N.J. and Delaware working to sequence more coronavirus samples to track variants
The U.S. is still far behind other countries when it comes to doing enough of the lab work needed to keep track of the variants of SARS-CoV-2.

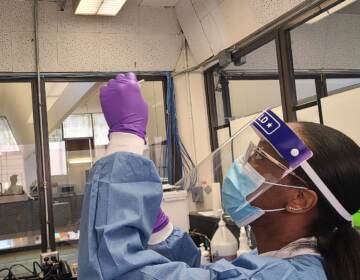
In this photo taken on Friday Dec. 25, 2020, Virologist Sunday Omilabu in a lab, during an interview with The Associated Press in Lagos, Nigeria. (AP Photo/Lekan Oyekanmi)
Ask us about COVID-19: What questions do you have about the current surge?
Public health laboratories in New Jersey and Delaware are working to do more investigations of the genetic data of coronavirus samples, to identify new variants sooner and see how the virus is spreading.
There’s a national need for this work, also known as genomic sequencing. It involves looking at all the genetic data of a coronavirus sample to see how it compares to other samples.
Only a tiny percentage of positive COVID-19 cases in the United States have been sequenced so far, according to data from the Centers for Disease Control and Prevention. In the vast majority of states, including Pennsylvania, Delaware, and New Jersey, less than 1% of all positive COVID-19 cases have been sequenced. All three states have reported cases of COVID-19 linked to the B1.1.7 variant of the virus. Scientists at a commercial sequencing company estimated that the U.S. needs to sequence around 5% of all positive COVID-19 cases to find variants of the coronavirus early on and at the same time not spend too much time just on sequencing.
A Washington Post analysis from December 2020 ranked the U.S. 43rd when it comes to the percentage of cases that have been sequenced, far behind countries such as Australia, New Zealand, Vietnam, and the United Kingdom.
Diane Griffin, a microbiology and immunology professor at Johns Hopkins University, said that new leadership at the CDC understands how important it is for the U.S. to do more sequencing, but that at the same time “it’s still embarrassing that we don’t do it better.”
She added that the U.S. has done a lot of sequencing in cities with large health departments or academic medical centers that already have the staff and equipment to do that work, but she worries that there may be other places around the country, like rural regions, that don’t have easy access to such resources.
Griffin co-authored a report from the National Academy of Sciences last year detailing what the U.S. needs to do to collect more genomic data about the coronavirus. One of the other co-authors, Julie Segre, a geneticist at the National Human Genome Research Institute, said the U.S. also needs to be able to link patient data to genome data, so public health officials can quickly figure out whether someone infected by a variant of the coronavirus had traveled outside the U.S., had particular health conditions, or had been vaccinated against the virus. Segre said countries like the U.K. had linked their national health systems to their sequencing infrastructure, which made case investigations much easier.
Ideally, she said, researchers would be able to sequence samples of the virus where they are being collected and processed already. That’s the case at the Delaware Public Health Laboratory, where the staff tests for the coronavirus and sequences some of those samples from positive tests. The goal is to sequence all the samples that come in, said Rebecca Savage, microbiology and sequencing lab manager.
Savage said the Delaware Public Health Laboratory had started sequencing samples in September and is now able to sequence around 60 samples a week, as well as sending others to the CDC. The goal is to more than double that by training additional microbiologists and using a machine to automate some of the more time- and labor-intensive steps that the staff currently does by hand.
The CDC has set a national goal of sequencing 7,000 samples a week. Aside from public health departments, a consortium of universities and commercial, government, and nonprofit labs around the country are doing some of this work as well.
The New Jersey Department of Health also is ramping up the sequencing capacity in its lab, which stands at 160 samples a week right now, said Edward Lifshitz, medical director for the department’s Communicable Disease Service. He said New Jersey needs to add equipment and train staff.
“It never happens as fast as in a perfect world,” Lifshitz said. “This is not a simple test; worse than not being able to do the test is doing the test and getting the wrong answers.”
Pennsylvania’s Department of Health is not sequencing samples of the coronavirus, nor does it partner with any other labs to do the work in the state, said Wendy Braund, COVID-19 response director for Pennsylvania.
Instead, Pennsylvania sends up to 35 samples of the coronavirus to the CDC to be sequenced every two weeks, with no change from the start of the year.
Investing in genomic sequencing will pay off even after the current pandemic, the scientists interviewed for this article said. Delaware started doing sequences back in 2015 to investigate other outbreaks, such as foodborne diseases.
Julie Segre, at the National Human Genome Research Institute, said there had already been a push for public health labs to do more genetic sequencing in the past few years.
“They also use the same technology if they want to understand if there is a salmonella food outbreak, or if there is an outbreak associated with some sort of soft cheese,” Segre said. “This need to do genomic sequencing in a public health setting is not new to SARS-CoV-2.”

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.




![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)