COVID-19 ‘long haulers’ face uncertain future
Many people who had COVID-19 are still experiencing symptoms weeks and months after they were infected. Now, a Penn clinic is trying to help these "long haulers" recover.
Listen 15:34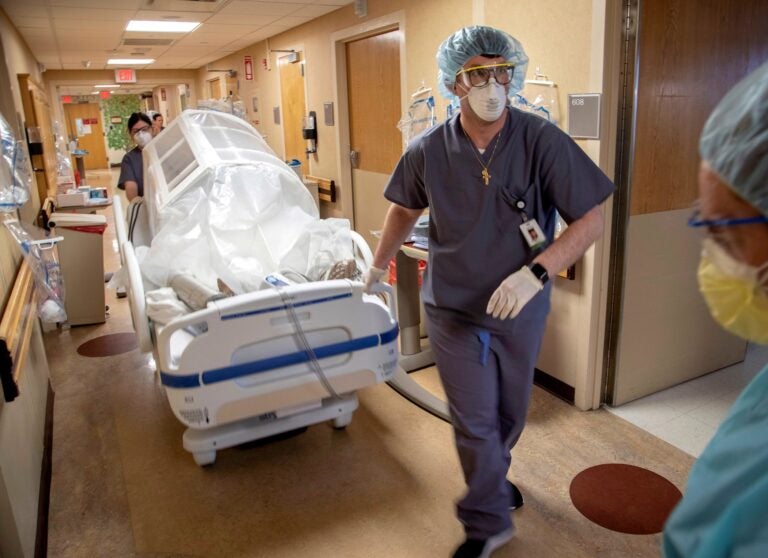
A COVID-19 patient is transported at Holy Name Medical Center in Teaneck, New Jersey, on March 19, 2020. (Jeff Rhode /Holy Name Medical Center)
When the pandemic started, most doctors seemed to think that COVID was an illness that typically lasted about two weeks. Now, we know a lot of people are still experiencing sometimes debilitating symptoms weeks and months after they were infected. A University of Pennsylvania clinic is trying to figure out why they are still suffering and how to treat them.
WHYY health reporter Nina Feldman talked to several “long haulers” in the region about their experiences which range from physical problems to mental health concerns.

Hear the whole story on The Why
Interview highlights
Nina on Melissa Mazer’s experience
She hunkered down at home and made herself some tea and rested up, and that seemed to work. She started to feel better after about two weeks, but then after about three weeks, she started having trouble breathing. Then a week later, she started getting a throbbing pain in her neck. And around that time, a New York Times report had come out that found that in a small minority of young patients who got COVID, they were having strokes. So she called her general practitioner and she was really surprised. The doctor told her that she probably didn’t have COVID because she can’t have it for more than two weeks. Her symptoms just kept on coming and she kept a log of them in the absence of any sort of other guidance. She had a racing heartbeat. She had gastrointestinal issues. She had what a lot of people describe as like a brain fog, fuzzy memory, hard to recall words, difficulty focusing on any one individual thing for a very long time …
The pandemic is young enough that there’s only so much research that can have been done at this point to bear out people who have long-term symptoms. But there are a couple of studies that show Melissa is not alone.
Patient Jacqui Canter on the toll the virus took on her mental health
So from what I understand, I had a couple days in my room, in a regular hospital room, and I remember talking mostly to my sister and telling her that I was going to call the radio stations because they were trying to commit me. And I guess the reason I thought that was because I was hallucinating … I remember punching the security guard in the face, like I was Buffy the Vampire Slayer… turning around and falling down and watching my cell phone slide down the hall. But I didn’t know if it actually happened and nobody said anything to me. And it wasn’t until I ordered my medical chart and I got home and read it, I was like, “Oh my God! I actually did that.”
Nina on what doctors are discovering about the lingering effects
There are some clinics specifically designed to look at people with ongoing COVID-19 symptoms items starting to crop up, including at the University of Pennsylvania, which is run by Dr. Robert Kotloff. He’s a pulmonologist at Penn and the clinic opened in June …
Sometimes it turns out that the symptoms the patient comes in with aren’t necessarily a result of the virus still circulating in their system. It might be the immune system’s response to the virus or maybe a racing heart is actually a function of anxiety, not COVID. And maybe extreme fatigue is the result of somebody having taken an antihistamine to try to reduce inflammation.
I think it’s important to note that those things don’t make the symptoms less real or important to treat. But it’s just another factor for doctors in trying to figure out how to untangle all these symptoms and treat them appropriately. And I think they’re still figuring out how to do that. They’re still figuring out which symptom is a result of the virus, which is the result of the immune system’s response to the virus, and which might be a result of treatments that we’ve tried to eradicate the virus. It’s a sort of new frontier for for medicine right now that that they’re dealing with.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.









