COVID-19 can spread without people showing symptoms. How do we prepare for that?
It’s unclear how many people might pass the coronavirus along through asymptomatic spread. WHO estimates range as high as 41%. One study put it at 81%.

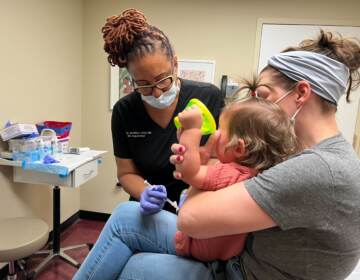
Mary Mack, right, a resident of senior housing, is tested for COVID-19 in Paterson, N.J., Friday, May 8, 2020. (AP Photo/Seth Wenig)
Are you on the front lines of the coronavirus? Help us report on the pandemic.
Back in early April, a team including Scott Goldberg, an emergency medicine physician at Brigham and Women’s Hospital in Boston, was preparing to move all the residents of one nursing home into other facilities, so that the space could be used as a center dedicated for COVID-19 patients.
Goldberg and his colleagues decided they would test every resident for the coronavirus, just to be sure they were not inadvertently sending people with the virus to the other facilities. The nursing home had no reported, or even suspected, COVID-19 cases. It had been closed to visitors and had followed all recommended social distancing guidelines at that time.
When the tests were performed, about 54% of the nursing home’s residents tested positive for COVID-19.
“This was really alarming,” Goldberg said. “I think that we were expecting a few cases, and that’s why we did the testing, just to be sure.”
Of course, the team did not end up moving those residents to other nursing homes, and they separated the facility into COVID and non-COVID floors. Goldberg and his colleagues recently published their findings in a research letter for the Journal of the American Medical Directors Association, with more follow-up data on those patients forthcoming.
“If there is COVID really anywhere in the community, then you have to assume that anybody could be positive, with or without symptoms, and this has pretty dramatic implications across our whole health care system,” Goldberg said.
It’s still unclear how many people will be infected by the novel coronavirus without ever developing symptoms — which is known as asymptomatic spread. Maria Van Kerkhove, technical lead for the World Health Organization’s health emergencies program, said estimates range from 6% to 41%, but some studies, like one of people on an Antarctic cruise, have found a rate as high at 81%, as reported by NPR.
With states lifting lockdown restrictions and more people returning to their workplaces and resuming social and shopping routines, asymptomatic spread could become a serious concern.
Early on, a lot of businesses that stayed open, including Amazon warehouses and health clinics, screened employees for symptoms, doing temperature checks and asking whether they had been coughing or had trouble breathing.
A doctor who worked at a primary care clinic outside Reading said that back in early March, the clinic, like many others, didn’t have universal masking guidelines yet, and some of the staff were worried about the early reports of asymptomatic spread. (The doctor, who did not have permission to talk about the clinic, asked not to be named in this article).
The doctor remembered a conference call from that time “when this medical assistant, who had maybe been there for a couple months, and just graduated from medical assistant school … said, ‘But if I’m seeing these patients and I get it and there’s asymptomatic spread, how do I know I’m not giving this to patients?’”
“And that this would occur to a medical assistant, that precautions that were being taken seemed inadequate, I found really striking,” the doctor told WHYY.
That, the doctor said — and Goldberg concurred — is why it’s important to keep wearing masks to protect the people around us and to continue following social distancing guidelines. It worries them when they see people not doing those things.
Research on asymptomatic spread also shows that screening people only based on symptoms is not enough, said Monica Gandhi, a professor of medicine at the University of California, San Francisco. She and her colleagues called asymptomatic spread “the Achilles’ heel of COVID-19 pandemic control through the public health strategies we have currently deployed” in an editorial for the New England Journal of Medicine in late May.
Aside from wearing masks and social distancing, Gandhi said, the United States should focus on mass testing for vulnerable and enclosed populations, such as people in nursing homes, jails, mental health facilities, homeless shelters, and hospitals — what Goldberg and his team did for that nursing home in Boston – “as opposed to saying, ‘OK, we’re going to test every human being in this country every week.’”
In early June, Pennsylvania called for universal COVID-19 testing for nursing homes by no later than July 24, but it is not mandatory, as Spotlight PA has pointed out in its reporting.
Overall, the U.S. is still not up to doing the 900,000 tests a day recommended by the Global Health Institute at Harvard University. The Washington Post reported in mid-May that while some states struggled to test enough people, others struggled to get more people to take tests.
What can people do if they’re worried about asymptomatic spread as they go back to work, shop, and ride public transit?
Check for the following, said Tista Ghosh, an epidemiologist and senior medical director for the health care company Grand Rounds: Are all employees and customers wearing masks? Is there hand sanitizer at the door? Are customers social distancing? Are gyms wiping down equipment every time someone uses it?
Ghosh has consulted for various businesses about reopening and changing workplace layouts and policies to keep staff — including film crews and insurance agents — safe.
“I would suggest that people really, as we start to reopen, take the asymptomatic spread guidelines seriously — wearing the mask and hand-washing — because the last thing we want is to have to shut down again.”

Show your support for local public media
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.




![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)