What do I need to know about the new coronavirus variants?
How did the new COVID-19 strains evolve? Will the vaccine still be effective? WHYY’s Health Desk Help Desk looked for answers.
Listen 5:02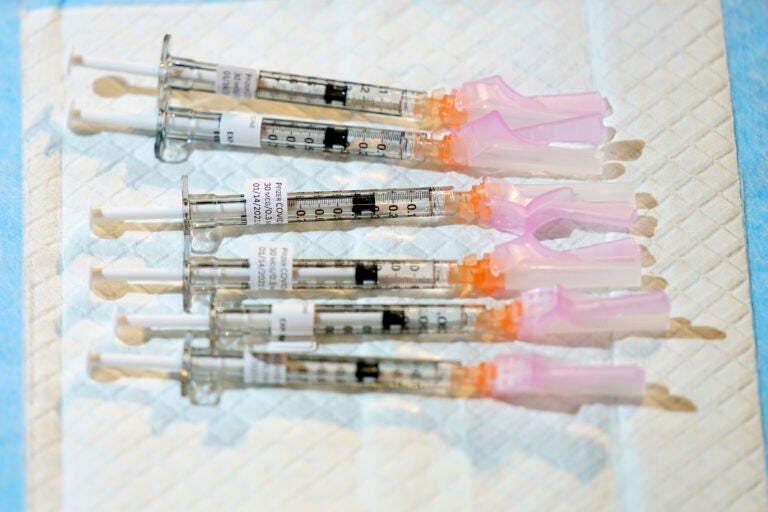
Doses of the COVID-19 vaccine are ready to be injected at Englewood Health in Englewood, N.J., Thursday, Jan. 14, 2021. (AP Photo/Seth Wenig)
This is one of a series of articles in which reporters from WHYY’s Health Desk Help Desk answer questions about vaccines and COVID-19 submitted by you, our audience.
Even as hospitals and clinics distribute COVID-19 vaccines all over the country, new — and more contagious — variants are beginning to travel across the globe.
Today, we focus on one key issue: What do we need to know about those coronavirus variants?
First things first: What is a virus variant, and where does it come from?
All viruses mutate: chickenpox, flu, even the common cold. The virus that infects one person is not going to be 100% identical to the virus that infects someone else.
That’s because in order to spread, viruses have to make copies of their own genetic material — and when they make those copies, they sometimes make small mistakes or changes. As those small changes build up, they can also change the way a virus acts, making it more contagious, or less dangerous, etc.
The new COVID-19 variants identified in Brazil, South Africa, the United Kingdom, and now potentially California are essentially new versions of the virus that have collected small changes over time. Because of that, they’re now more contagious than the version of the coronavirus we’re used to.
That brings us to our question, from a WHYY listener in Philadelphia named Cynthia Olds. She’s concerned about the variants but says she hasn’t really heard about them in the context of Philadelphia or Pennsylvania — have they identified any cases here?
Yes. On Jan. 15, officials identified a case of the U.K. variant in a woman from both Philadelphia and Bucks counties. The city Department of Public Health said she had started having symptoms of the coronavirus in late December, was briefly hospitalized, and was recovering.
But we don’t yet know for sure whether people in our area are being widely infected by the new variant. That’s because in order to identify which cases are which, scientists have to take samples from each case and compare the virus to itself — kind of like a spot-the-difference game, albeit much more complex.
One way to do that is through something called viral whole genome sequencing, where scientists isolate the RNA from viral samples and compare them side by side, to determine which changes have occurred.
Rick Bushman, who teaches microbiology at the University of Pennsylvania and serves as co-principal investigator of the university’s new Center for Research on Coronaviruses and Other Emerging Pathogens, leads a team that’s already started sequencing samples from patients at Penn Medicine hospitals. His team was the one that identified the Philadelphia/Bucks County woman’s case.
“For the U.K. strain, for example, it has multiple changes in this protein on the outer surface of the viral particle — the spike protein,” Bushman told WHYY. “And there’s increasing evidence that those changes can affect how the virus binds to cells and helps them get into human cells so that it may allow the virus to spread more commonly between people.”
So we know the variants are probably more contagious. Are they more serious? Do they make people any sicker?
They could be. Bushman said we haven’t seen any evidence indicating that the variants are more pathogenic, in addition to being more transmissible. But since the variants are still new, it’s too early to rule the possibility out completely.
That said, he added, “I’m optimistic that variants that make people sicker may not do very well long term, because if the virus is spread by respiratory [means] — coughing, sneezing all the usual stuff — then somebody has to be walking around and relatively healthy in order to be able to spread.”
In other words, there’s no evolutionary benefit for the virus to make people sicker. On the contrary, Bushman is hopeful that as the virus becomes more transmissible, it may also become more benign.
Since a variant is here in this region, should we be worried? Is there anything that we can do to avoid contracting or spreading it?
Right now, it seems like the best course of action is just to follow what we already know: Wear masks, wash hands, avoid indoor gatherings, stay physically distant from people outside our households, and so forth.
Multiple medical experts have also recommended “double masking” — for example, layering a surgical mask underneath a fitted cloth one, which adds both an extra layer of protection and a snugger fit. When they are layered properly, some researchers suggest, double masks can even simulate the effectiveness of an N95, which is still the gold standard for protection.
Is the vaccine going to be effective against new variants?
Yes. COVID-19 is still spreading and changing and infecting new people, and that’s definitely concerning, in that it could diminish the vaccine’s effectiveness slightly. But that doesn’t mean the vaccine won’t work altogether.
Even if it does become less effective, Bushman said, we’d just have an additional booster shot — maybe a seasonal one, like we do with the flu every year. Vaccine maker Moderna, for example, is already working to develop a booster like this.
“It’s not a crisis,” Bushman said. “[It’s] not the end of the world. If we have to do that, that’s what we’ll do.”

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)




