The sounds of blood pressure: What are we listening for?
Blood pressure. It's one of the most important measurements in medicine. And yet, taking it correctly is kind of an art.
Listen 4:06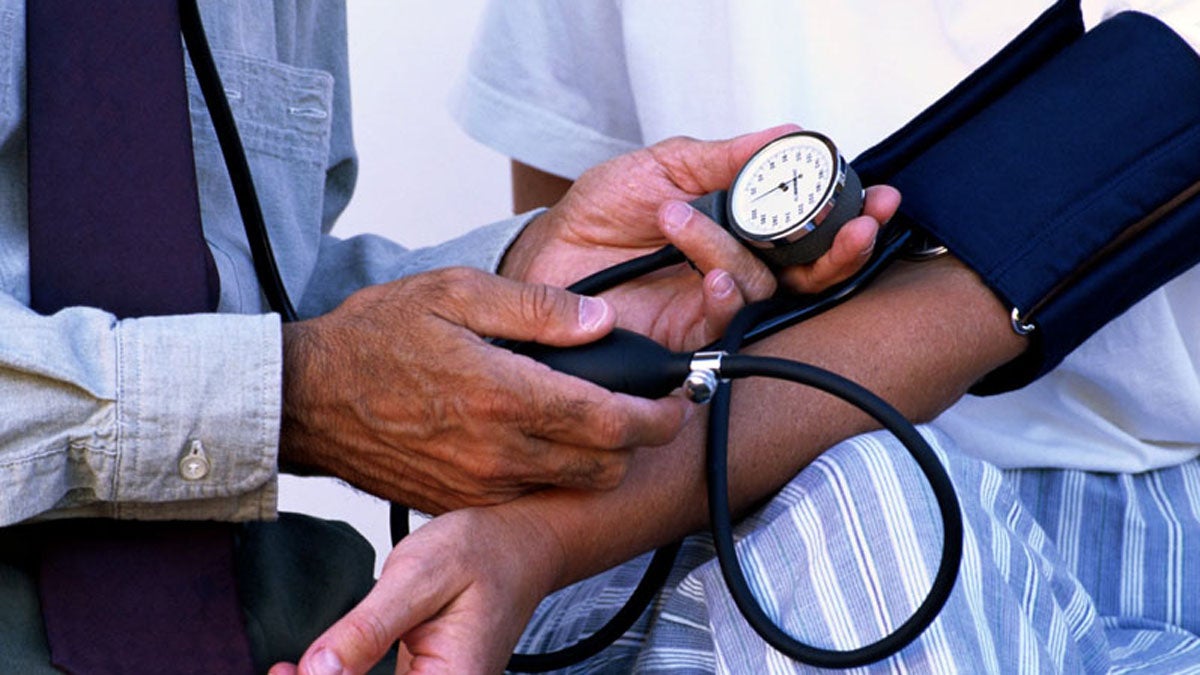
Ever wonder what doctors and nurses are listening for when they are manually taking your blood pressure? (Photo via Wikimedia Commons)
Blood pressure. It’s one of the most important measurements in medicine. And yet, taking it correctly is kind of an art. It’s fluid, it changes, and it can be impacted by something as simple as being at the doctors’ office.
The set up
“So feet on the floor, back supported, arm at a heart’s length and supported,” says Dr. Keith C. Ferdinand, a cardiologist at Tulane’s School of Medicine in New Orleans.
Ferdinand means business when it comes to taking blood pressure.
“No smoking, no eating, no drinking, no talking,” he advises to patients.
And to all the health staff, he adds: wait at least five to 10 minutes before taking the blood pressure.
How it works: systolic
So now, imagine that velcro cuff being wrapped around your arm.
“We’re looking to have the blood pressure cuff to be about 20 percent longer or wider than the circumference of the upper arm,” explains Deborah Becker, a longtime professor of nursing at the University of Pennsylvania and chair of the school’s simulation lab.
Once that’s secured, one can see that the cuff is connected to a tube and an air pump. It’s also connected to a manometer, to tally the measurements.
With earbuds in place, the doctor or nurse places a stethoscope on the inside of the arm, over the brachial artery, near that blood pressure cuff (if they’re measuring it manually).
Then they listen.
“Lub dub, lub dub, lub dub,” Ferdinand mimics the sound of the heartbeat.
At first, he and others would hear as blood pumps from the heart through the artery (the force of your blood against your arteries is the blood pressure).
Then, as they pump air into that sleeve, the cuff gets tighter and tighter, squeezing your arm until it occludes the circulation in that artery…
Silence.
Ferdinand or Becker then hear nothing.
They’d pump a few more bits of air into the sleeve, and then they’d slowly start to release it.
Wait for it…
“Doom, doom, doom!” Ferdinand mimics the thumping sound of the heartbeat, the sound of blood rushing through the arteries.
This first sound is the systolic blood pressure, the point when doctors or nurses check the gauge or meter for a reading. It’s the 120 if your blood pressure is 120 over 80.
It represents the heart contracting, pushing the blood out against the artery in that arm.
“The higher the blood pressure value, that top number, the harder the heart has to contract to get it out,” says Becker.
How it works: diastolic
That’s the top reading. But Becker and others are also listening for something else.
“As the blood starts to run off, it makes a tapping sound, a dull tapping sound and the blood disappears,” says Ferdinand.
Some describe it as a ‘swooshing’ sound that then fades out.
“And when that sound disappears, that’s the diastolic or the lower blood pressure,” he says.
When everything goes silent again, when your heart is at rest in between beats, that’s the diastolic pressure. It’s the lower reading, or the 80, if your blood pressure is 120 over 80.
Some history
These units of pressure represent millimeters of mercury, but Ferdinand says that’s more or less a throwback to the old way of measuring blood pressure.
“Those that have a little age on you remember you go to the doctor’s office and there on the wall, there’d be this gleaming silver metal inside a glass tube,” he says. “That’s how the blood pressure was measured.”
It was a column of mercury that one could see pulsate when the pressure was being taken. It was accurate, but it was dangerous. If it ever fell and broke, which would happen, then you’d be left with a highly toxic substance scattered all over the place.
Nowadays there are mechanical and manual alternatives.
Of course, none of this – not even a stethoscope – was available in 1733, when the first blood pressure experiment took place.
This was when Stephen Hales, a curious country parson in England, described in Volume II of his Statical Essays, his attempt to take the pressure of a middle-aged mare in 1733:
“In December, I caused a mare to be tied down alive on her back; she was fourteen hands high, and about fourteen years of age; had a fistula of her withers, was neither very lean nor yet lusty; having laid open the left crural artery about three inches from her bely, I inserted into it a brass pipe whose bore was one sixth of an inch in diameter…I fixed a glass tube of nearly the same diameter which was nine feet in length: the nun tying the ligature of the artery, the blood rose in the tube 8 feet 3 inches perpendicular above the level of the left ventricle of the heart;…when it was at its full height it would rise and fall at and after each pulse 2, 3, or 4 inches…”
Back to the present…RELAX
High blood pressure, especially, can stretch and damage the walls of the arteries, making the heart pump even harder and in turn, be a major risk factor for serious complications like heart disease and stroke.
It’s why Dr. Ferdinand and others place so much attention on getting that measurement right.
“It’s one of the most important maneuvers done in clinical medicine,” he says.
Yet, because so many factors can affect a person’s blood pressure at any given time, Becker doesn’t hedge all her bets on any one reading in isolation.
“We kind of look at blood pressure over time as an average,” she says.
Ferdinand advises for those who are feeling anxious, not to get it measured right away.
“It’s going to be a little high,” he cautions.
So no pressure. Relax!
Ferdinand says instead, wait a few minutes. Some even recommend, when appropriate, that a patient measure it again at home. Becker’s technique: asking patients about his or her week to provide some benign distraction.
So perhaps as anxiety and stress might build, in those moments or minutes before a doctor or nurse enters that exam room, one could maybe find some solace flipping through that six-month-old Time magazine that’s probably on the table.
Or think about your cat?
Whatever you think might work to help you relax.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.





