N.J. employers fined for COVID safety lapses amid rise in workplace deaths
Dying of COVID-19 from an infection on the job remains a threat as more workplace deaths were reported last year than in recent years.
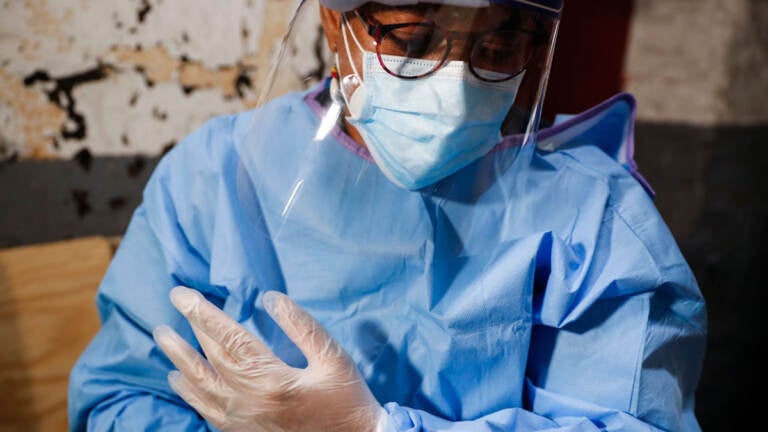
A nurse at work during the early days of the pandemic. (AP Photo/John Minchillo)
This story originally appeared on NJ Spotlight.
Cecelia Gilligan Leto often fields calls from workers concerned for their safety while they do their jobs.
As project director for the New Jersey Work Environment Council, Leto has trained people in workplace safety for years. So, when the novel coronavirus began to spread last year, workers in health care, retail, warehouses and in other occupations turned to her.
“You had this invisible thing come into the workplace; people just didn’t know what to do with it, and there was a lot to learn in the beginning,’’ she said. “COVID was a new hazard, and in February and March those calls kept coming in and the people were fearful, and they were scared.”
More than a year later as the spread of the highly contagious delta variant of COVID-19 has caused an uptick in new cases and hospitalizations in New Jersey, Leto said she’s getting calls again.
“That fear is still with us; now there is concern about who is vaccinated and who is not vaccinated,’’ she said.
COVID-19 infections were found in different workplaces last year during the height of the pandemic, leading to federal inspections at different works sites. And dying of COVID-19 from an infection on the job remains a threat as more workplace deaths were reported last year than in recent years.
Inspections by OSHA
So far in 2021, the New Jersey offices of the Occupational Safety and Health Administration have conducted 32 COVID-19-related fatality and catastrophe inspections, according to Joanna Hawkins, a spokeswoman for the agency.
Last year, OSHA conducted 180 COVID-19-related fatality inspections in New Jersey. In addition, federal OSHA initiated two employer-reported referral inspections in the Garden State in response to hospitalization reports related to COVID-19.
Inspections the agency performed between Feb. 1, 2020 and Dec. 31, 2020 led to proposed penalties on companies totaling $342,424, Hawkins said.
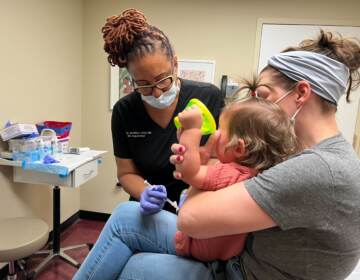
On Monday, amid growing concerns about unvaccinated co-workers, Gov. Phil Murphy mandated inoculations for all workers in most state and private health care facilities, including nursing homes and other long-term care facilities, and correctional settings.
Last month, OSHA fined Avantor Fluid Handling, a pharmaceutical company in Monmouth County, $13,653. claiming that it did not enforce mask-wearing or social distancing among employees. The federal agency said that 30 of the company’s 50 employees tested positive for the virus. In November 2020, four company employees required hospitalization, and by January, two of the workers — a husband and wife — died due to complications related to the virus. The other workers recovered.
A spokesperson for Avantor could not be reached Monday, but a spokesperson for the company told the Asbury Park Press last month that the facility for several years has operated as a sterile, cleanroom environment where employees routinely wear masks, gowns and other protective gear.
‘Failed to take precautions necessary’
“Two workers lost their lives and others were sickened because their employer failed to take the precautions necessary to keep them safe,” OSHA Area Director Paula Dixon-Roderick who is based in Marlton said in a statement. “Tragically, this case should remind all employers of the importance of fully implementing coronavirus prevention measures.”
Weeks later, OSHA announced it had found that Oaks Integrated Care Inc., a Mount Holly-based health care provider, failed to implement a required coronavirus prevention program at two of its locations to mitigate the spread of the virus following outbreaks at locations in Howell and in Lumberton.
The company failed to identify and isolate clients suspected of having the coronavirus who lived in group homes and did not adequately inform staff about the associated risks, OSHA said in a statement. The agency said that, as a result, two workers were exposed to the virus and later died.
OSHA cited the company for violations, including of the general duty clause that requires employers to ensure workplaces are free of recognized hazards that may cause death or serious physical harm. The company faces a penalty of $27,306. A call to Oaks Integrated Care was not immediately returned Monday.
The continued fines and the numbers of workers who died are not surprising to Leto and Louis Kimmel, executive director of New Labor, who organize an annual event to remember workers who died due to workplace injuries. In April, they received the list of around 250 workplace fatalities that had led to OSHA inspections. There were many more names on that list than in previous years, they said. And this time, COVID-19 was listed next to a majority of the names.
Many in hospitals, nursing homes
“Under cause of death, you’ll see COVID is all over this list,’’ Kimmel said.
Nearly 200 of those included in the list died after contracting COVID-19. Many were employees of hospitals and nursing homes and other health-care-related facilities.
“COVID has been the biggest health and safety hazard that has affected the workforce, and it has been an invisible hazard,’’ said Leto said. “When you see these numbers, they are terrible but I think they are higher than that; there are many people that didn’t realize where they got it from, it probably came from work.”
On its website where OSHA posts COVID-19 deaths that it investigated, OSHA said the worker fatalities were reported by employers who designated them as being related to COVID-19. The list includes cases where no conclusion had been made that the worker contracted COVID-19 from occupational exposure, the agency notes. And even though these fatalities were reported by employers, the agency notes it does not necessarily mean that any OSHA standard was violated.
Still, the numbers listed by OSHA for the first year of COVID-19 are higher than the workplace deaths that occurred in previous years.
In 2018, there were 83 reported deaths and 74 fatalities counted in the workplace in 2017 in New Jersey by the Bureau of Labor Statistics. The bureau counts deaths related to fatal injuries in the workforce, said Martin Kohli, chief regional economist for the Bureau of Labor Statistics in New York.
“Our fatality data is just injuries and not illnesses, so we are not going to pick up people who got COVID or died from COVID at the job,’’ he said.
Father of a teenager
Among those who died of COVID-19 early in the pandemic was 52-year-old John Cofrancesco, of Bergenfield, the father of a teenage son and the administrator of a nursing home in Montclair. Cofrancesco battled the illness for a few weeks at home before he went to Englewood Hospital where he tested positive for COVID-19. He died March 19, 2020 a few days after arriving at the hospital, his wife Angela Cofrancesco, said.
Angela Cofrancesco, who also contracted COVID-19, said she was told that her husband was among the first dozen confirmed cases in the state. OSHA representatives contacted her at one point concerning the death of her husband, she said. She also said that her husband’s infection was traced back to the nursing home.

“I think it was the end of February when he shook someone’s hand; it was a visitor from the nursing home,’’ she said. “That’s what they told me, but who knows really what happened. We were in a pandemic.”
Debbie White, president of the Health Professionals and Allied Employees union, said the union filed 26 complaints with OSHA based on reports that its members were not getting personal protection equipment early in the pandemic. She said even though the OSHA complaints took a while to resolve, they led to citations and eventual changes that are aimed at helping workers keep safe.
“Employers were mandated to develop plans of correction to address the issues, and we have seen things change in our work environment,’’ White said. “We have seen employers go back to regular fit testing [of respirators] … stockpiles are back at the state level and at the employer level, and we have seen a lot of our issues addressed and corrected.”
But, White said, the delta variant makes it even more important for employers to take steps to ensure the safety of their workers. She said she also wants New Jersey to reinstate the mask-wearing mandate.
“We need to go back to those strategies, we need to go back to masking, we need to go back to requiring the public if you are going to my place of employment, wear a mask,’’ White said. “It’s like we discarded all those precautions that would help us that would aid in reducing the spread.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)