Pennsylvania leading the way in making addiction treatment more available
Opioid prescriptions have fallen by 28 percent in Pennsylvania from 2013 to 2018, but overdoses and deaths continue to rise.

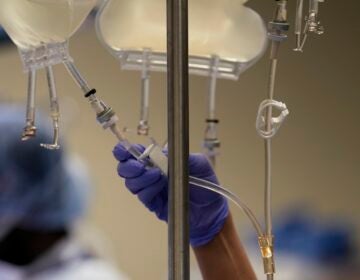
Pennsylvania Insurance Commissioner Jessica Altman talks about steps taken to ensure access to opioid addiction treatment during a visit to a Walgreens pharmacy in Kensington. (Emma Lee/WHYY)
Pennsylvania is making it easier for doctors to provide treatment for opioid addiction. That’s according to a new report released by the American Medical Association, the Pennsylvania Medical Society and Manatt Health. Approaches to combating the opioid epidemic range from prevention to harm reduction, but many solutions lie in easing regulations on treatment prescribing and tightening of restrictions on medical oversight. The new report found that Pennsylvania is leading the way in several of these areas.
While prescriptions for opioids have fallen by 28 percent in Pennsylvania from 2013 to 2018, overdoses and deaths continue to rise, highlighting the need for increased access to treatment.
In October, Pennsylvania announced an agreement with its seven largest private insurance companies that they would waive prior authorization requirements for doctors to prescribe Suboxone, methadone and naltrexone. Those are the three FDA- approved drugs to treat opioid addiction, known commonly as medically assisted treatment, or MAT. Under this agreement, the prescriptions for MAT would be covered at the lowest cost possible based on the plan. Those requirements had already been waived for patients on the state’s Medicaid plans.
Prior to this, if a physician wanted to prescribe Suboxone, a low-grade opioid that prevents withdrawal and helps curb cravings, for a patient with substance use disorder, she would have to go through an bureaucratic process that could take weeks.
“The ideal time for a patient to get treatment is when the patient says they want treatment,” said Joel Ario, former insurance commissioner in Pennsylvania and Oregon. “Patients that disappear without getting treatment may show up later in a morgue or something.”
Pennsylvania Insurance Department Commissioner Jessica Altman, who said it’s too early to gauge the effects of the waived authorization requirements, said her department will keep on eye on a couple of data points to measure the impact of increased access to MAT treatment.
“One is utilization,” she said. “How many prescriptions are being filled under that insurance?”
Another, said Altman, is cost: “How much are people paying, and how much are people saving by these medications being made available at lower cost to the patient?”
The report noted that while removing barriers for doctors to prescribe MAT is an important step, Pennsylvania, like much of the rest of the country, needs to increase the number of facilities that offer it in the first place. Just over half of substance use disorder-treatment facilities in the state offer any form of MAT, and only one in 20 offer all three forms.
The report also heralded the success of the state Insurance Department’s efforts to crack down on benefits packages that violate parity laws for substance use treatment — in other words, making sure that insurance companies are offering the same coverage for mental health and substance use treatment that they would for physical health.
The report noted Pennsylvania’s efforts in making non-opioid pain alternatives available to physicians and educating them on their prescribing potential. These alternatives can range from non-addictive pharmaceuticals such as nonsteroidal anti-inflammatory drugs and oxycodone, as well as the alternative practices of yoga and meditation.
“If all payers do is limit one form of pain relief without increasing access to another, we will only succeed at increasing patients suffering and perhaps death,” said Dr. Patrice Harris, American Medical Association president-elect and chair of its opioid task force.
At the same time, said Harris, it’s important not to enforce sweeping regulations that would force doctors to wean patients suffering from chronic pain off opioids before they are ready.
“In my visits around the country, I’ve heard from both patients and physicians [about the effects] that some of these one-size-fits-all blunt-force regulations regarding dosage limits and pill counts have had on our patients with pain,” she said.
Pennsylvania is also among U.S. leaders in providing access to the overdose reversal drug, naloxone, according to the report. Data from the state Department of Health shows that emergency professionals administered naloxone more than 12,000 in 2018 throughout the state.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.