The expanding role of the physician assistant
Listen-

-

-

-

-

-
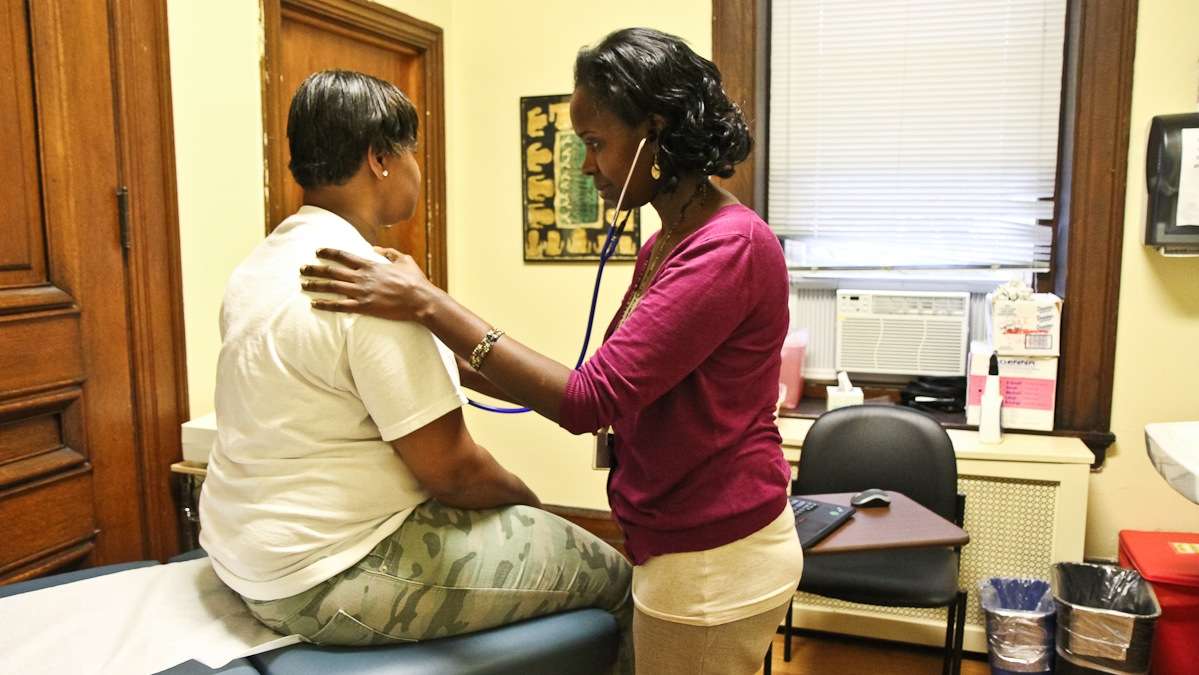
Lucy Kibe examines patient Sherri Robinson at St. Elizabeth Wellness Center
If you’ve ever gotten health care, for anything really, you’ve more than likely been helped at some point in a critical way by someone in this position.
No, it’s not the physician…but rather, the physician assistant.
“It’s not physician apostrophe ‘s’ [as in, physician’s assistant]. We’re not the possession of the physician,” explains Patrick Auth, director of the physician assistant program at Drexel University, of one of his biggest pet peeves. “It’s the physician assistant.”
Or ‘PA’ for short.
Whatever one might call it, the profession is booming right now, as the health system looks to it and other non-physician practitioners to help increase capacity and handle an anticipated influx in patients.
As a result, new training programs are popping up around Philadelphia and elsewhere. The number of PAs has more than doubled in the last decade, with about one PA out there for every 9 or 10 doctors.
Some patient surveys have found that people trust the doctor most, but the role of the PA itself has been changing, and even expanding.
So what exactly is a physician assistant?
At first glance, one might think Jesse Coale is a doctor at State Road Medical Associates, a general medicine practice in Drexel Hill, Pennsylvania. He sees his own patients, diagnoses and treats them.
Except he would never identify or introduce himself that way.
“I can’t practice on my own,” he says. “I have a supervising physician.”
Coale, who also directs Philadelphia University’s physician assistant training program, works under a negotiated agreement with the physicians at State Road. That agreement defines what he can and can’t do. In Pennsylvania, the terms must also be approved by the state board of medicine.
Both he and the doctors are liable for his care.
“Somebody like Jesse, who’s been here a long time, I trust what he does,” explains Dr. Namir Kosa, Coale’s supervising physician. “If this was somebody who’s starting now out of school, then I’d have to be with them, at least in the beginning for a while until I’d be sure that they are doing the right thing and in the way I want them to be doing it,” he says.
Kosa doesn’t even have to be in the office when Coale sees patients, but he does have to be available by phone or electronically, in case anything comes up. He also reviews and signs off on all of Coale’s charts. Pennsylvania recently changed its rules to allow the option of less direct oversight.
A little bit of history and a common thread
Coale recalls being hired on at the State Road practice about 25 years ago by a doctor who has since left.
“He needed help,” he says. “He couldn’t afford a full time partner, so he hired a physician assistant which happened to be me.”
John McGinnity, president of the American Academy of Physician Assistants, says the whole PA profession started as a response to primary care and rural access shortages in the late 60s.
“So at that time, they decided, ‘let’s create a new profession, put them through an accelerated medical school type process like they did for doctors in World War II,” says McGinnity. “So we’re going to train them in the medical model, put them through an intense and accelerated program, and have them come out and improve access.
PA training lasts two to three years, whereas training a doctor can take up to a decade. Nurse practitioners tend to have a Master’s or Doctoral degree after having practiced an average of 10 years.
In the last decade alone, the PA profession has more than doubled in size. There are approximately 100,000 certified PAs practicing across the U.S. Most states have either passed or updated laws pertaining to PAs, according to McGinnity. About a third of PAs are in primary care, a percentage which has actually declined since the profession’s early days. McGinnity says the rest have expanded across just about every specialty you can think of.
“If you have a patient going for bypass surgery, the majority of vein grafts harvesting, that’s an area of expertise of PAs,” he says.
Dr. Mark Friedberg, a researcher specializing in workforce issues with the Rand Corporation, says PAs tend to fall into one of two roles: a substitute role, as is the case with Jesse, or a complimentary role, such as assisting in surgery. Physicians may also handle the more complex cases.
Policymakers are increasingly relying on PAs and nurse practitioners to address growing concerns about doctor shortages in the years to come. Their responsibilities are growing. A recent Institute of Medicine report also pointed to mid-level practitioners, working with doctors in a new team-based model of care, as key elements of increasing the health system’s capacity.
“Even without increasing the supply of physicians beyond what there currently is, even if the population grows and ages, there isn’t necessarily going to be a physician shortage because each physician can probably take care of more patients working with a team of nurse practitioners and physician assistants than a physician can working on his or her own,” says Friedberg.
People may compare PAs to nurse practitioners, or NPs, which started around the same time. PAs and NPs may both serve as primary care providers, but the type and approach in training varies. In some states, NPs can practice totally independent of a physician.
More training programs but more competition
The PA field’s popularity, along with increasing health care needs, have fueled a major growth in PA training programs.
Thomas Jefferson University Hospital launched a program this spring.
Susan Dubendorfer, director of curriculum and evaluation at the new school, says students are in some highly coveted spots.
“We had almost 2,000 applications for 30 slots in our class that we’ve seated this year,” she says. Another 1,500 applied for next year’s class.
Some in the health industry become PAs as a second career, but 24-year-old Janel Jesberger and Jefferson PA student, says she was drawn to the profession after shadowing a PA, and seeing the kind of relationships in that practice that one could develop with patients. She’s interested in orthopedics but lightheartedly recalls first having to explain to her family what she was even getting a degree in.
“I come from a family of engineers, and they looked at me and were like, ‘What? What is this? Just a nurse?’ So I had to explain that all over again,” she says.
PA school was a first choice for 27-year-old Samantha Melonas, adding that it may pay for itself in the first year or two after obtaining a license.
“The average salary coming straight out of school is around $80,000 or so, and then depending on the field you’re in, it’ll grow from there.”
The salary is about half of an average physician salary.
Nationwide, there are nearly 200 certified training programs, compared to about 50 in the early 90s. There are currently 23 programs across New Jersey and Pennsylvania, including five new ones in the last two years, according to the National Commission on Certification of Physicians Assistants.
Philadelphia University plans to expand to Atlantic City soon. Temple is on track to open a program in two years. Three other schools – Mercyhurst, Slipperty Rock and Kean University – appear to have something in the works.
‘On trial’
Inside State Road Medical Associates on a recent evening, Coale meets with an older patient, Barbara Kammer, who has a nasty chest cold. She’s feeling weak and uses a walker to get around.
“Now, your sister was here a bit ago, did she give [the cold] to you?” Coale asks.
The two laugh.
It’s about 6 p.m. and Dr. Kosa has already left for the day. Coale is also the provider on call for the night.
He writes up a prescription for Kammer. When he first started practicing, he recalls, PAs weren’t allowed to prescribe anything.
Kammer recalls having first started seeing Coale about 15 years ago, when her doctor got too busy.
“He pushed me off on Jesse,” she says smiling. “He was on trial!
But Kammer says he did the right things.
“And I said, ‘This is it.’ He’s not a doctor but I’d rather go to him than anybody else.”
This is the first in an occasional series on The Pulse about the region’s health care workforce.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



