Pa.’s failure to mandate quicker death reporting before the coronavirus fueled wild data fluctuations, mistrust
Pa. health officials abandoned their urgency in implementing a faster process, leaving them ill-prepared to accurately report death data when the pandemic arrived.
(Dan Nott for Spotlight PA)
For years, Pennsylvania has had a hard time counting its dead.
A new analysis shows that in 2017, Pennsylvania had the most severe death reporting lags in the country. Almost every state was able to send the vast majority of death certificates to federal health officials within three months, but Pennsylvania was able to manage only two-thirds of the work — earning the dubious distinction of slowest in the country.
Unlike many other states, Pennsylvania was still doing much of its death registration by hand, relying on a cumbersome system of faxed paper and manual data entry. It was a process identified by the federal government as “dire and in need of immediate support.”
Death reporting delays can have serious consequences. For example, they can hinder the ability to get protective equipment to communities in need of help. The sooner health officials can analyze death certificates and identify trends, the sooner they can take action and respond to deadly outbreaks of disease — a necessity made all too clear by the COVID-19 pandemic.
Four years ago, Pennsylvania launched its solution: an Electronic Death Registration System that would allow funeral directors, physicians, coroners, and more to quickly and directly submit death data, vastly improving the time it would take to respond to an outbreak.
But an investigation by Spotlight PA and WHYY News found that state health officials abandoned their urgency in implementing the new technology. When the coronavirus arrived and data would become central to saving lives, the system was still largely voluntary, with thousands of funeral homes, hospitals, and coroners’ offices unprepared to use it.
It wasn’t until March 2020 that state officials abruptly mandated use of the electronic system for the reporting of COVID-19 deaths, leading to confusion, delays, and crossed wires at a time when public officials were relying on fast data to inform their pandemic response.
As a result, the state’s official death count unexpectedly fluctuated during the pandemic’s deadliest months, fueling conspiracy theories and undermining public trust in the numbers. Even now, six months into the crisis, the state is continuing to add months-old deaths to its official tally, skewing a real-time view of the virus.
Across Pennsylvania, in big cities and small towns, the death reporting process is largely the same. Funeral directors work with cause-of-death certifiers — the coroner, medical examiner, or physicians at hospitals or nursing homes — to start the death certificate process. From there, in most cases, a local registrar appointed by the state health department will get involved, gathering and logging information from the funeral home and funneling it up to the state.
Dan Weinberger, an associate professor at the Yale School of Public Health, said death statistics submitted by Pennsylvania officials to the Centers for Disease Control and Prevention for January through April of this year were national outliers –– showing such steep declines in deaths amid flu season and a pandemic that the data strained credulity.
“There are no other states in which we see declines quite this dramatic,” he said. “When it’s that obvious and abrupt, it’s usually an indication that the data hadn’t been fully reported.”
The Pennsylvania Department of Health blamed the prolonged rollout on a small number of coroners who refused to be trained on the electronic system, and on others who did not voluntarily use the technology, like funeral directors and hospital personnel. Unlike in other states, coroners do not report directly to the health department, said Nate Wardle, a spokesperson for the agency.
Spotlight PA and WHYY News repeatedly asked to interview Audrey Marrocco, director of the state’s Bureau of Health Statistics and Registries, which oversees death reporting. The department denied those requests, but eventually arranged an interview with Executive Deputy Secretary Sarah Boateng.
In June, Boateng acknowledged that the initial rollout of the system had not gone as planned.
“What we saw, obviously, is that by four years later, not everyone had taken the steps to start using that electronic system,” Boateng said.
Yet she could not fully explain why the state hadn’t ordered mandatory electronic reporting any earlier.
“We did not have a global pandemic prior to now,” she said.
In a statement, the health department focused on the “significant improvements” it has made over the years, both to death registration and to the process of issuing death certificates. But it was the pandemic that exposed the system’s largest weaknesses, jolting changes into place.
Delayed rollout, wasted time
The Electronic Death Registration System — or EDRS — is not new, and it’s not unique to Pennsylvania.
The switch was part of a national effort, dating to the early 2000s, to create a new gold standard for death reporting. About 20 states were using their first iterations of the tool by 2006, according to the CDC. Neighboring states like New Jersey and New York said they finished the switch to electronic systems in 2013 and 2019, respectively.
Electronic death reporting is critical, as it helps officials to more quickly identify and assess a deadly crisis. Fast, accurate data can help inform decisions about where to send supplies and how to allocate resources. Having a modernized system that produces timely death information can “improve outbreak and disaster response efforts,” a CDC website says.
“It’s a whole lot easier to detect people who are dead than people who are sick,” said Robert Anderson, chief of the Mortality Statistics Branch at the CDC’s National Center for Health Statistics. “The earlier we can get information on mortality, the quicker we can develop interventions.”
Pennsylvania’s plan was to implement EDRS gradually, much like other states had done. The system was officially launched in October 2016, said Wardle, the spokesperson for the health department, and the rollout was set to occur in phases due to the “complexity of implementing an EDRS.”
Pennsylvania’s goal was to have “all end users trained to register deaths electronically … by the spring of 2017,” according to an early document.
At the time, there were few states in as dire need of an overhaul as Pennsylvania.
New data from the CDC shows that in 2017, the vast majority of U.S. states were able to send information about nearly all deaths to federal health officials within 13 weeks of the date deaths occurred. Pennsylvania, however, lagged far behind, able to manage only 65% of the work in that same time period. Connecticut was the next slowest state, at 68%, followed by Arizona (85%) and West Virginia (87%).
But by the end of 2017, and despite a quarter of a million dollars spent just on the first phase of the rollout, the state still had not trained everyone on the technology — let alone all 67 county coroner or medical examiner offices.
At the time, 13 county coroner offices refused to participate in the training, Wardle said. A document previously available on the health department’s website showed the following 13 offices were not trained on EDRS as of December 2017: Armstrong, Bedford, Berks, Blair, Delaware, Franklin, Huntingdon, Lebanon, Mifflin, Montour, Somerset, Venango, and Warren.
“In 2017, due to concerns expressed by some stakeholders, including those coroners’ offices that refused to attend training and others that refused to voluntarily adopt EDRS prior to the pandemic, the department decided to roll out EDRS over a few year period so that stakeholders were able to make necessary internal business workflow modifications to support electronic reporting,” Wardle said.
Charles Kiessling Jr., coroner in Lycoming County and president of the Pennsylvania Coroners Association, said part of the issue was that about 25 coroners’ offices in the state had already been using a different electronic system called Quincy. Kiessling said that for years, he had asked the health department to build a bridge between Quincy and EDRS, so coroners didn’t have to input the same information twice.
According to Quincy’s documentation, it shouldn’t have been difficult to implement a bridge connecting the two electronic systems, as Quincy was designed specifically to be able to hook into EDRS applications. “Duplicative keystrokes are costly and error-prone,” the technology’s website says. “We do everything we can to avoid ‘double data entry.’”
“Hopefully the bridges will be completed in the future,” said Kiessling, “but this system has been being developed for many years and is still not complete.”
He said his office in Lycoming County has one deputy coroner trained on EDRS, “but most of the time we print paper death certificates out of Quincy and deliver to the funeral directors who input the information into the EDRS system.”
Wardle, the spokesperson, acknowledged “there is still work to do,” saying the department has waited five months for several coroners to begin the bridge testing.
‘Deer in the headlights’
The second phase of EDRS training, dedicated to onboarding the tens of thousands of medical professionals legally tasked with completing cause-of-death paperwork, didn’t begin until April 2019.
Ongoing delays were apparent at the beginning of 2020.
Kiessling said he met with a group of Pennsylvania physicians in late February 2020, at the request of a UPMC hospital in Williamsport. At that time, the coronavirus was already international news. Wuhan, China, had been ravaged by the pandemic, and the U.S. had documented its first confirmed case the month prior.
Kiessling said he traveled with Audrey Marrocco, director of the state’s Bureau of Health Statistics and Registries office, to discuss issues with death certificates. According to Kiessling, the physicians looked like “deer in the headlights” when it came to the electronic system.
They didn’t know what EDRS was, he said. But they would soon find out.
On March 6, just 12 days before Pennsylvania’s first recorded COVID-19 death, the state health department issued a mandate: All deaths attributed to COVID-19 would have to be reported through EDRS.
Two weeks later, the department went further. Beginning March 20, all funeral homes in the state would need to use the system to report all deaths, COVID-19 or not.
Funeral homes without computers or internet service could apply for EDRS waivers, allowing them to continue with paper, the department said. But for everyone else, protocol had shifted. The state was demanding tens of thousands of funeral directors, coroners, and physicians at hospitals and nursing homes to adjust their workflows effectively overnight.
Many weren’t prepared. Some even started flagging concerns with the health department.
Through a public-records request, Spotlight PA and WHYY News obtained copies of nearly 60 EDRS waiver applications submitted to the department.

“How can we do mandatory EDRS reporting when proper training has not been provided,” one funeral director wrote in a waiver application dated March 19.
“Physicians are not yet set up for this,” warned another on March 20.
“We are EDRS capable,” wrote a third funeral director on March 23. “But most of the hospitals, doctors, and nursing facilities are NOT able to respond in kind.”
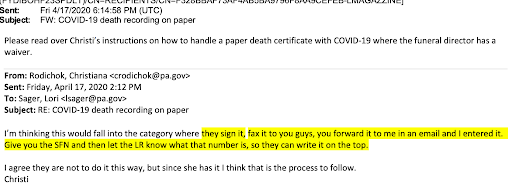
According to data obtained through a public-records request, more than 7,550 medical professionals, support staff, and administrators rushed to sign up for EDRS between March and April, compared to only about 350 new users who signed up in January and February.
“The problem was, they implemented this in the middle of a pandemic,” said Kiessling.
Though Kiessling credited the state for pushing out a flood of digital training materials and webinars, he questioned the health department’s assumption that front-line physicians would even have time to participate.
“Doctors don’t have time to sit in the ICU and watch these videos,” he said. “People are dying.”
Death toll fluctuates
For the first two months of the crisis — the deadliest two months in Pennsylvania’s COVID-19 history — the state didn’t draw from EDRS to produce its public death count.
Instead, death data was being reported out of a different system, PA-NEDSS, and pulled from EDRS with the help of algorithms, Wardle, the spokesperson, said in April.
But without a fully functional electronic death system in place, the state found itself playing catch-up — adding weeks-old deaths to its count and causing the death toll to spike several times in April and May.
Health Secretary Rachel Levine often cited difficulties “reconciling” data from different sources, as she reported hundreds of deaths that had occurred in weeks prior.
In the spring, the state’s numbers for Philadelphia also consistently lagged behind the city’s own count, by hundreds of fatalities. Questioned by reporters in April, officials blamed the discrepancy on a vague computer update, but deaths jumped the next week as the state reconciled its numbers with the city.
That month, as neighboring states were showing enormous total death increases compared to the same period in 2019, health department officials said they were unable to provide an exact count of how many people had died — from any cause — in Pennsylvania in March.
The reason: 2,000 uncounted paper death certificates that continued to stream into the office.
Since mandating the use of EDRS, the state has seen improvement on that front. In January and February, about 30% of the state’s deaths were reported fully on paper. By April and May, that number had dropped to 2%.
And officially, the Wolf administration regards the rollout of its Electronic Death Registration System as a success story.
“The department has been focused on continuous quality improvement,” said Wardle, the spokesperson. The agency has made “significant improvements,” he said, adding that by early summer, the state was able to issue death certificates within two to three weeks. Wardle blamed additional reporting lags on delays in COVID-19 test results, citing the need for a medical certifier to amend a death record when a pending test comes back positive.
Yet data obtained by the news organizations show the state is still a long way from full adoption.
Unlike some other states, Pennsylvania doesn’t allow death certificates to be obtained under the state’s public records law. In order to understand how often EDRS was used in the first half of 2020, Spotlight PA and WHYY News submitted a Right-to-Know request for the forms funeral homes must file to apply for death certificates. A small box on that form lists two options for a filing method: one for EDRS and another for paper.
In April and May, more than 60% of death information was reported partially on paper in what the state calls a “hybrid” EDRS process. Doctors from hospitals or nursing homes continued to avoid using the electronic system to fill out their portions of death certificates, instead faxing the details directly to the state. This left funeral directors in a lurch, waiting for the state to sync the records and handle the manual data entry of the medical information before the death record could be fully processed.
Nearly half of all 12,500 inquiries sent to the state’s EDRS support helpline during the first half of 2020 were from funeral directors requesting “status updates on data entry,” an attorney for the state health department said in response to a public-records request from Spotlight PA and WHYY News.
In June, Wardle said information faxed by medical professionals is entered into EDRS by department staff within two to three days, “which enables rapid reporting of the deaths.”
But a notice published by the health department on July 1 acknowledged ongoing reporting lags, imploring those who report deaths to use EDRS to reduce “the three-month delay associated with paper reported deaths.”
Pennsylvania’s Electronic Death Registration System is part of a national effort to improve the timeliness of death reporting. Fast access to death data can help officials to assess patterns and identify potential crises. According to the CDC, it should take about two to three years for a state of Pennsylvania’s size to fully roll out an EDRS. Currently, the state’s EDRS is in its fourth year of use.
Geneva Goldstein, of the Goldsteins’ Rosenberg’s Raphael-Sacks Inc. funeral home in Philadelphia, said she followed the state’s instruction to switch to EDRS, but doctors kept faxing her the medical portion of death certificates anyway. So, she completed her portion online and faxed the rest to the state.
“This whole online system that we use is still in its infancy,” said Goldstein. “It’s working in a sense, but it’s not fully operating.”
With EDRS rollouts, states must be prepared to manage what’s often a difficult transition away from paper, said Anderson, of the CDC.
During a state’s first year of working with an electronic system, Anderson said, “the timeliness of the data gets a lot worse.” It’s only later, once the kinks of the new system are worked out, that death reporting gets speedier.
“I fully expect that Pennsylvania’s system, as it matures, is going to be good,” he said. “But until then, it’s sort of like trying to herd cats.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)



