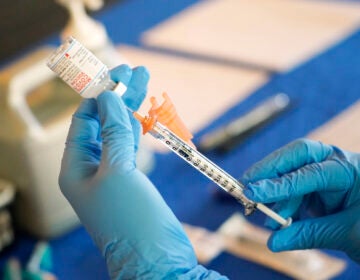
I got the COVID-19 vaccine. What’s safe for me to do now, and what isn’t?
What does “fully vaccinated” against COVID-19 mean? WHYY’s Health Desk Help Desk looked at the new CDC guidelines, and some specific situations.
Listen 4:49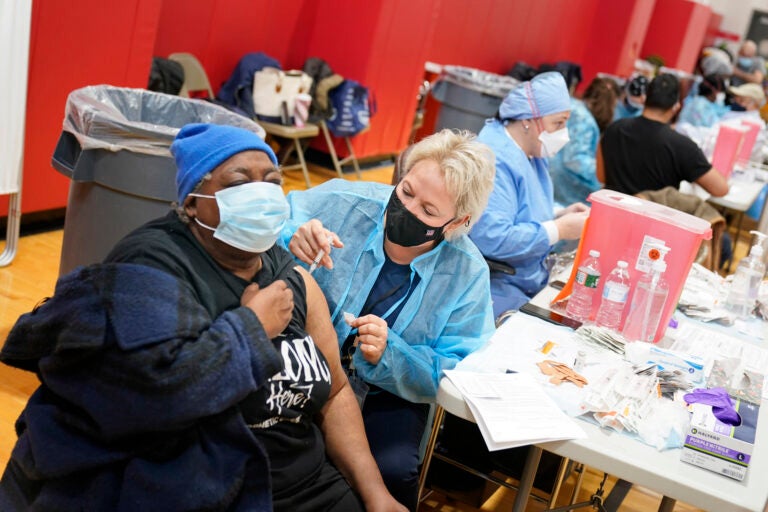
Mary Jenkins, left, receives the COVID-19 vaccine in Paterson, N.J., Thursday, Jan. 21, 2021. (AP Photo/Seth Wenig)
Ask us about COVID-19: What questions do you have about the coronavirus and vaccines?
This is one of a series of articles in which reporters from WHYY’s Health Desk Help Desk answer questions about vaccines and COVID-19 submitted by you, our audience.
Catherina DePaz of Philadelphia longs to gather with her family over the dinner table for the upcoming holiday. It’s been a whole year since they’ve been able to engage in their favorite traditions because of COVID-19 fears.
Now that vaccines are being administered, DePaz is hopeful her family will have a real Easter in a few weeks.
“This would be the first holiday we would have been together since 2019. Easter is a big deal to us. There’s a lot of cooking, gathering around the table, Easter egg hunts for the kids. So, it’s a special family tradition for us. And it was really hard last year not to be together, and little did we know we would miss every major holiday,” she said.
“My heart broke when I couldn’t eat my mom’s potato salad,” DePaz said with a laugh. “So it would be really special. And when I got the vaccine, I actually cried. It was that glimmer of hope that made me get really emotional that this could possibly be coming to an end.”
After a year of physical distancing and mask-wearing, many of us are itching to get back to normal. People are getting vaccinated slowly but surely, so WHYY’s readers and listeners have questions about what they can do safely — and what they can’t.
___
How much protection does partial vaccination offer? If I get the first shot of Moderna or Pfizer, but I haven’t had my second shot, am I protected?
People get some immunity after the first dose. During clinical trials for the Pfizer and Moderna vaccines, researchers reported that the first dose was about 50% effective at providing protection from COVID-19. But people aren’t fully protected until after the second dose.
“In the clinical trials, there was some reduction in COVID-19 disease starting around Day 12 or 14 after the first shot, and that persisted after the second shot,” said John Wherry, director of the Institute for Immunology at the Perelman School of Medicine at the University of Pennsylvania.
“What we don’t know from the clinical trials,” Wherry said, “is how long that protection after the first shot might last, how effective it is against actually being infected, and how well it might work against some of the variants that are now circulating widely.”
Once I’m fully vaccinated, can I meet with people right away?
A person is not fully protected until two weeks after getting the second dose of the Moderna and Pfizer vaccines, or after the single-dose regimen of the Johnson & Johnson vaccine. That’s because two weeks, or 14 days, is about how long it takes the body’s immune system to build a strong antibody response.
“Typically what happens when you stimulate the immune system is it takes a few days to get some of the cells mobilized, and to get everybody quite literally talking to each other as part of the immune system,” Wherry said.
“And then it takes about another week, or 10 days, for those responses to really mature for the cells of your immune system to start making very high levels of antibodies. And that’s really what likely protects you from infection.”
What is safe to do after the wait period?
The Centers for Disease Control and Prevention guidelines say fully vaccinated people can meet one another indoors, without physical distancing and masks.
Syra Madad is a New York City infectious-disease epidemiologist. She said she felt very safe visiting her parents maskless two weeks after she — and they — had gotten their final doses.
She met her parents indoors. They hugged. They shared a meal.
“If I’m infected with COVID-19 and passing it to them, or vice versa, the chance is extremely low,” she said. “We’re getting more and more information, studies both in the lab setting as well as in the real-world setting, that show the reduced risk of transmission of the virus if you’re infected and you’ve been vaccinated … and so looking at it from that lens, I felt very comfortable seeing my parents without any restrictions.”
What if I’m vaccinated, but my friends or family aren’t? Is it safe to meet?
DePaz and her sister have received the vaccine, but their parents and brother have not.
“I would want to know if I would need to wear a mask around them? If our doors were open, would we need to wear a mask? If it was a nice day on Easter, could we eat outside and be in close proximity?” she said. “How many people could be there? I have a partner, my sister has a partner, my brother has three kids.”
Fully vaccinated people can potentially meet with someone who has not had the shot, the CDC says. They can do so indoors and without masks if the unvaccinated person is not at risk for severe illness from COVID-19.
When meeting someone who could become seriously ill from COVID-19, such as an older person or someone with a chronic health condition, masks must be worn, and a physical distance of 6 feet must be maintained.
Wherry said people should risk-strategize when considering meeting others.
“I think whenever you have a mixture of non-vaccinated and vaccinated people, everybody should still be following the masking, social distancing guidelines. I think when you’re talking about family gatherings or small groups of people … if the more vulnerable people in the group are fully vaccinated, it may be reasonable to relax some of these guidelines a bit during those interactions,” he said. “[But] if one of the parents is in a high-risk group, immunosuppressed, or a cancer patient, we still may want to be more careful about interactions with other people who aren’t vaccinated.”
Wherry said that’s because, though it is unlikely, there is some concern that even vaccinated people can at very low frequency still get infected and transmit the virus.
A vaccinated person should also consider factors like job or lifestyle before meeting unvaccinated friends and loved ones. For example, a vaccinated health care provider could still be exposed to COVID-19 at work, so there’s an increased risk of spreading the virus.
Wherry recommends that groups stay small.
“I think we probably want to advise people to limit things to what you would call first-degree relatives, and try to keep family units relatively small,” he said.
What about nursing home visits?
Last week, the Biden administration revised guidance for nursing home visitation. The recommendations allow people to visit individuals living at nursing homes whether either party is vaccinated or not.
However, the guidance suggests that visitation should be avoided if the facility is located in an area with a COVID-19 rate higher than 10% and fewer than 70% of residents have been fully vaccinated. If residents have COVID-19 or are in quarantine, visitation should be limited, according to the guidance.
Although indoor visits are allowed, federal officials still say that outdoor visits are preferable, even when nursing home residents have been vaccinated. If residents are fully vaccinated, they can have close contact with their visitors, including touch. However, they should continue to wear masks and wash hands afterward. Visitors should physically distance from other residents and staff in the facility.
How long does the vaccine protect us?
Jacqueline Schaefer of Philadelphia wants to know if her parents will be protected by the vaccine six months from now, or if their immunity will decrease over time.
“Do I need to be more cautious as time goes on?” she asked. “It would mean everything to see my family and not have to worry about getting someone ill, or getting ill, or someone ending up in the hospital.”
The simple answer is we don’t know yet, Wherry said.
“We are probably just about to start getting data from the very first people in the Phase One trials, about a year out from vaccinations. So far, the projections from what we’re seeing is that immunological memory, so that long-term protection, probably is going to be pretty durable,” he said.
“I think most of us are estimating that, one year, two, three years, most people are still going to be protected. Will we need a booster in three years or five years? It’s too early to say. But right now it looks like we can expect to have a pretty high confidence out of the 12- to 18-month mark, based on extrapolating from information we have now.”
What about other activities? Like going out to dinner, or going to the gym?
The risk of participating in those activities is much lower when fully vaccinated, according to the CDC. But the agency does still recommend wearing masks, hand-washing, and maintaining a 6-foot distance.
“My opinion is that people can feel a little bit safer with some of these activities. I think it’s still very important in this sort of public setting to be following masking and social distancing guidelines. But you are clearly at a much lower risk once you’re vaccinated,” Wherry said.
“Indoor dining would be one … If you’re vaccinated and the person you’re dining with is vaccinated, you’re not really at a high risk for getting disease.”
But Madad said it’s not just about personal risk.
“You’re looking at it from the lens of those people around you … because this is a mixed gathering of people that may be vaccinated and people that may be unvaccinated,” Madad said.
“You want to invoke the precautionary principle, continuing to abide by the public health guidance — that is, until we have more people that are vaccinated in our general community.”
What if I was exposed to someone who tested positive for COVID-19?
A fully vaccinated person does not need to quarantine or get tested, as long as symptoms aren’t present, the CDC says. If a person has symptoms — fatigue, fever, cough, shortness of breath, loss of taste or smell — or they test positive for COVID-19, they must self-isolate for 10 days.
For those who live in congregate settings, the risks are higher. In that case, the CDC recommends quarantining for 14 days and getting tested, even without symptoms.
“If you’re wrong on the side where you’re being overly cautious, you lose people’s activities a little bit. If you’re not conservative enough, people could get infected and die,” Wherry cautioned.
He said if a vaccinated person is exposed to COVID-19 and has no symptoms, they can safely go to work wearing a mask and if they physically distance themselves from co-workers. But if they have Easter, Passover, or other upcoming plans with elderly parents who aren’t vaccinated, they should “just get tested to be sure.”
It looks like things are getting back to normal. Does that mean mask-wearing and physical distancing are a thing of the past?
Not at all; even if you’re fully vaccinated, you should continue to wear a mask and maintain physical distance in public — that’s to protect the people around you, who might not be vaccinated or have a risk factor for severe illness from COVID-19. The CDC also advises against participating in medium to large in-person gatherings. And people should follow travel advisories and various other precautions.
Eventually, once more people in the community have been vaccinated, cities and states will be able to start loosening restrictions, Madad said. Those restrictions should be more like a dial than an on-and-off switch.
“As more and more people get vaccinated, as we build more herd immunity … as hospitalizations continue to decline, as community transmission continues to decline,” officials will be able to ease distancing and masking requirements, she added.
Wherry said friends and families need to have open conversations about their vaccine status to prevent COVID-19 infection. He also cautions that, in public, it’s impossible to know who has gotten the shot.
“I think we still have to try to mask and socially distance going to the grocery store and doing other activities where it’s not clear who is vaccinated and who is not,” Wherry said.

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)