One year, 350,000 doses later: What Penn Medicine’s vaccine rollout taught it about equity
Pop-up clinics and low-tech sign-ups provided a road map for equitable mass vaccination. Now, the health system is planning for what’s next.
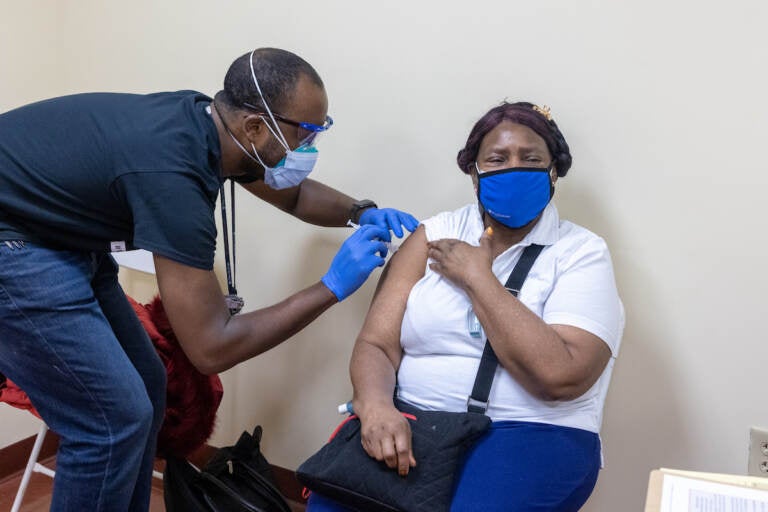
Penn Medicine vaccinates Philadelphia residents at the Church of Christian Compassion in Cobbs Creek neighborhood. (Courtesy of Penn Medicine)
Since late 2020, when the first COVID-19 vaccines became available, Penn Medicine has distributed more than 350,000 shots, with 200,000 administered in Philadelphia. That’s more vaccines distributed in the city than any other local health system or nonprofit, based on city vaccination data.
About one in 20 vaccinated people in Philadelphia received a shot from a Penn Medicine provider. And, according to the city data, the distribution of these vaccinations closely mirrored the city’s racial and ethnic composition.
Looking back recently on the first year of vaccination, Penn Medicine administrators said health equity was at the core of their approach. And with cases surging now because of new variants of the coronavirus, being local and maintaining the integrity of its clinic operation will be the focus of the next stage of the vaccine rollout.
Even before the first vaccine became available, there were barriers the health system was aware of that would affect access throughout the West and Southwest Philadelphia neighborhoods near the University of Pennsylvania, said Dr. Heather Klusaritz, director of community health services for the Penn Medicine Center for Health Equity Advancement and director of community engagement for the university’s Center for Public Health Initiatives. Access to transportation, financial issues, and community trust in health systems were already well-documented hurdles in the communities that surround Penn Medicine, she said. And throughout the pandemic, a higher burden of COVID-19 has been observed in Black, Latino, and Asian American communities.
“So we saw early on that our communities of color were disproportionately bearing the burden of COVID rates, and we knew that intersected with a disproportionate burden of access to vaccines in our communities of color,” Klusaritz said.
More than a year into the vaccination effort, a focus on health equity has yielded some observable results. Forty-two percent of all shots administered to Black individuals in Philadelphia came from Penn Medicine, according to a Penn analysis of the data. The health system also provided more than 12,000 shots to the city’s Asian American residents, ranking just behind a collection of commercial pharmacies and FEMA’s centralized mass vaccine operation.
The challenges to vaccine equity evolved, said Klusaritz, who oversees Penn Medicine’s vaccine dissemination strategy. During the first wave of vaccination and eligibility for the elderly and people at high risk of complications from COVID-19, the biggest challenge was logistical: How do you deliver the vaccine in rapid fashion to meet pent-up demand?
During this first round, stories abounded of seniors and immunocompromised individuals staying up late at night with the help of family members, desperately searching online to find a place where they could get a dose. This was a period in which Penn Medicine was trying to scale a series of mass vaccination sites to meet the need. There was an acknowledgment that not all seniors or immunocompromised people had family members or others to help them search online, nor did everyone have access to a computer or a phone to make an appointment.
“We know that to make appointments to get vaccines, many retail organizations and other systems require accessing a website, filling out multiple data fields, and progressing through a series of clicks to be able to make an appointment for a vaccine,” said Klusaritz. “And one of our fundamental principles from the beginning was a low-tech barrier.”
Administrators at Penn Medicine worked together to design a system where they could register individuals for vaccines using an SMS text messaging system so that people could use their phones instead of a computer. And if they didn’t have text messaging access on their phones, Penn offered telephone support. Then the health system worked with community partners in West Philadelphia to identify venues that could accommodate a large number of people, usually gyms and public schools. More than 100-plus volunteers would eventually come on board to build capacity for vaccinating hundreds of people during a single session.
Dr. Richard Wender is the department chair of Family and Community Medicine at the University of Pennsylvania’s Perelman School of Medicine. That period of early mass vaccination was marked by high and steady demand, he said, and as other groups became eligible for the vaccine, Penn Medicine was vaccinating hundreds and sometimes thousands of people per day.
“I think we knew that once that first wave of people who had already decided to be vaccinated passed … there would be a big drop-off in vaccines,” said Wender. “But I think all of us were a bit surprised at how rapidly it happened.”
What they learned, Wender said, was that the people who were really receptive to getting vaccinated found a way to find a dose. And the nature of the challenge for the health system changed very rapidly to making sure that people who were reluctant to get a dose or who faced a lot of barriers to getting a dose had the information and the support that they needed and the recommendation from a trusted source to be vaccinated.
“We took some of that wonderful technology that helped us vaccinate massive numbers of people and we revamped it to really host much smaller clinics and put greater emphasis on making sure that people felt that it was safe to get a vaccine and easy to get a vaccine because it was close to home or in a location that they were familiar with,” said Wender.
That second wave of vaccine efforts signaled a shift away from the mass vaccination model to hyperlocal clinics that were brought to undervaccinated and underserved communities. Those local clinics were conducted in places such as fast-food restaurants and hardware store parking lots. They had the capacity to vaccinate thousands of people but also to give doses to a handful of people at a time. And they were portable clinics, making it easy to move into different neighborhoods with flexibility.
“Philadelphia describes itself as a city of neighborhoods, and If you’re from Philadelphia, you know that there are geographic lines of demarcation where there’s either a real geographic barrier or there is an identity, community-identity barrier,” said Klusaritz. “So people won’t necessarily travel long distances outside of their community, [and] because of our high rates of poverty, people don’t have the financial resources to travel long distances outside of their [neighborhood].”
In an effort to vaccinate those who were not making it to the traditional mass vaccination sites, Klusaritz and other colleagues at Penn Medicine used city data to identify neighborhoods where there was low vaccine uptake and set up clinics there. They worked closely with school principals, churches and mosques, local businesses, and corporate partners like Philadelphia sports teams to gain the trust of communities.
“We describe May through the end of October [2021] as the marathon, not the sprint,” said Klusaritz, “where we had a continuous presence in these communities where we gave vaccines. But what we also did was just provide a lot of education and outreach, allowing opportunities for people to ask questions, get their concerns addressed.”
New challenges ahead
With vaccines now approved for ages 5 and up, Penn Medicine has recentered its efforts on vaccinating children, including school-based clinics in underserved areas. To date, the health system has hosted clinics at 21 different schools across Philadelphia, including one that administered roughly 800 shots.
“And it really was very emotional, very moving to watch 5- and 6- and 7-year-olds grapple with their own need to have a shot that, just a few months before, wasn’t on the radar,” said Wender. “And we were able to vaccinate virtually everybody who came in, including some children who were really nervous and frightened about it.”
Parents who had been reluctant about getting the vaccine for themselves earlier in the pandemic were hesitant about vaccinating their children, Klusaritz said. Beginning in summer 2021, when children 12 years and older were eligible for a vaccine, Penn Medicine began holding a series of virtual town halls and invited physicians to explain the science of the vaccine and to provide an open forum for questions.
In addition, Klusaritz said, Penn Medicine trained and worked with vaccine ambassadors, trusted people who are from the communities they serve. This special workforce has conversations about the efficacy of the vaccine with local residents in libraries, retail shops, recreation centers, and schoolyards. Though not all parents are going to decide to vaccinate their children after one conversation, Klusaritz and her team have noticed some positive results.
“What shifted when the 5- to 11-year-olds came online is that we saw that families who had made a decision [to get] their child vaccinated [decided] it was the right time for the whole family to get vaccinated,” said Klusaritz. “So that availability of the vaccine for the younger kids has really created this energy around getting family units vaccinated.”
Yet some big challenges lie ahead, Wender and Klusaritz said. The local clinic model stretches the volunteer workforce, and requires having many clinics during any given week.
“To achieve equity is to be as available as we possibly can be,” said Wender. For example, “we have to be at school during the school day, right in the middle of the week. So that puts a tremendous test for our capacity to attract volunteers.”
Now, with different vaccines and boosters, as well as a diversity of eligible groups coming to the clinics, there are significant safety challenges, Wender said. At the beginning of the vaccine rollout, there were only two kinds of mRNA vaccines being offered. That has significantly changed, and now health systems are being tasked with creating a system of safety checks to make sure that they’re matching the right vaccine with the right patient.
“We have parents, we have teachers, we’re vaccinating people who are getting their first dose,” said Wender. “We’re vaccinating people getting their second dose, and we’re vaccinating people getting booster shots. So it has been a very substantial challenge to the logistics and the safety of the clinic, which moves pretty quickly.”
Klusaritz said Penn Medicine’s health system had anticipated that not everything was going to come easily.
“We knew going into this, the context in which we were rolling out a new vaccine, the climate in the country, we knew that there was going to be hesitancy and concern, and we weren’t going to convince everyone,” said Klusaritz. “And so we wanted to take the approach of being present in a consistent fashion in neighborhoods over time, so that when people were ready to say yes, we would be there, and they’d be able to choose the vaccine.”
—
Support for WHYY’s coverage on health equity issues comes from the Commonwealth Fund.

Saturdays just got more interesting.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.




![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)





