when, in fact, they may not have it.
“That could have implications for them, for example, getting life insurance,” Powe said.
A more accurate marker than race is needed for assessing kidney function, Powe agreed, but as hospitals rush to eliminate race from their equations, he worries that without national guidance the use of race in eGFR will be applied inconsistently across different health systems, which could have disastrous effects for Black patients.
So in August 2020, the National Kidney Foundation and the American Society of Nephrology formed a task force to debate the pros and cons of using race in estimated GFR. In April 2021, they issued an interim report stating that they no longer recommended the use of race in the equations.
But now, the question becomes: How to take race out?
Toward a better kidney function equation
Andrew Levey, whose research led to development of the estimated score, said it turns out the best way to make the equations more accurate again is to measure a biomarker in the blood in addition to creatinine. It’s called cystatin C, and Levey said it doesn’t depend on the use of race.
“Cystatin C is a protein that’s made by all cells,” said Levey. “We don’t understand as much what governs how much it’s made, but we do find that the level of cystatin in the blood is related a little bit to age and a little bit to sex — less related than creatinine — but it doesn’t appear to be related to race at all.”
Experts say it’s slightly better than creatinine because it’s less affected by such factors as whether someone is vegan or how old someone is than creatinine would be.
And when we’re talking about a vital organ like a kidney, the stakes are high. Getting it right could be the difference between someone living and someone dying.
Nephrologist Amaka Eneanya said that while kidney experts vary in opinion about how to account for race in precision medicine, she believes the use of race is worth reconsidering.
“It’s a huge stepping stone, it’s kind of a historical moment that we are challenging the literature in this way,” Eneanya said.
“I think that we should keep our attention on racial inequities, but we actually need to take steps towards that. We’ve described racial inequities for a very, very long time, and we’re beyond the point of describing. It’s time for action.”
Waiting for the call
Nichole Jefferson did eventually get a new kidney transplant after listing herself at hospitals all over the country in 2020.
At 2 a.m. one April morning, she got the call she had been waiting for — there was a match!
That same morning, she boarded a plan from Dallas, where she was living, to Iowa to get her transplant.

She’s now an advocate for other Black patients battling kidney disease.
Jefferson says she’s overwhelmed by stories like hers — stories of Black patients just trying to get the care they need and having to face barrier after barrier to get it. She fears that race correction in eGFR could be making it much harder for Black people to survive.
Support for WHYY’s coverage on health equity issues comes from the Commonwealth Fund.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.