Stimulant use on the rise in Pennsylvania, new report finds
The data from Gaudenzia represents over 14,000 people treated at its facilities in 16 Pa. counties, Delaware and Maryland in FY2021.

This photo provided by the Cannon River Drug and Violent Task Force shows a box containing methamphetamine. (Cannon River Drug and Violent Task Force via AP)
A new report from the largest nonprofit drug rehab provider in Pennsylvania found that over the last year people entered treatment more often for stimulants and alcohol, and less often for opioids.
The trend is not an indication that fewer people are using opioids, according to the report’s authors, but rather a sign that more people are using multiple substances in combination, said Gaudenzia CEO Dale Klatzker.
“Simply put, more people are becoming addicted to more types of substances, and more people are dying because of it than ever before,” he said.
Gaudenzia has 43 programs and facilities in Pennsylvania spanning 16 counties. It is also the largest nonprofit treatment provider in Maryland, and has facilities in Delaware.
The report gathered data from more than 14,000 people served by Gaudenzia in fiscal year 2021 across all its treatment facilities.
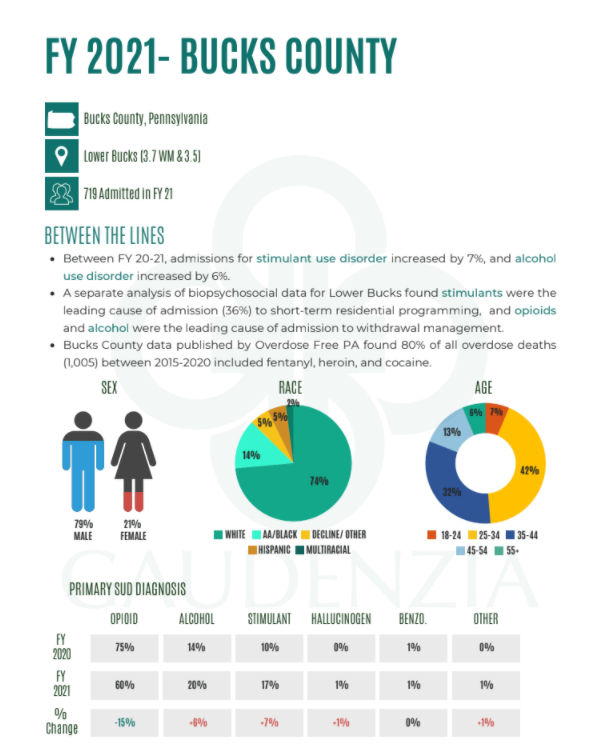
In Bucks County, where Gaudenzia’s facility admitted more than 700 people in FY21, the number of people whose primary substance use diagnosis was stimulant use disorder increased by 7%, while those whose primary diagnosis was opioid use disorder declined by 15%. The number of those entering treatment with alcohol use disorder also grew, to 20% from 14%.
The most notable stimulant increase was in Lancaster County: More than 20% of people there were admitted for stimulant use, though the facility admitted fewer than 50 people.
Stimulant use disorder also increased substantially in Erie and Fulton counties. In Schuylkill County, half of those admitted to treatment are now there for stimulant use disorder.
Philadelphia showed very little change in the primary diagnosis for those entering treatment between 2020 and 2021.
The prevalence of polysubstance use, or what Klatzker called the “fourth wave” of the opioid epidemic, comes with an increase in overdose deaths, as well as new challenges in treatment.
Though opioid use disorder on its own can be treated with evidence-based medical interventions such as Suboxone or methadone, there is no pharmacological treatment option for methamphetamine addiction.
Dr. Patricia McKernan, chief of staff at Gaudenzia, said that to treat those addicted to stimulants, the facilities have started using the Matrix Model, a cognitive behavioral therapy tailored toward methamphetamine use, along with holistic mindfulness and wellness initiatives.
Klatzker speculated that the increase in stimulant use could be a function of economics and availability during the pandemic, since meth transport isn’t as reliant on international supply chains that may have been disrupted as fentanyl and heroin are.
“Methamphetamines can be made cheaply and can be made locally, literally in your apartment or your house, so that may have something to do with it,” he said.
To improve these numbers, Klatzker said governments need to treat the addiction epidemic as the public health crisis that it is.
“For far too long, these services have been undervalued, underfunded, and under-resourced, particularly for Medicaid recipients,” he said, noting that population makes up the majority of Gaudenzia’s clients.
Due to financial constraints including low Medicaid rates, Gaudenzia has closed 12 facilities during the pandemic. It continues to struggle with staffing its facilities, despite offering incentives such as signing bonuses and raises.
The report is the first of its kind from Gaudenzia, made possible after a system-level overhaul to electronic medical records. The nonprofit treatment provider plans to release it annually.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.