Genetic tests help parents avoid passing on serious diseases
Listen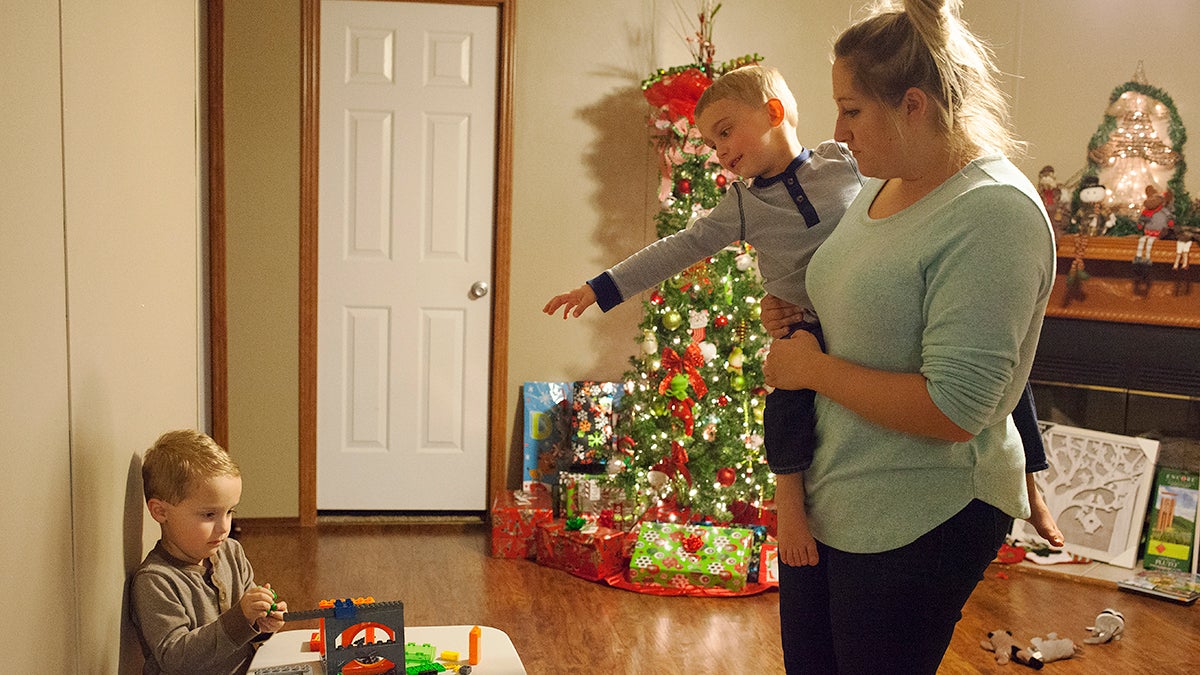
Emily Brooks with her sons
In 2009, Emily Brooks was newly married and eager to start a family. Then her dad, after years of symptoms, was diagnosed with Huntington’s disease.
In 2009, Emily Brooks was newly married and eager to start a family.
Then her dad, after years of symptoms, was diagnosed with Huntington’s disease. Huntington’s is a hereditary brain disorder, which, over time, kills brain cells. Usually symptoms start in adulthood and eventually result in diminished physical and mental ability. People with Huntington’s live an average of 10 to 25 years after symptoms begin and they have a 50-50 chance of passing the disease down to their children.
Emily and her husband put their plans on hold until she could get tested for the disease.
She tested positive in 2011. Her brother chose not to get tested, and her sister tested negative.
“My mom cried for a long time, even my dad. She said, ‘I don’t know the route we would have taken, but I’m very sorry.’ My mom still cries a lot about it,” Brooks said.
When 29-year-old Brooks was born, there wasn’t much her mom could do about preventing Huntington’s, even if she’d known her husband was a carrier. But Brooks was able to take advantage of special measures to make sure her children would not have Huntington’s.
Early tests
Just before Christmas, the Brooks house in rural Alabama was already littered with opened gifts. Construction sets, legos, and toy trucks occupied an otherwise sparse playroom. Nash and Tate, four-year-old twins, wielded swords.
“They battle with everything,” Brooks said. “Best friends and worst enemies. All at the same time.”
Nash is a little taller, bossier, gets in trouble at school and pinches and bites and kicks and screams. Tate is gentler, plays well with others, an easygoing child. “So they’re a very good balance,” Brooks said.

Nash and Tate play with their new toys. Their mom had IVF so she could test their embryos for the genetically inherited Huntington’s disease. Both of the boys are negative for Huntington’s. (Irina Zhorov/WHYY)
She always knew she wanted to be a mom, and that she wanted to be pregnant at least once. But she also knew, with certainty, that she didn’t want to pass her Huntington’s on to her kids.
“As long as I know they don’t have Huntington’s, then from there on, it’s just the luck of the draw as it is with everybody,” she said.
Her doctor recommended a test that almost guarantees the disease would end with her in the Brooks family. Researchers first performed such tests in 1990 and the technology has evolved rapidly since then.
It starts with invitro fertilization, or IVF. In IVF, doctors combine male sperm with female eggs in a laboratory. After an embryo forms and grows for five days, they place it into the woman’s uterus.
But, in Emily’s case, before placing the embryo in her uterus, doctors screened the embryo’s genetics. A technician uses a laser to make a small hole in the shell of the embryo. Then, another fine instrument goes through that hole and sucks out cells from the layer that will eventually become the placenta.
Technicians take five to six cells out of the approximately 100 that make up the five-day embryo.
“If you gave a sample of blood for genetic testing, that’s like a million cells. So there’s just no comparison in the magnitude,” said Dr. Anuja Dokras, a fertility expert at the University of Pennsylvania.
The cells are sent to a special lab that can work at that scale. Because there’s so little genetic material in those few cells, the first thing the lab does is replicate the DNA, so they have more of the stuff to work with.
One of the tests the lab then performs is called preimplantation genetic screening, in which staff check the embryo for the proper number of chromosomes. An incorrect chromosome count can cause conditions like Downs syndrome, Edwards syndrome, or Patau syndrome.
They can also take an even closer look at specific gene mutations in a test called preimplantation genetic diagnosis.
This test is usually done for conditions that are “lethal or very much associated with disabilities, chronic illness, where they don’t want to have another child with the same conditions, they’ve had deaths in the family with those conditions,” said Dokras.
The lab staff find the mutation on the chromosome, and check whether the embryo inherited the bad gene from the mother or the father. They can tell that by examining the DNA sequences around the gene, a marker that’s inherited alongside the gene. If you know who has the bad gene to begin with, it’s possible to trace the lineage and figure out if the embryo carries a normal one or not.
Labs can now test for more than 6,000 genetic conditions, like Cystic Fibrosis, Spinal Muscular Atrophy, and Huntington’s.
“But the limitation is we don’t have a gene for everything. We don’t have a gene for diabetes, we don’t have a gene for autism, there are so many of these controversial conditions people do want to avoid in the next generation but we can’t offer that because we need a single gene that’s associated with it, not a complex condition,” Dokras said.
Ethical questions
The technology sounds like a great option for families like this one, right? But, like any biomedical technology, it brings up some ethical questions.
In the U.S. there are no federal legal restrictions on using such testing to choose the sex of the embryo, for example. Some believe that could enable sex preference in families. Even the ethics committee of the American Society for Reproductive Medicine (ASRM), the medical society that oversees the industry, couldn’t come to a consensus on whether clinics should offer this service. That’s unusual. As a result, clinics can make their own decisions on whether they offer testing for sex when it’s not medically necessary.
For Judith Daar, who chairs ASRM’s Ethics Committee, a bigger issue is access. Insurance often does not cover IVF or the genetic testing, which together can cost around $20,000 per cycle. For many women more than one round of IVF is necessary before they have a successful pregnancy.
“Families that have a pedigree of genetic disorders that can be quite devastating that want to avoid the birth of a child with that disorder who don’t have insurance for IVF, may not be able to do so,” Daar said.
For Emily Brooks and her husband, in Alabama, it meant taking on loans and some help from their parents.
“People always ask, when are you going to have more kids? And we’re like, when we pay these two off!” Brooks said. (The family did recently finish paying off their loans.)
Doctors took 17 eggs from Emily, and tested 14 of the embryos that formed. “Nine or ten were positive for Huntington’s. And then we had four that were good. So of the four we put in, we did a fresh transfer, and we now have Nash and Tate,” she said.

Emily Brooks plays with her children, Nash and Tate. (Irina Zhorov/WHYY)
After the birth of the twins, Brooks had tubal ligation, so she won’t have any more kids without another medical intervention.
The process wasn’t without heartbreak for the family. They missed the giddiness many parents experience in discovering a natural pregnancy, didn’t have as much guesswork. They also, as devout Christians opposed to abortion, struggled with the loss of all those other embryos.
“I chose my kids’ wellbeing over my spiritual wellbeing, and that’s okay,” Brooks said. They prayed over the remaining embryos and then donated them to science.
Meanwhile, the whole Brooks family participates in studies for Huntington’s, and Brooks takes an anti-depressant to help her cope with her always-looming diagnosis. She sees her dad declining and knows she’ll follow a similar course.
“I try to have extra patience with my dad so that somebody will pay me that patience one day when I’m in that situation,” she said.
But she said she doesn’t regret doing things this way.
“It was a very good decision for our case and for our family and for my kids and their future,” Brooks said. “Mine may not be as bright, but theirs can be, and so I just have to focus on the good times that I have and try not to dwell on what we don’t know. And hopefully they’ll come up with a cure. Hopefully.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



