People with autoimmune issues find critical drug scarce after Trump touts it for COVID-19
Used to treat conditions such as lupus, hydroxychloroquine is in short supply for those who need it. But they haven’t been proven to work on COVID-19.
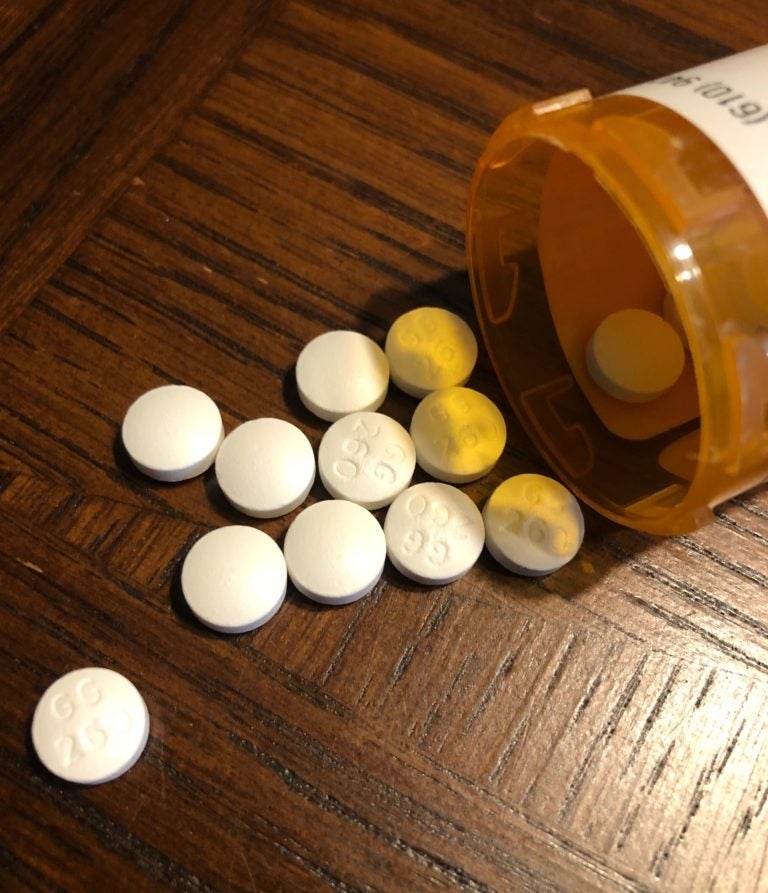
A bottle of hydroxychloroquine.(Courtesy of Susan Hauk)
Sue Hauk has 12 days before her body starts to shut down. At least, that’s what happened last time she went off Plaquenil, the drug she takes each day as a treatment for lupus.
Hauk, 48, is no stranger to pain: She wakes up each day with varying degrees of fatigue, joint aches, chest pain, and nausea — all typical symptoms of lupus, an autoimmune disease that more than 1.5 million Americans live with each day. Nearly all lupus patients are women, and the disease is at least twice as prevalent in women of color. Plaquenil is a common daily treatment to keep the symptoms in check.
But now, it’s in short supply because of its potential to work as an antiviral treatment for people with COVID-19. Though not yet clinically tested for that use, the drug — which has also been used to treat malaria for almost a century – has been in high demand since last week, when President Donald Trump heralded it in his national address as the most promising treatment prospect. Since then, pharmacists have had a hard time keeping Plaquenil in stock.
Hauk usually gets a month’s supply of hydroxychloroquine, the drug’s generic name, at a time. She wasn’t due for a refill for another week, but started seeing news reports that people with autoimmune disorders were having trouble getting their prescriptions filled.
“I thought, that can’t happen to me, because I’m on this and this is my life-sustaining drug,” she said. But when she called her local pharmacy in Conshohocken, all it could offer her was five days’ worth.
She called seven different local pharmacies and five out of state. They all told her that they were either out of stock or were only filling prescriptions for their current patients.
“If I can’t find more, once it’s out of my system I don’t know what will happen,” said Hauk. “I’m at a loss right now.”

How hydroxychloroquine works
Why might hydroxychloroquine work against COVID-19? That remains to be tested, but Sharon Kolasinski, a rheumatologist and professor of clinical medicine at the University of Pennsylvania, said scientists are working on two ideas:
- Viruses like the new coronavirus need to attach to cells to do their work. Hydroxychloroquine could make it harder for a virus to do that.
- Some patients might have died from severe cases of COVID-19 because their immune systems went into high gear to try to fight the virus — such a high gear that it started damaging the person’s own body as collateral damage, an overreaction that is called a cytokine storm. That happens in autoimmune diseases like lupus as well. Hydroxychloroquine puts the immune system back into a normal gear, reducing the damage from its attacks.
Labs across the world are setting up clinical trials to determine how well hydroxychloroquine can treat COVID-19. At the University of Pennsylvania, researchers are working around the clock to get their trial up and running.
Researchers there are also running high-throughput lab screens, in which they test the virus’s interaction with an expansive library of existing FDA-approved drugs including hydroxychloroquine. If lab results are promising with a given drug, it could move on to clinical trials.
“It would be transformative if we found a generic drug that is highly effective and had no side effects, and for which there was a global supply,” said Sara Cherry, a virologist who runs the lab. She said she hopes to have data from the tests in a couple of weeks, but cautioned against moving too quickly with any drug that hadn’t gone through the proper testing channels.
In clinical trials at Penn and elsewhere, scientists will test hydroxychloroquine in a variety of circumstances, such as whether it can be taken preventatively; whether it works in mild cases or severe; whether it can be used on intubated patients. And most importantly, whether it’s effective at all: In the first small clinical trial out of China, outcomes were about the same for the patients treated with hydroxychloroquine as the ones who weren’t. The next trial, a French study that catapulted hydroxychloroquine onto the public stage when Trump cited it, showed more promising results. But it’s been highly criticized by scientists, including those within Trump’s own administration, for its methodology.
In the meantime, hydroxychloroquine remains critical for people with autoimmune diseases, and they’re having trouble finding it.
Kolasinski said as soon as the news started spreading that hydroxychloroquine might be used to treat COVID-19, she heard from patients who were worried that they might not be able to get their regular prescriptions.
Balancing access and regulation
Scientists and public health experts largely agree that successful clinical trials are necessary before hydroxychloroquine should be prescribed for COVID-19. But regulations in some states leave room for doctors to provide it off-label for the virus.
In recent days, shortages of hydroxychloroquine have become so severe in several states that state boards of pharmacy, which regulate pharmacists, have issued emergency guidelines or restrictions on how the drugs can be given out. For example, the state boards of pharmacy in Ohio, North Carolina, and Texas say that anyone trying to get hydroxychloroquine for COVID-19 must have a prescription saying so, and cannot get more than a two-week supply. Ohio also requires a positive COVID-19 test result.
Delaware’s Division of Professional Regulation encourages pharmacies to adopt policies such as restricting hydroxychloroquine only to infectious-disease patients, limiting new prescriptions to a 14-day-supply, and limiting patients with existing prescriptions to a 30-day supply. The division notes there are reported shortages of the drug statewide.
Pennsylvania’s Department of State says that if pharmacists give people hydroxychloroquine for COVID-19, they should confirm that the patient tested positive.
The New York Times reported that some doctors are hoarding possible coronavirus treatments, like hydroxychloroquine, by writing prescriptions for themselves or family members. In a joint statement, the American Medical Association, American Pharmacists Association, and American Society of Health-System Pharmacists warned that stockpiling these drugs, or using up supplies with excessive orders, have grave consequences for patients who already use and need them.
In the wake of Trump’s misleading remarks, not only did doctors start prescribing off-label, some people took risks in the absence of any official guidance. One man even ate a form of chloroquine that is used to clean fish tanks. He later died.
Desperate for a solution
In the Philadelphia region, pharmacists reported seeing an increase in requests for off-label prescriptions from doctors, an increase in demand from patients, and low supply at the wholesale level.
“It’s like Lysol wipes — the moment it comes in, everybody’s buying it up,” said Richard Ost, who runs an independent pharmacy in Philadelphia. He said patients like Hauk might be having trouble when they call around to pharmacies where they’ve never filled their prescriptions before because pharmacists want to preserve the supply for their existing customers.
“Hydroxychloroquine has become like Oxycontin,” he said. “If you call me and ask if I have it, I’m gonna say no.”
Cindy Messerle, CEO of the Lupus Foundation of America’s Philadelphia Tri-State Chapter, said that, for everyone’s sake, she hopes clinical trials show that hydroxychloroquine is effective against COVID-19.
“I do hope that a treatment for COVID-19 is found as soon as possible,” Messerle said. “If it happens to be with hydroxycholoroquine, the important thing is that people who take it on a daily basis for lupus and other autoimmune diseases have uninterrupted access to their medication.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.


![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)