Should there be standards for acupuncture in the U.S.?
If you get acupuncture in the U.S., chances are you will pay for it out of pocket. Some acupuncturists say having standards for the industry gives more people access.
Listen 11:40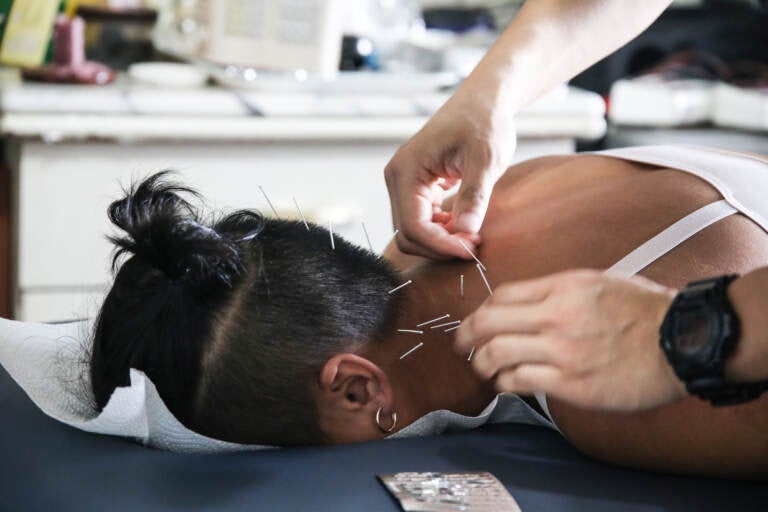
Acupuncturist Toto Cheng performs acupuncture on an athlete. (Lin Tin Nok/WHYY)
This story is from The Pulse, a weekly health and science podcast.
Find it on Apple Podcasts, Spotify, or wherever you get your podcasts.
When Tyler Phan was 17, he went to visit his relatives in Vietnam during the summer. He has asthma. It was hotter and more humid in Vietnam than in western Pennsylvania where he lived — which made his asthma worse.
His grand uncle gave him a quick lesson in acupuncture. Then he handed Phan the needles. Phan put needles in his forearm, which hurt but also made him feel better. It was “almost … an instantaneous relief in my breathing,” Phan said.
His mother told him this medicine is a family tradition, passed down through generations. She introduced him to acupuncturists who work at hospitals in Vietnam that were connected to Buddhist monasteries that serve the poor. Phan became an apprentice and started doing acupuncture.
Phan really liked the DIY aspect of acupuncture, and thinks it appealed to him because he was also into punk rock.
“The unique thing about acupuncture is that you can needle yourself,” Phan said. “It gives you this great sense of autonomy and it gives you a sense of self-empowerment.”
After spending a few summers in Vietnam, he decided to pursue acupuncture as a career. But he knew that if he wanted to practice in the U.S. he had to get credentials at an acupuncture school. He attended a four-year program at a school in North Carolina.
On the very first day of class, Phan’s instructor told him, “if you are needling someone without a license, that you are doing something illegal.”
“And I don’t know if it was me being young, 19 at the time, or being punk rock. I immediately questioned why.”

The acupuncture school also taught a much different philosophy than what he had grown up with. He learned that if somebody has pain in one area — the needles should go into another body part that is similar. For example, if someone had left knee pain, the acupuncturist would put the needles in a part of the body that looks like a knee but is not a knee, like the right elbow.
But at school, he learned a mixture of Chinese and Japanese traditions, translated from the point of view of British and French practitioners. Then, he prepared for the national board exams, which tested students on standardized practices from 1950s China.
“A lot of the students were completely in dismay because they had to relearn a completely other set of Chinese medicine.”
Phan was confused by all of these different requirements. He wondered: Who gets to decide on these standards in the U.S.? What should be taught in acupuncture schools? And why is it so different from what he learned?
“It seemed a little bit arbitrary and baffling to standardize these disparate practices,” he said.
Phan got a master’s degree, and a PhD to answer those questions. For his PhD research, he traveled across the U.S. to find out how different acupuncture schools treated patients in their clinics and what type of acupuncture they were using.
None of the schools wanted to work with him, so he went undercover as a patient. He went to clinics in Oregon, California, New Mexico, Florida, North Carolina, and Pennsylvania. He had shingles at the time, and pain in his left shoulder. He wanted to see what practitioners at different clinics would do with the same set of symptoms.
He was treated sometimes with regular acupuncture, sometimes with electroacupuncture, sometimes with tuning forks. Some clinics talked to him about his health history for 15 minutes; while another interviewed him for 2 ½ hours.
He says he felt better, to varying degrees, after all of the treatments he received, so he did not come away thinking any one approach was better than the other.
Subscribe to The Pulse
After all this, he wondered: Why try to create one national standard, like with the national board exam, if acupuncture already comes from vastly different traditions, and practitioners end up doing vastly different things to patients anyway?
“If I didn’t know anything about Chinese medicine or acupuncture, it would be this black box of … jargon that they’re using, right? But I’ve been studying and practicing for 15 years, so I had an understanding,” Phan said. “It was, for me, really fascinating how they came to those points or how they came to those specific formulas,” he said. “None of it was consistent.”
Phan said that variation is a feature, not a bug. He explained that to him, acupuncture is a little like the slime that his 8-year-old son used to play with.
“It attaches to … dirt, attaches to Legos and attaches to anything that it touches,” he said. “Chinese medicine has a similar context in regards to culture: It attaches to a lot of the cultural mores, the regulations, the other medical practices that are involved.”
He said trying to create one standardized acupuncture exam in the U.S. is like trying to make slime solid: it’s pointless, and it defeats the purpose.
Instead, he said schools should focus on teaching patient safety, and the logistics of running a private practice; don’t focus as much on one particular type of acupuncture that a board decides should be the standard.

It’s not a popular take with some acupuncturists who say the field needs standards because without any, no one would take them seriously. Licensed acupuncturist Elaine Wolf Komarow has been practicing in Virginia since the 1990s, and she worked with lawmakers in her state to help create the regulations.
“The establishment had no confidence that we knew what we were doing,” she said.
Anyone could say they’re a master at acupuncture even if they don’t know what they’re doing. It’s rare, but there can be bad outcomes from acupuncture, like bleeding, bruising or nerve injuries.
“We found it helpful that there was an exam that we could point to as an independent exam that was not offered by the schools, that could give some stamp of approval, ” Komarow said.
Having these kinds of standards could also mean that acupuncture will be covered by insurance, said Mina Larson, the CEO of the national acupuncture board, the National Certification Commission for Acupuncture and Oriental Medicine.
Larson said having standards and regulations is the key to expanding access to this treatment.
She also said the board reviews its standards every five years. And they do a broad survey of the field, to make sure their regulations can apply to different acupuncture traditions and reflect the diversity of the field. The purpose of the national exam is to make sure people joining the field know the basics of physiology and anatomy.
Emilie Cloatre, a law professor at the University of Kent in the U.K., studies how governments regulate alternative medicine. She said there are always going to be tradeoffs when applying rules created for Western medicine to other practices. Being hands off might mean patients could be taking a risk with treatments that cost a lot — but are not effective or reliable. But creating regulations means an organization has to decide what it considers acupuncture, and who gets to practice.
Countries can come to completely different conclusions. For example, in the U.K., private acupuncturists do not need to register with any national body to start practicing. But just across the English Channel in France, only medical providers like doctors and nurses can officially give people acupuncture.
Cloatre added this balancing act applies not just to acupuncture, but other medical traditions in the West that are outside of Western biomedicine: Ayurveda, naturopathic medicine, and other kinds of alternative medicine.
“There is always a danger when you regulate those particular practices that by regulating them along the lines we are used to in the West, we end up validating only particular forms and reimagining what different traditions should be about.”
It’s a delicate balance between setting standards, safeguarding patient wellbeing, and protecting the traditions that made these practices appealing in the first place.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.







