Do 3D mammograms detect more invasive cancers?
Listen-

-

-

-

Patricia Ortiz was team captain for LAM Foundation Easy-Brethers. Ortiz was an elite cyclist when she was diagnosed with LAM disease 2 years ago
-

-

-

-

-

-

-

-
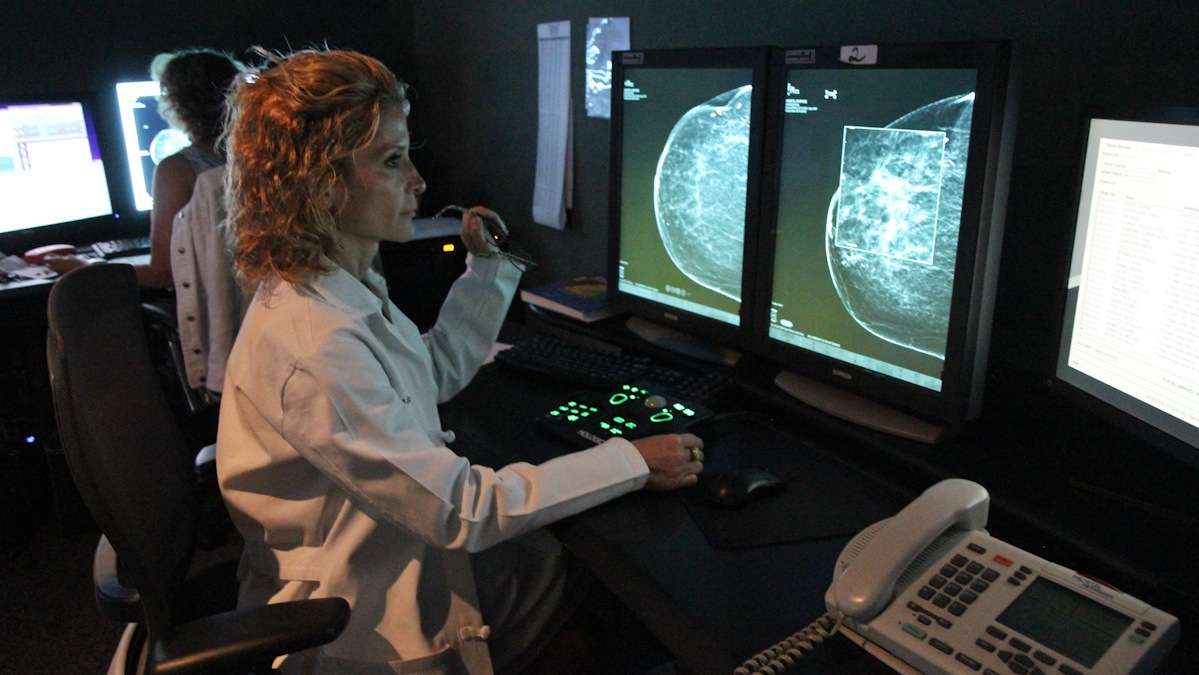
Dr. Debra Somers Copit reads mammography results in the Reading room at the Marion-Louise Saltzman Women's Center at Einstein Hospital's campus. (Kimberly Paynter/WHYY)
New research published in the Journal of the American Medical Association compares standard 2D mammography to 3D mammography.
Two health systems in Philadelphia now offer a three-dimensional digital test to everyone who comes in for a routine mammogram.
It’s a new approach to breast-cancer screening, and a change that most hospitals have not made. Radiologists at Penn Medicine and Einstein Medical Center say they were early adopters and are now big believers in the new technology.
A study published this week in the Journal of the American Medical Association compares standard two-dimensional digital mammography with a combo technique that adds on tomosynthesis, or 3D mammography.
The researchers say 3D screening detected more cancers that are likely to spread. It also reduced the number of women called back for unnecessary screening because of a false alarm.
A ‘deeper look’
Radiologist Emily Conant, chief of breast imaging at the University of Pennsylvania Medical Center in Philadelphia, co-authored the study and is an unpaid consultant to manufacturer Hologic, which makes the 3D technology.
She said 3D scans give her a “deeper look” when she’s studying a mammogram, kind of like opening a book to see the pages inside.
“In 2D mammograms things can be hiding behind structures. In the 3D mammogram we can leaf through the breast tissue and see different normal things as well as things that are potentially abnormal,” Conant said.
“It’s literally like if you had pick-up sticks and you threw them out together and they would be all on top of each other. And say there was some object hidden in the pickup sticks, you’d have trouble seeing it,” said study co-author Debra Somers Copit.
Copit, who is director of breast imaging at the Einstein Healthcare Network, said a three-dimensional image lets doctors see beyond the body structures that can block the view.
Copit is a scientific advisor to tech-maker Hologic which funded the study along with the National Cancer Institute.
3D breast scans expose patients to a slightly higher does of radiation. The extra cost is generally not covered by health insurance.
Fewer false alarms
The research was a ‘look-back’ study of mammograms conducted at 13 screening sites around the country, and examined the records of nearly half a million patients.
It’s the best evidence yet that 3D scans find more cancer—especially invasive tumors that doctors worry will spread, Copit said.
“It is also better because we have fewer false positives, so we are calling fewer patients back. Many, many times a day I’m grateful to the tomosynthesis images to help me determine that something that I questioned on the 2D image is absolutely nothing,” she said.
In the new study, the 3D technique resulted in 15 percent fewer false alarms that can cause unnecessary anxiety for patients.
That addresses a big critique of all mammography: that it leads to overdiagnosis and unnecessary treatment. Overdiagnosis is a term that means finding a cancer that may never grow large–or unwieldy–enough to cause true problems.
In the x-ray reading room at Einstein, Copit pulls up a breast image with two fuzzy white spots, then clicks to zoom-in on the 3D image. To her trained eye, suddenly it’s clear: One spot is a bunch of normal blood vessels and ligaments. The other spot is cancer.
That detail didn’t show up on the 2D image, but the second mass has branching tentacles. “That’s classic for invasive cancer,” Copit said. “Cancer in Latin means crab, so it’s these sort of crab-like projections.”
Similar process, different outcome
West Philadelphia mom Lisa Clapper had her 3D mammogram at the Perelman Center at Penn Medicine.
The 43-year-old had lymph node cancer as a teenager, and the treatment she had decades ago makes her high risk for another tumor. Ever since, doctors have been closely monitoring her health. In April 2013, she was overdue for her mammogram.
“I remember going in, and I just thought it will be the same as it always is,” Clapper said. “You go in, you get the press down. Smack. Your breast turns into a pancake.”
The arm of the mammography machine swings a few degrees to the left and right to capture the 3D images.
Clapper said from her perspective, the experience was exactly the same. Except, this time she got a call a few days later. Doctors said something looked “iffy,” on her 3D scan and they recommended a follow-up ultrasound. Soon after Clapper was diagnosed with cancer in her left breast.
“It’s emotional, it’s incredibly scary,” she said. “And much more scary as a parent and as a wife, with a family with children, than when I was 19.”
Radiologists at Penn said 3D mammography helped make Clapper’s diagnosis when the tumor was small and treatable.
Addressing a ‘potential harm’
In the JAMA study, tomosynthesis found more cancers, but some policy watchers say the ultimate goal of screening is not to just find more cancer.
The goal is to save more lives and reduce deaths in a way that doesn’t have a lot of harms, said Steven Woloshin, a physician and professor at the Dartmouth Institute for Health Policy and Clinical Practice.
“The most fundamental open question is: Does this reduce breast cancer death,” Woloshin said. His research specialty is helping people understand what medicine can and can’t do.
“We just don’t know. And the fact that [the study] is getting all of this media coverage, I think the potential harm is that women, and clinicians may be tempted to change practice on the basis of this data, and I just think that that would be premature,” Woloshin said.
This week, Fran Visco, president of the National Breast Cancer Coalition, said while the technology may sound exciting to some, it’s important to remind women but of the extra cost and extra radiation associated with 3D imaging.
“Women should not be rushing to their doctor and asking for 3D mammography,” Visco said. “They should be waiting to see the results of more studies to see if it will actually benefit their lives. We don’t know that, this [study] is a step along the way to finding that out.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



