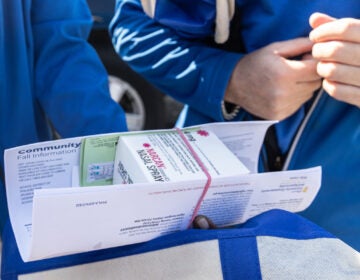
Naloxone by mail? What N.J. addiction help looks like during COVID-19
With coronavirus infections soaring, New Jersey addiction treatment providers are figuring out how to continue offering services — at arm’s length.
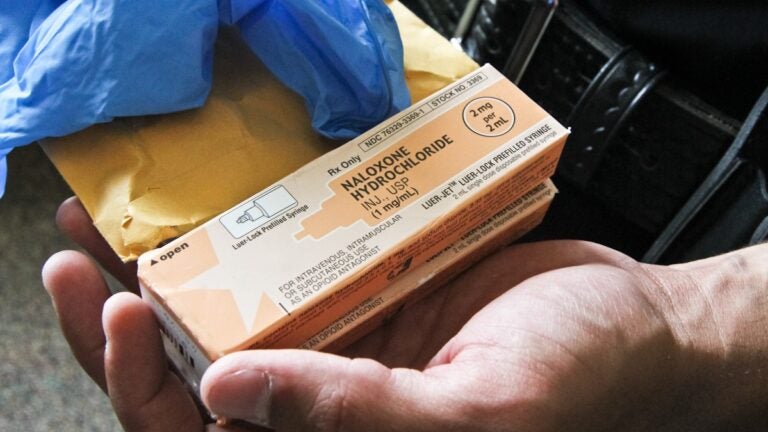
File photo: Naloxone (Kimberly Paynter/WHYY)
As COVID-19 cases continue to soar in New Jersey, addiction treatment providers who are usually in close contact with people who use drugs have been figuring out how to continue offering services — at arm’s length.
With the state’s harm reduction centers cutting back their hours and in-person consultations becoming trickier, advocates for those with addiction worry that the coronavirus pandemic may cause other public health emergencies to worsen while nobody’s watching.
“It’s sort of intensifying all of the other things that come along with the overdose crisis,” said Caitlin O’Neill, director of harm reduction services at the New Jersey Harm Reduction Coalition.
O’Neill said the increased isolation of drug users from their friends and families — whom she calls “the first of the first responders” — means more people may overdose alone. Meanwhile, emergency service workers are toiling feverishly to treat the flood of COVID-19 patients.
That’s why the Harm Reduction Coalition, which had been mailing the overdose-reversing drug naloxone to residents, ramped up its efforts after Gov. Phil Murphy issued a statewide stay-at-home order to slow the spread of the coronavirus.
“If people have naloxone in their homes, they would be able to immediately have somebody reverse an overdose, as opposed to sort of having to be triaged for care during COVID-19, because we do need those first responders for the COVID patients.”
O’Neill said the group has mailed 775 doses of naloxone since March 13 to New Jersey residents who requested it online or called 877-4NARCAN (877-462-7226).
The overdose crisis continues to ravage New Jersey. The Garden State reported 3,021 drug overdose deaths in 2019, a slight reduction from the year before, according to state data. But it saw another 789 overdose fatalities from Jan. 1 through the end of March.
And it may be harder now than ever for people who use drugs to access critical services.
Two of the state’s harm reduction centers — also called needle exchanges — have closed, and others have cut their hours amid personal protective equipment shortages.
Axel Torres Marrero, senior director of public policy and legal services at the Hyacinth AIDS Foundation, which operates three of New Jersey’s seven harm reduction centers, said his priority was to continue operating in a way that was safe for both workers and clients.
“It’s a struggle, week in and week out, but so far we’re able to do it,” Torres Marrero said.
Hyacinth’s harm reduction centers provide clean syringes, fentanyl test strips, tests for hepatitis C, and access to wound care. But Torres Marrero suggested a significant reduction in hours has meant that far fewer people are seeking out its services.
“The heroin addict is not going to be scheduling when they get their fix,” he said.
Donna Leusner, a spokeswoman for the Department of Health, said the state is ensuring harm reduction centers are stocked with naloxone and noted that people can obtain up to 10 new syringes at pharmacies.
Those receiving medication-assisted treatment may also struggle to get care, though both the state and federal government have made it easier for treatment centers to operate with fewer in-person interactions.
In March, the Trump administration relaxed the rules for MAT, allowing doctors to prescribe drugs such as buprenorphine and suboxone by phone or telemedicine rather than in-person visits. Doctors can also prescribe 28 days of take-home medication.
The state Department of Human Services has provided guidance to opioid treatment programs on how to operate safely during the coronavirus outbreak, such as implementing social distancing and hand hygiene policies, handing out medication to patients in separate rooms, and encouraging the use of telehealth and take-home doses.
Lewis Nelson, chair of emergency medicine at Rutgers New Jersey Medical School in Newark, said emergency room admissions for opioid overdoses have decreased at University Hospital in the weeks since the COVID-19 crisis began.
He said it could be that fewer people who overdose and survive are seeking care, or that relaxed rules for MAT mean that drugs like methadone and buprenorphine are more accessible on the street.
“These are unintended consequences. Often unintended consequences are bad,” Nelson said. “In this case, the silver lining is it appears perhaps that people have more access to [these drugs] who wouldn’t otherwise be engaged in a medication-assisted treatment program.”
Nelson said the hospital was seeing fewer cases of most illnesses, such as heart attacks and strokes as well, possibly because people are wary of seeking care in the epicenters of the coronavirus outbreak.
But he added that since most people who overdose don’t die, the drop in emergency room admissions “doesn’t necessarily portend that we’re going to see a huge increase in overdose deaths.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.




![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)