MIS-C: Doctors make progress on COVID-related illness affecting kids
While doctors say they have more information on how to treat MIS-C, it's still a mystery why some children get it and others don't.
Listen 2:26
Students, wearing face masks and paying attention to social distancing, study at Les Magnolias primary school during the partial lifting of coronavirus, COVID-19, lockdown regulations in Brussels, Monday, May 18, 2020. (AP Photo/Francisco Seco)
Are you on the front lines of the coronavirus? Help us report on the pandemic.
On a sunny day at the end of May, the Lis family decided to take a walk in the park with their dog Rexy.
The dachshund is usually well-behaved and never leaves the family’s side — so the Coatesville family decided to let him off his leash.
But something caught Rexy’s attention, and he took off at dart speed, running across the field.
Fifteen-year-old Andrew, a cross country runner, ran after the dog for about a quarter of a mile until catching him.
A month prior, Andrew was fighting for his life at Nemours/Alfred I. duPont Hospital for Children in Wilmington. So, the chase was a joyful sight for his parents Ed and Ingrid.
“I have to tell you, it caught my breath and I almost started to cry, and I thought, ‘Thank God he’s alive and well,’” Ed said.
After fighting a bout of mysterious symptoms in April, Andrew, who has no underlying medical conditions, was diagnosed with multisystem inflammatory syndrome in children, or MIS-C, which occurs in young people who were likely exposed to or have had COVID-19.
Children’s hospitals in the area say they’ve had fewer cases of MIS-C as incidents of COVID-19 have declined. However, they’re prepared to continue to treat the illness until the coronavirus is eradicated.
Physicians say they’re able to provide more informed treatment now than in the spring when news about MIS-C first came out. However, the mystery remains about why some children get it and others don’t.
MIS-C cases are rarer than COVID-19 cases among children, and COVID-19 occurs less frequently in children than adults. But as schools grapple with the decision to reopen in the fall, some health experts worry about a potential spread of the coronavirus.
The Lis family wants to warn other parents about MIS-C.
“The caution for parents is to not take things lightly,” Ed said. “If your kid is not feeling normal…. have them checked out right away because we might have waited for too long. Thankfully our son didn’t pay the price for that.”
A mystery illness
MIS-C typically occurs after a child has recovered from a COVID-19 infection, when the body’s immune response is ramped up. Many MIS-C patients don’t know they previously had COVID-19 because they were asymptomatic. The patient might not get symptoms for MIS-C until up to eight weeks after having the virus.
Symptoms include high fever, rash, and prominent gastrointestinal problems such as pain and diarrhea. Some children also present with neurological symptoms.
There’s no standardized treatment for MIS-C. However, most patients receive an immune modulator to decrease inflammation.
Doctors can diagnose MIS-C after evaluating symptoms, and conducting a series of laboratory and imaging testing. Patients also undergo an antibody test to determine if they previously had COVID-19.
The treatment often consists of steroids and intravenous immunoglobulin — which is taken from the blood plasma of donors.
Nemours Hospital has diagnosed 15 MIS-C cases, most of which have been among teenagers. The hospital system has also diagnosed 240 pediatric COVID-19 cases across its sites in Delaware, Pennsylvania and New Jersey.
Across the border in Philadelphia, St. Christopher’s Hospital has diagnosed about 15 to 25 cases since May, among patients ages 8 and 12. They also diagnosed about 175 pediatric COVID-19 cases.
Patients at both hospitals are now healthy, officials say.
Hospitalized for Easter
Leading up to Easter, Andrew had a mild headache and some pain in his stomach, before developing a fever. He didn’t have a cough or shortness of breath, so his parents didn’t think he had COVID-19.
At first, Ed and Ingrid Lis decided not to take Andrew to the doctor, because they feared he might catch the coronavirus at the doctor’s office.
But on Easter weekend, Andrew’s fever continued to spike, and he complained of significant pain in his abdomen, and an ache on the back of his head and the side of his neck.
“When I started feeling sick, I thought it’s just one of those days you get a cold or something, so I went to bed early,” he said. “And the next day I still wasn’t feeling good … There were some points I was up and could pay attention, and there were some times the pain was so great I couldn’t do anything.”
Early Easter morning, Andrew checked into Nemours, on the advice of his primary care physician, who thought he could have appendicitis or meningitis.
Physicians at Nemours performed bloodwork and various other tests to determine his illness. At first, they thought Andrew might have a gastrointestinal problem. But Andrew’s symptoms continued to worsen. He developed other issues, including a drop in blood pressure, severe diarrhea and a rash. Physicians tested Andrew for every disease they could think of but continued to be stumped on what was wrong.
“Here we were seeing him get increasingly sicker, and not knowing what was going on and hearing the doctors say, ‘We think it might be this, we think it might be that.’ These are the best doctors in the country for treating kids, and they were continuing to seek out an answer for this,” Ed said.
Doctors then became worried about a cardiac dysfunction and told Ed and Ingrid that Andrew had to be moved to the cardiac ICU and be intubated for the best chance of saving his life.
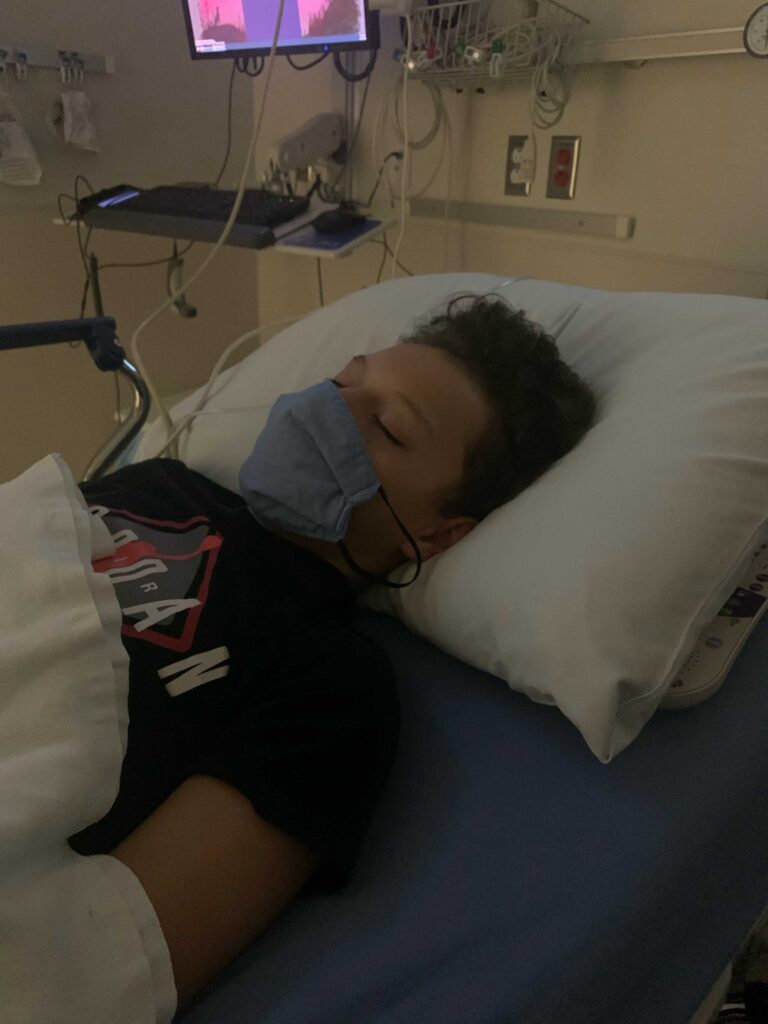
“Nothing prepares you for hearing, ‘We need to do everything we can to save your son’s life.’ It brought my wife and I to our knees,” Ed said. “[But] they were like medical detectives. Even though it was absolutely unsettling not knowing what was going on, what gave us reassurance was these doctors were not going to stop until they could figure out what was wrong. And everything they could do to preserve my son’s life they were going to do.”
Andrew was in the hospital for 10 days before he was able to return home. When research about MIS-C was announced about a week after Andrew’s discharge, the physicians finally had the answers they were looking for.
The whole family was asked to take an antibody test for COVID-19 — Andrew was the only one with positive results.
The family still doesn’t know how Andrew could be the sole member to contract the virus. At the beginning of March, they had taken a trip to Florida together, and after the lockdown started, they all hunkered down at home.
“We’re a large family. We are very close. We’re not scared of showing affection. So, it was strange to find out he was the only one who got sick,” Ingrid said.
Andrew said he is doing well today and was given a clean bill of health by his cardiologist.
The future of MIS-C
Since the first treatment of MIS-C a few months ago, doctors have been able to share information all over the world to educate each other on which treatments are successful, allowing health professionals to prescribe better-informed treatment.
“As we are learning more information, our treatment is becoming more protocolized to direct it toward what other colleagues are having significant success with,” said Dr. Meg Frizzola, chair of pediatrics at Nemours.
While much progress has been made on MIS-C, doctors still don’t know why certain age groups contract MIS-C, or the underlying reasons that cause certain children to contract it.
“I think we don’t know why some children get it versus others, and we don’t know the long-term consequences of this disease,” said Dr. Emily Souder, attending physician of pediatric infectious diseases for St. Christopher’s Hospital. “We think because of the way we’ve seen an increase in COVID cases, and a couple weeks later we see an increase in MIS-C cases, there definitely seems to be a certain time frame. But I think in terms of the underlying mechanisms of why this is happening, we don’t know.”
So far, all of St. Christopher’s and Nemours patients have recovered and are doing well. However, physicians still aren’t sure about long-term impacts.
That weighs heavily on Ingrid Lis, Andrew’s mother.
“Finding closure was good, but it continues to worry us,” she said. “Because as we learn, you can contract the virus and it might not do anything to you, any complications related to that can happen later on.”
“What’s it going to be for him when he gets the flu, or get something else, how is his body going to react?” she added. “How is the virus going to continue showing complications for him? That keeps us on the edge.”
St. Christopher’s has had fewer MIS-C cases recently, which Souder said might be because COVID-19 cases have been overall decreasing in the Philadelphia region. She said if there’s a large increase in COVID-19 cases again, there will likely be a peak in MIS-C cases.
Doctors say it’s impossible to predict when MIS-C will be eradicated.
“Although fortunately in our state the numbers are not continuing to climb, COVID-19 is still in existence and is still prevalent. Many children are asymptomatic from the first infection of COVID-19, and this [MIS-C] is the post inflammatory phase, so we are continued to and prepared to continue to treat this disease,” Frizzola said.
Souder said the lack of information on MIS-C makes health experts wonder how school openings will affect the spread of COVID-19 and related illnesses like MIS-C among children.
“That’s the important question we’re all trying to decide,” Souder said. “What the right thing is to do and whether children will be big transmitters of the virus … If they were back in school, what’s the risk? I don’t think there’s a clear answer at this point.”
Ed and Ingrid encourage their friends and family to social distance and wear masks. The couple say they get frustrated when people suggest kids can’t become seriously ill with the virus.
“There’s as much if not more we don’t know about this disease and its short and long-term effects and its impact on kids, and they need to listen to the health experts and stop beating this drum about, ‘My rights and my needs,’ because this a public health crisis,” Ed said. “Until it comes on your doorstep, it may seem like a distant reality. But it wasn’t for us.”
The couple is also urging other parents to take their kids to the hospital as soon as they become ill.
“We were very concerned about checking into the hospital. I was saying, ‘No, he doesn’t have COVID, I don’t want him to get it if we go to the hospital.’ But I think if we had taken one more day to ride it out, he would not have made it,” Ingrid said. “Doctors and nurses will know what is best for them because there are limited resources at home.”

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.





![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)


