Nurses at St. Mary Medical Center strike for safer staff levels as coronavirus surges
As the virus hospitalizes more people across the region, the 700-plus nurses say there aren’t enough of them on staff to keep patients safe.

Nurses picket at the entrance to St. Mary Medical Center in Langhorne, Pa. About 800 nurses went on strike Tuesday citing long simmering grievances over wages and staffing levels. (Emma Lee/WHYY)
Ask us about COVID-19: What questions do you have about the current surge?
A little over a year ago, Debbi Bozeman left her station on the medical surgical unit at St. Mary Medical Center in Bucks County and began going floor to floor with a simple message: It’s time to start a union.
It wasn’t a tough sell, she said. The Langhorne hospital’s owner had been cutting staff and on-call pay across departments for years. Pretty much everyone agreed that if they were going to keep patients safe, there simply must be more nurses.
After months of pushing for staffing guarantees in their first contract with hospital owner Trinity Health, more than 700 nurses at St. Mary walked off the job Tuesday for a two-day strike.
Negotiations between the nurses, represented by the Pennsylvania Association of Skilled Nurses and Allied Professionals (PASNAP), and Livonia, Michigan-based Trinity Health have been taking place for more than a year. Nurses want enough staff on each unit to allow them to focus on caring for patients at their bedsides, without being pulled off to transport them, admit new patients, or collect supplies from faraway storage areas.
“There’s just not enough of us to go around,” said Bozeman. “You always feel like you’re falling a little short.”
In Bozeman’s med/surg unit, she said, there is one nurse for every 11 patients. Her team determined that staffing there should be doubled.
The need for safe staffing is especially dire as COVID-19 cases surge and hospitals prepare for an influx of patients.
“There are clearly much better strategies for treating patients with COVID now than there were at the beginning of the pandemic, but they are strategies that require a lot of staff,” said Rebecca Givans, a labor studies expert at Rutgers University who specializes in health care settings.

She pointed to “proning,” the practice of turning often-intubated patients on their stomachs to relieve the pressure on their lungs, which has proved to save lives but often requires up to a half-dozen nurses and aides to perform.
“Having a shortage of staff means that every COVID patient cannot have that level of care and people may die because of that,” Givans said.
Joe Gentile, who has worked at St. Mary for 36 years, said that scenario is not a hypothetical: It’s a reality he and his colleagues already lived through once.
“A person can’t breathe and they’re in a quarantined room,” he said, describing a severely ill COVID-19 patient. “They’re too weak to reach the call button. If I had four patients and now I have seven, I can’t get to them, and someone can and will get hurt. This isn’t conjecture, I’m not exaggerating, we’ve lived it. Some of us have a little PTSD from it.”
It’s been widely acknowledged that keeping hospitals below their maximum capacity improves the death rate from COVID-19 — that’s part of why the disease is not as fatal now as it was during the pandemic’s spring peak in places like Pennsylvania.
Hospital owner Trinity Health frames the nurses, who claim their priority is the safety of their patients, as hypocritical for walking off the job just as COVID cases were surging. Bozeman said that could have been avoided long ago, since Trinity had several weeks’ notice that the nurses were preparing to strike.

To keep the hospital open, Trinity hired replacement nurses, which it said were “fully oriented to [the] hospital’s processes and policies.” Research indicates that nurses hired through a staffing agency are less likely to offer high-quality care.
Trinity will keep the contract nurses through Sunday, even though the PASNAP-affiliated staff planned to return Thursday. Trinity said the extra days are to accommodate transition time for the staff, but Givans said it’s a common tactic to both take advantage of staffing agencies’ minimum contract lengths and spite their own staff for striking.
“It’s a bit of a cruel tit-for-tat game,” she said.

Trinity Health bought the hospital in 2018. In 2019, St. Mary was the most profitable acute-care hospital in Southeastern Pennsylvania, according to a report from the Pennsylvania Health Care Cost Containment Council, netting $390 million and posting a 13% increase in profit margin over the three prior years. The medical center is the second-largest private employer in Bucks County, and the fourth largest overall.
Nurses involved in the negotiations said that before they took a break for the pandemic, they felt they were making progress in bargaining with Trinity’s representatives. After the pause, the hospital owner swapped out lead negotiators. The new attorney, a lawyer from the Stevens and Lee law firm in Philadelphia, was less open to compromise, said the nurses.
Bozeman said not being able to communicate with hospital leadership who actually work on site makes it hard to see eye to eye.
“Sometimes, you just have to get the parties together and you need to talk it out,” she said. “If we could sit down at the table and they could say, ‘Well, I can see how you need this, but we can’t work with this — let’s find a compromise.’ We’re not even getting that.”
Bringing in outside counsel may be a tactic designed to stall progress and prevent a first contract from ever being reached, said Givans.
“They have to maintain a plausible case that they bargained in good faith, otherwise they’ll be breaking labor law, but if they can show that they’re bargaining in good faith but yet the contract can’t be achieved, they might be able to never achieve a first contract, which might serve their goals,” Givans said.
In a statement, Trinity said it remained “committed to negotiating in good faith to reach agreement on a fair, consistent and sustainable initial contract for St. Mary nurses.”
The nurses point to the recently finalized first contract at St. Mary’s sister hospital, Mercy Fitzgerald in Delaware County, as a demonstration of the type of wages and staffing they’d like to secure. The nurses there are also represented by PASNAP.
St. Mary officials said staffs at the two hospitals are being drawn from different markets, therefore eliciting different contract terms.
“Mercy Fitzgerald competes for nurses with large academic medical centers in downtown Philadelphia, and their nurses’ wages reflect that competitive reality,” wrote Christy McCabe, a spokesperson for Trinity Health. “In Bucks County, wages for St. Mary nurses are in line with other suburban hospitals’ pay. St. Mary has made generous offers on wages, which the union has rejected.”
While the nurses maintain their priority is safe staffing, not wage increases, they note the two are related, as competitive wages lead to better staff retention.
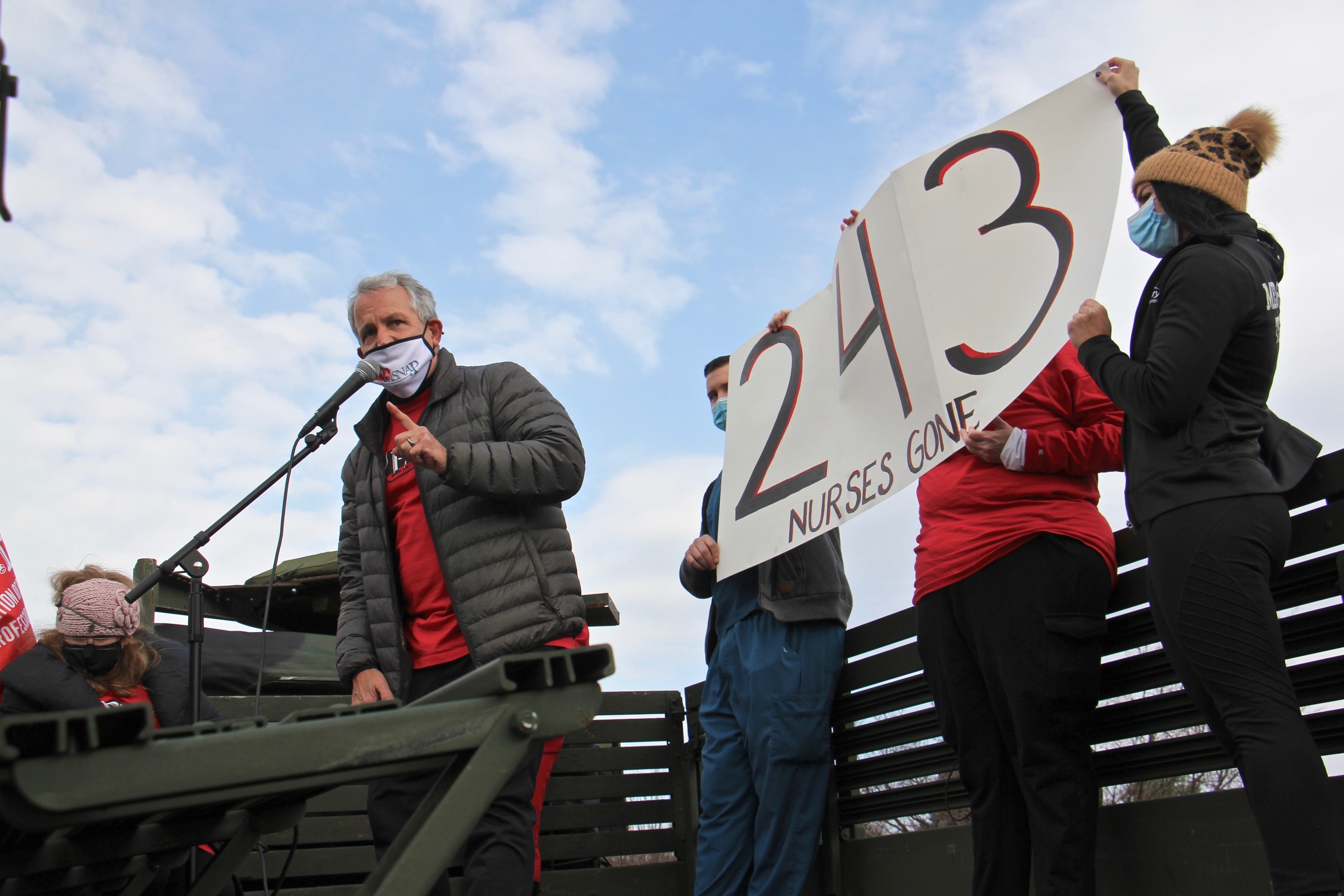
Jill Gross works in the progressive care unit and has been at St. Mary for eight years. She said she watched as the hospital hemorrhaged nurses, losing more than 200 over the last two years, with more than 20 people leaving one unit alone. Many of her former colleagues, she said, were afraid of losing their nursing licenses because they were stretched so thin that they were more likely to make a mistake or be forced to do shoddy work under pressure. She didn’t want to be counted among them.
“I grew up here, I feel an attachment to the hospital that I feel is gone,” said Gross, noting it was becoming an increasingly difficult place to work. “I live here. Think of what we do together every day at work. We’re family.”

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)