Philly rolls back smoking ban at inpatient drug treatment centers
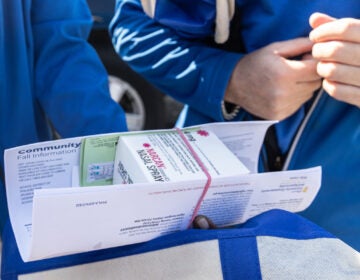
Harm reduction advocates criticized the policy, arguing that banning smoking in treatment would act as yet another obstacle to recovery.

Harm reduction advocates arguedvthat banning smoking in treatment would act as yet another obstacle to recovery. (stasokulov / BigStock)
After nearly three years, Philadelphia’s Department of Behavioral Health and Intellectual disAbility Services has quietly ended its controversial smoking ban at drug treatment centers.
DBHIdS announced the policy would go into effect in January 2019 at the city’s 80 inpatient facilities that receive funding through Community Behavioral Health, the city’s Medicaid pass-through agency. It was to be enforced as a contract mandate, meaning the funding was contingent on providers implementing the ban.
Harm reduction advocates criticized the policy, arguing that prohibiting smoking in treatment would act as yet another obstacle deterring people from seeking out or staying in recovery.
But DBHIdS defended the policy as evidence-based, citing research that shows recovery from drug addiction is more successful when patients also quit smoking.
“Our addictive behaviors don’t just center around one thing — we need to begin to stop with this hierarchy of drugs, so to speak,” said the department’s deputy commissioner, Roland Lamb, in a 2019 interview with WHYY News. “If you’re telling me that you don’t want to stop smoking, you’re telling me that you’re willing to jeopardize any success that we have at treatment.”
Now, the department is changing its tune.
“The idea is to be welcoming, to engage people where they are in their recovery journey, ensure that it’s all non-punitive approaches,” DBHIdS Commissioner Dr. Jill Bowen, who was appointed head of the billion-dollar agency in December 2020, said in an interview this week. “Nobody is turned away.”
As she sees it, Bowen said, the focus of the initiative is about changing attitudes among behavioral health providers so that tobacco dependency is included in addiction treatment, which it has not historically been. She said she simply wants to ensure that everyone has equal access to resources to help them quit smoking.
“I don’t think it was ever intended to be a ban,” said Bowen.
But that’s exactly what it was intended to be, according to the initial press release announcing the policy.
The trajectory from an abstinence-only approach toward smoking in treatment centers to Bowen’s new framework has been a contentious one.
There is substantial research indicating that people have better chances of long-term recovery from addiction if they quit smoking early on in the process. Smokers are greatly overrepresented among people with substance use disorder, and tobacco kills far more people in Philadelphia than overdoses do. All that undergirded Philadelphia’s policy.
Still, the ban was met with immediate pushback from members of the harm reduction community, who countered that a year after more than 1,100 people in Philadelphia had died of overdoses was not the time to tell individuals they weren’t allowed to access treatment unless they were willing to quit smoking. That rate has only gone up since.
“If someone says, ‘Look, I want to stop shooting dope, but I’m not ready to quit smoking cigarettes and I’m not going to go to treatment if you force me to do that, then they should have options available,” said Brooke Feldman, a social worker who led the charge against the policy.
Research also shows that people with substance use disorder are particularly vulnerable to overdoses right after they leave treatment.
After a series of protests and news articles in spring 2019, the department sent a memo to treatment centers, instructing them not to kick people out for smoking. But that only led to more confusion, according to providers, who felt they were caught between a rock and a hard place: They were still supposed to implement the policy, or risk losing critical city funding. But they weren’t supposed to kick people out, either.
A WHYY report from 2019 found that as a result, providers turned a blind eye to people smoking, rendering the policy, at least at some facilities, a ban in name only. Because the policy banned smoking outside, clients in inpatient rehab centers often ended up smoking indoors in hidden places, creating dangerous situations and filling hallways with secondhand smoke. A black market for cigarettes thrived, fueling the very “addictive behaviors” the department officials claimed they wanted to avoid.
Still, DBHIdS defended the policy, citing figures that showed the number of admissions to inpatient treatment centers had not substantially decreased since the ban went into effect, as critics feared they would. They also provided figures showing more people had not left treatment early due to the ban.
But emerging research shows the ban affected people’s decision to seek out or stay in treatment. A recent exploratory survey conducted by Casey Bohrman, an assistant professor of social work at West Chester University, in partnership with the outreach group Angels in Motion examined the impact of the policy on people who currently both use drugs and smoke cigarettes. More than half the participants identified as unhoused.
Of the 112 respondents, just over half said they had left treatment early, against medical advice. Among that group, 85% said the smoking policy was part of the reason they left. Of those considering going to treatment in the coming months, more than half said the smoking policy might or would influence their decision to go into treatment in the next three months.
“This group represents a particularly vulnerable portion of people with substance use disorder,” said Bohrman. “The fact that for the people in our sample, this policy seemed to be such a deterrent and really seemed to influence whether they were staying in treatment is of particular concern.”
The survey also confirmed inconsistencies in the ban’s application. Of respondents who had been to treatment since 2019, 37% said they were able to smoke while there. While most said they were offered smoking cessation tools like a patch or nicotine gum, nearly half said they experienced delays in getting them.
Bohrman presented her research to Bowen of DBHIdS earlier this fall. Bowen was also concerned about the perception of the policy as a deterrent to those considering treatment.
“So it’s one thing whether providers are actually turning people away actively or not. The other is, are people understanding this policy in a way that they don’t even come and request access?” said Bowen. “If you think that it’s not going to be welcoming, or that’s what you hear from perhaps other people, that in and of itself becomes a barrier.”
Bowen said the policy is now more focused on equitable access to tobacco-quitting resources and changing attitudes among behavioral health providers. DBHIdS reported 280 hours of on-site training and technical assistance in 2018 and 2019 at 25 residential drug and alcohol providers.
When asked whether Community Behavioral Health funding for treatment centers would still be contingent on compliance with the policy in its new form, Bowen said her agency will be working with providers to figure out the next steps and the best way to implement the policy that meets their conceptual framework, focused on long-term, whole-person recovery.
A spokesperson for CBH added that it has not utilized any financial penalties as a method of enforcement since the origination of the tobacco recovery wellness initiative.

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.