In wake of alarming HIV forecast, Philadelphia intensifies new approach to curb epidemic
Listen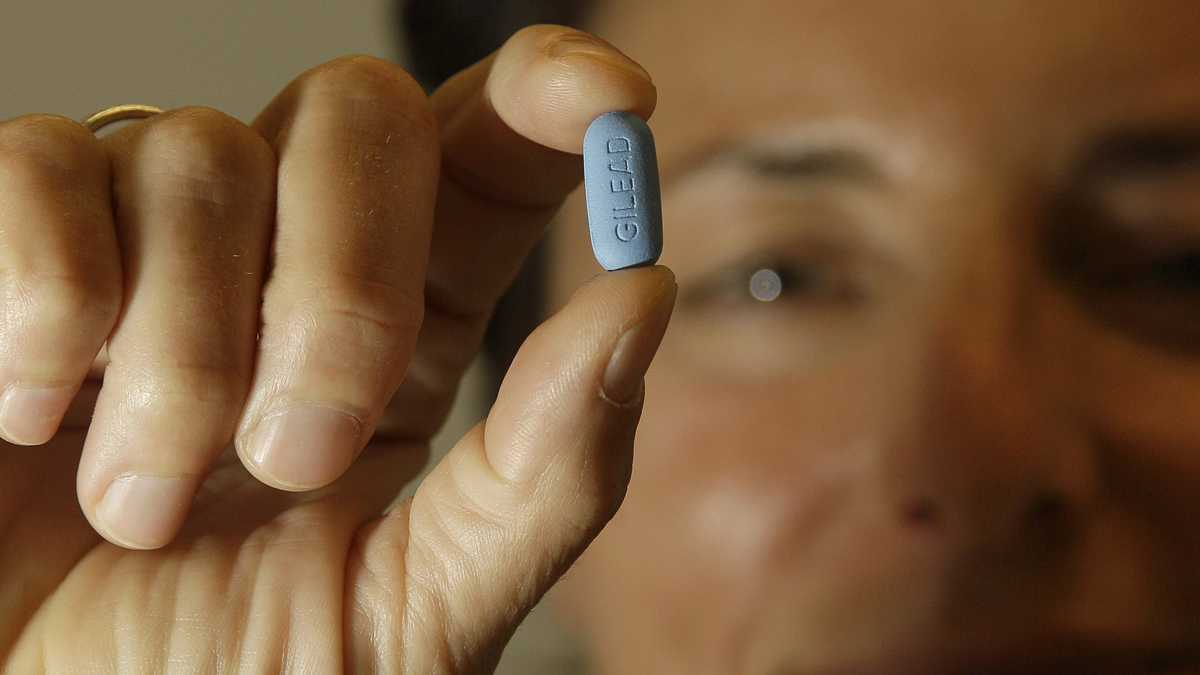
Dr. Lisa Sterman holds up a Truvada pill at her office in San Francisco. The pill, used to treat people with HIV, also helps prevent the virus from infecting healthy people. (Jeff Chiu/AP Photo)
Without context, the numbers can seem demoralizing: In the U.S., half of all black men who have sex with men will contract HIV at some point in their lives.
The Centers for Disease Control and Prevention based the projection on infection rates between 2009 and 2013.
“My reaction was, I was quite shocked,” said D. D’Ontace Keyes, an organizer with Philadelphia Black Pride. “We have been packaged to be victims of this epidemic, but, in addition, there hasn’t been enough investment to celebrate our resilience within that, to celebrate our successes.”
Basic HIV education and awareness are out there, but the strategies and approaches have to change, he said.
“I think there’s a need to bring more people to the table having this conversation and also mobilizing for something new,” said Keyes.

Dr. Kathleen Brady, medical director with Philadelphia’s AIDS activities coordinating office, agreed. She views those CDC projections as a worst-case scenario, as a call to action.
“We’ve been using condoms for the last 30 years, but we haven’t seen any major changes in the epidemic,” said Brady. “We need to do something different.”
Nearly 19,500 Philadelphians are living with HIV/AIDS, according to 2014 data. It’s estimated that about 3,804 black gay men in Philly have HIV, compared with 2,083 white gay men.
Meanwhile, for Latino gay and bisexual men, the recent CDC estimates one in four will have HIV at some point. Compare that to one in 11 for gay and bisexual white men and one in 2,514 for heterosexual white men.
The reasons behind the higher infection rates are complex and involve socioeconomic factors, Brady said. But it’s not about differences in behavior.
“Part of the problem ends up being, once there is a higher prevalence in a community, your potential sex partners typically come from that community,” said Brady. “So the risk of being exposed to HIV is definitely going to be higher.”
‘We have something different’
A powerful prevention tool now exists that could dramatically change the course of the epidemic: pre-exposure prophylaxis therapy, also known as PrEP.
It’s a pill that, if taken regularly, prevents a person from getting HIV. PrEP, in combination with better treating people who have HIV and better diagnosing people, could dramatically alter the course of the epidemic, Brady said.
Problem is?
“It’s being underutilized,” she said.
Prep was approved in 2012, but it’s still relatively new. A 2014 health department survey of about 500 HIV-negative gay men found that about 6 percent were on PrEP. The number was 4 percent for black gay men. After a brief description of PrEP to interviewees, about two-thirds said they were willing to take it.
In response, the city recently hired a PrEP coordinator, mainly to educate doctors. It developed an official city PrEP plan; it increased the health centers, including its STD clinic, that now offer PrEP; and it created a help line (215-685-2437). The city health department was recently awarded millions in federal dollars to step up outreach efforts, specifically among black and Latino gay men.
All that sounds great in theory, said Keyes, adding that it will only work if those efforts are really led by the community and stem from within the community.
“Those type of conversations happen in the most informal ways. Not in systems, not in institutionalized spaces, not necessarily in clubs,” Keyes said. “They happen in homes, on the phone, they happen online in chat groups. And I think that is something that has not been tapped into appropriately.”
Taking control of one’s health
For 22-year-old Ramee Garnett, the decision to take PrEP happened last year. He first learned about it from a friend in Atlanta.
“And I was like, do they have it in Philly?”
He Googled information about it, and then found a clinic that helped him sign up for insurance, which then covered it.
“Nobody’s worrying about my health besides me, so I put my life in my own hands and decided to get on it,” said Garnett. “I’m the one that’s taking control of my own life.”
Garnett said there’s still a learning curve. He recalls an incident when he had company over who saw the medication and then abruptly left, assuming Garnett had lied about his status, that the medication was to treat HIV as opposed to preventing him from getting it. (The medicine — brand name Truvada — is also used as a combination therapy to treat HIV.)
“They started going off on me, and I was like, ‘Look it up!'”
That just got Garnett talking even more about it with close friends. He doesn’t want those HIV projections to reflect the reality for him and others. And he says, now, it doesn’t have to.
“It’s just one extra step.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.

