Community health clinics are positioned to vaccinate the most vulnerable. Do they have what they need to do it?
Federally qualified health centers are well positioned to vaccinate underserved communities. But they must balance that need with serving regular patients.
Listen 2:17
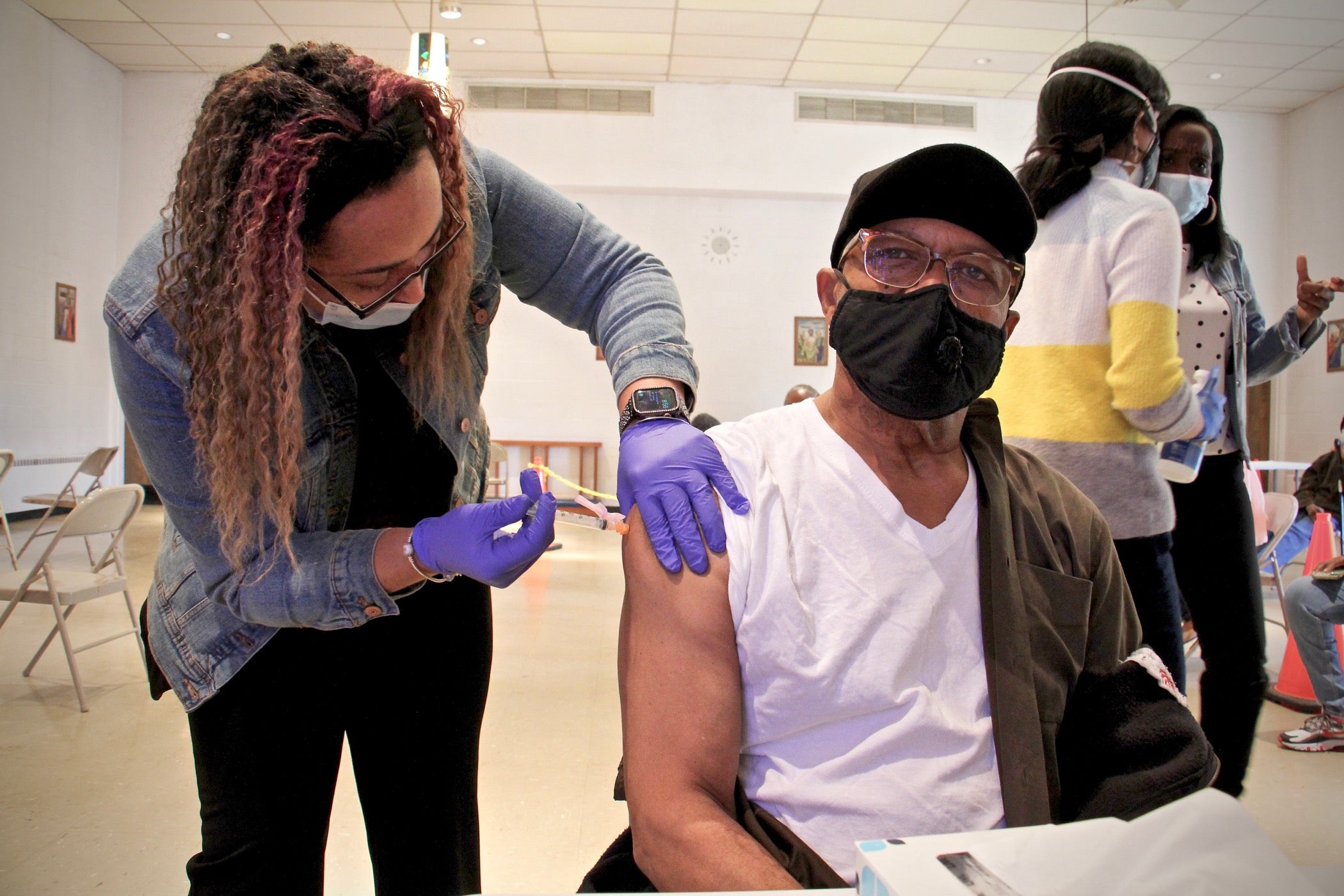
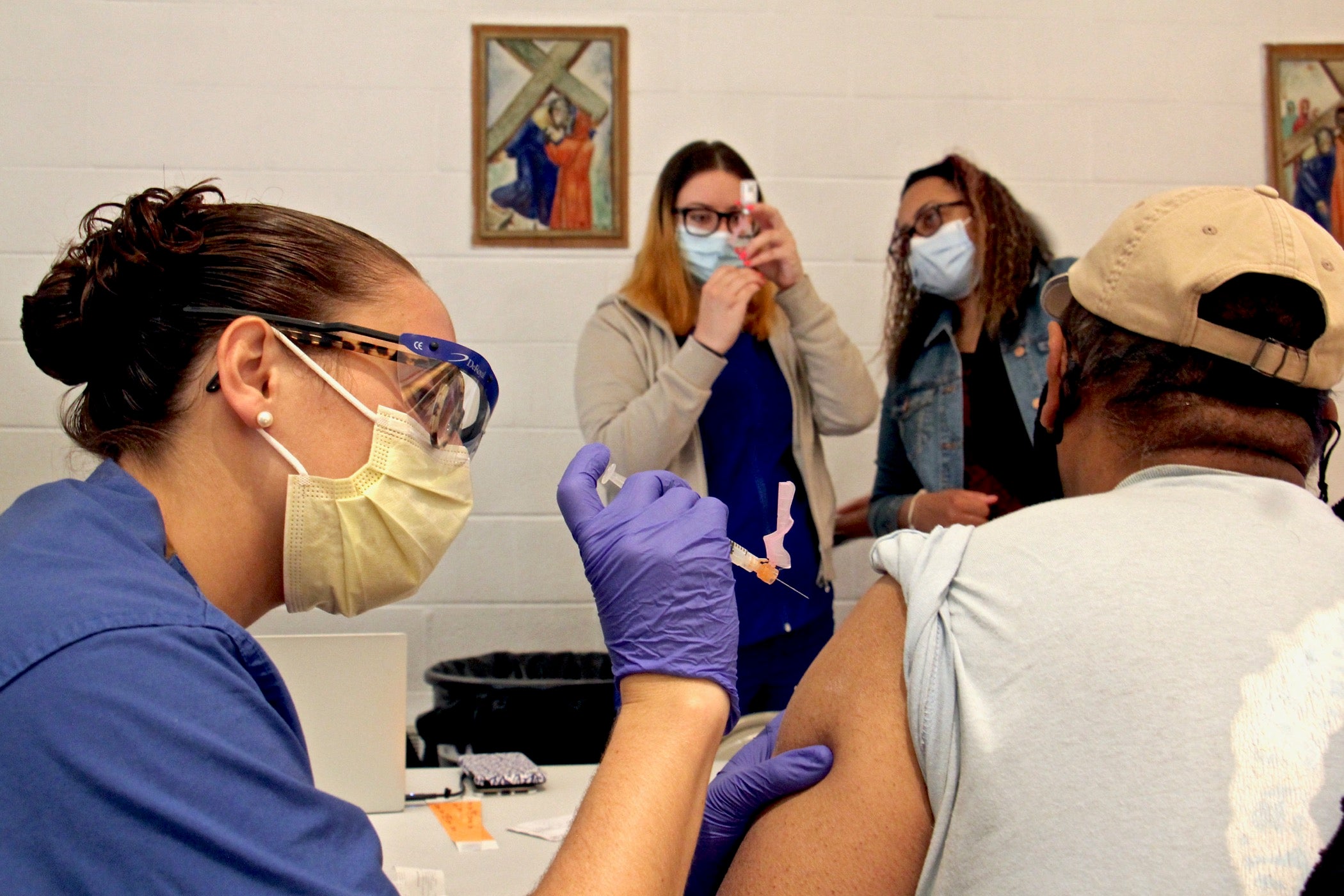
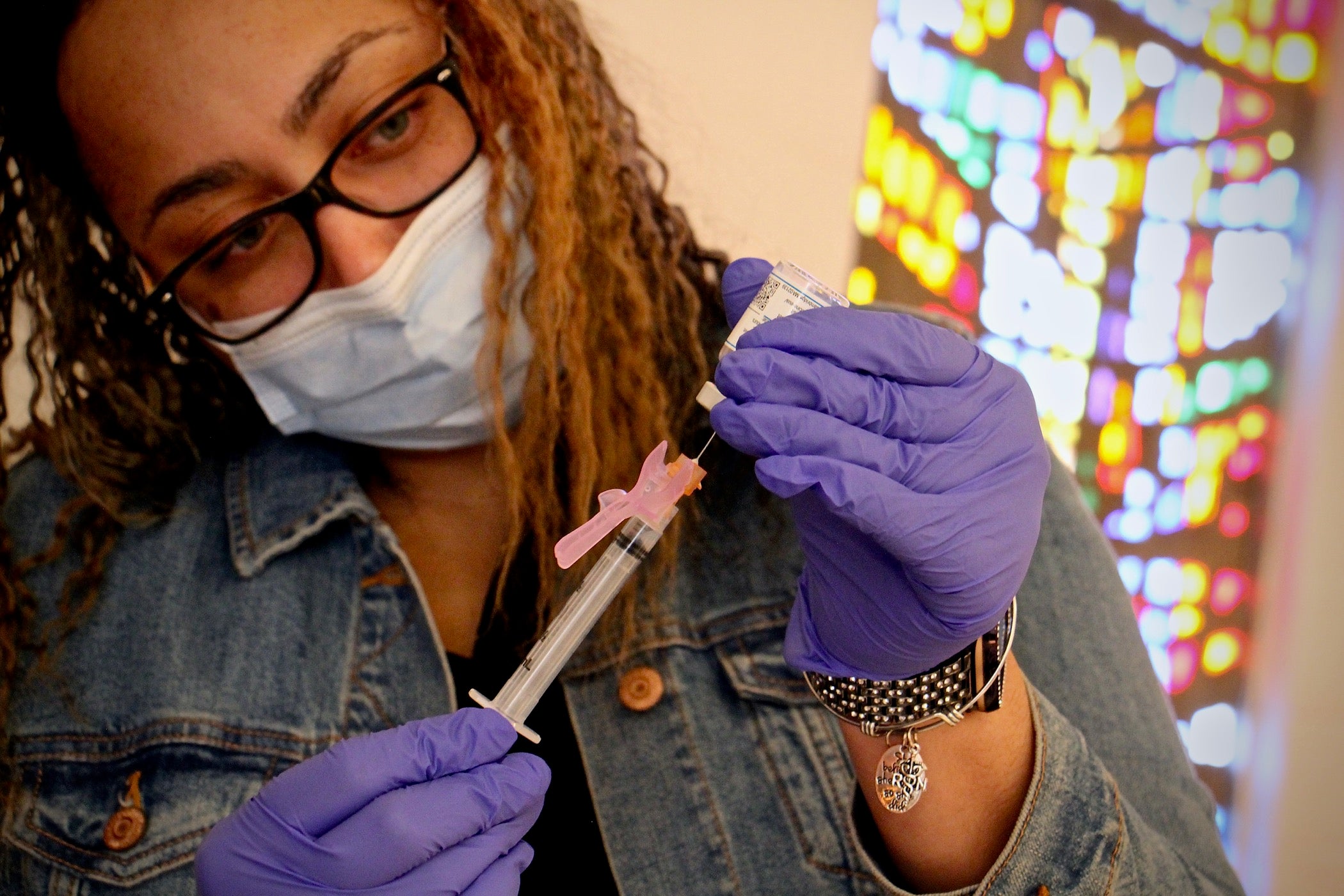
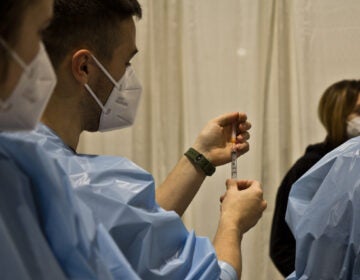
Vivian Satchell (right) receives her second dose of COVID-19 vaccine from registered nurse Elizabeth Lash during a Sayre Health vaccine clinic at Tabernacle Lutheran Church in West Philadelphia. Also pictured (from left) are Dr. Alexandra Stough and medical assistant Alexis Wright. (Emma Lee/WHYY)
Ask us about COVID-19: What questions do you have about the coronavirus and vaccines?
There are a lot of adjectives Kent Bream would use to describe the people who wait in line for vaccines each day at the Sayre Health Center in West Philadelphia: Eager. Impatient. Numerous.
Hesitant doesn’t come to mind.
“Word of mouth worked too effectively,” said Bream, medical director at the federally qualified health center in Cobbs Creek, where most residents are Black. “Wait times were increasing, we were working until two hours after closure to clear our line.”
Sayre was distributing more than 160 doses per day at its mass clinic, but with the level of vaccine demand his staff was seeing, Bream said, they could have been doling out twice that many. Calls were overwhelming the new phone lines they’d set up since COVID. Senior citizens spent up to six hours waiting.

The flooded system was not only frustrating patients, it was also putting enormous pressure on Sayre’s 30-person staff, who were regularly working after hours.
Bream took a hard look at his overworked employees and saw the threat of burnout creeping closer. So, in early March, he sat them down and had a hard conversation.
“It is not our legal responsibility to run a mass vaccination clinic,” he told them at a staff meeting. “We can choose not to do this.”
Federally qualified health centers are uniquely well positioned to vaccinate underserved communities and those most vulnerable to COVID-19. They provide primary care to millions of people across the United States, and the majority of their patients live at or below the federal poverty line. Many patients who go to these centers are uninsured, and not English-proficient. Last month, the White House announced a program to send vaccines directly to some of these health centers. In Philadelphia, Health Commissioner Thomas Farley has touted the clinics as a critical resource in vaccine distribution, and a way to even out the racial inequities in the rollout so far.
Yet on the ground, employees at federally qualified health centers in Philadelphia say the demand for vaccines in the communities they serve far outstrips the space, staffing, and overall infrastructure available to get shots in arms at scale. Vaccine operations come on top of the daily primary care they must continue to provide to high-needs patients. Even if their vaccine allotment from the city increased, it would be a struggle to keep pace.
Ultimately after talking it over, Bream and his staff made the difficult decision to scale back their mass vaccination operation. They asked the city not to advertise their site and cut back their daily doses by about half.
“We had to set limits,” Bream said. “Until we can identify additional staff or additional partnerships with the city or other organizations, we’ve had to scale back a little bit to keep everybody healthy.”
Sayre is still vaccinating about 10 people a day against COVID-19 at its primary care clinic, and 30 to 100 per day at its mobile clinic, in addition to 80 or so at the mass clinic. The center hopes additional funding and partnerships in the works could help it reach its goal of doubling its staff and scaling the mass clinic up again to meet demand. Sayre expects to get nearly $1 million in federal funding from the American Rescue Plan in the coming weeks.
Positioned for impact
Across Pennsylvania, the vaccine rollout to health centers started slowly. Clinics weren’t getting the number of doses they knew they could give out.
“For a time period, it was painful, because the pie was being sliced thinner and thinner,” said Cheri Rinehart, president and CEO of Pennsylvania Association of Community Health Centers, which represents the state’s 350 or so FQHCs.
To streamline distribution, the state Department of Health culled the number of vaccine providers, but it kept the FQHCs on the list, with an eye toward equity. Still, dose allocation was unreliable, making it hard for health centers to plan events in advance, such as large community vaccinations, or visits to senior living sites, according to Rinehart.
As of March 19, more than 320 community health centers in Pennsylvania had administered more than 70,000 vaccines across the commonwealth. That’s 2% of the state’s 2,778,953 doses administered by the same date.
Philadelphia’s 40 centers are responsible for a higher proportion of the city’s shots: In the week ending March 22, clinics gave out about 12,000, or 10% of the city’s vaccines. That share was up 3% from the week prior.
Now, increasingly, health centers are receiving their own supply of vaccines directly from the Health Resources and Services Administration. And more help is on the way: The centers are being promised funding from the American Rescue Plan. Twelve of the 40 centers in Philadelphia will receive ARP funding, including the city-operated health centers, which are slated to get more than $8 million.
Dating back to their inception, federally qualified health centers have historically played a critical role in combating health disparities among people of color and individuals living in poverty. Clinics in the United States borrow from a community-based health model from apartheid South Africa. During the civil rights movement, activists organized impromptu clinics modeled after those in South Africa as ways to help people who had been injured during protests. The centers became more formalized after a doctor pitched them to a White House agency that was part of President Lyndon B. Johnson’s War on Poverty, leading to funding for the nation’s first two experimental health centers.
During the 2009 H1N1 pandemic, federal, state, and local governments used federally qualified health centers as one key way to get that vaccine to the community. Sayre’s Bream said his health center based its mass vaccination clinic on that experience, and he wondered why federally qualified health centers weren’t used as the primary vaccine distribution sites again during the current pandemic.
“They are known by their communities and trusted by their communities,” Bream said. “More specifically, FQHCs exist to take care of vulnerable populations.”
He explained that FQHCs are already treating people who are underserved by health care and less likely to be able to quarantine safely at home due to work obligations or finances, and are thus at higher risk of being affected by infectious disease epidemics.
Why didn’t the city go with federally qualified health centers as primary vaccine sites again during this pandemic?
The vaccines for H1N1 were much easier to manage and distribute, said James Garrow, spokesperson for the Philadelphia Department of Public Health. Those vaccines did not require ultra-cold freezers, there were more of them to go around so there was no need to prioritize specific groups, and there weren’t any social distancing measures back then, Garrow said.
“Our city-run clinics have demonstrated the manpower needed to do this work, so we understand that FQHCs likely won’t be high throughput vaccine providers,” Garrow wrote in an email. “That doesn’t mean that they’re not critical to vaccinating the City.”
Staffing up to meet demand
These community health centers provide primary care, behavioral health, and often dental care year-round to low-income residents, many of whom do not have insurance and for whom English is not always their first language. Integrating vaccinations into daily operations has been no easy task for the centers, and most have had to hire entirely separate vaccination teams, a feat that takes time and resources, especially for heavily regulated federal agencies.
Public Health Management Corp., which runs a network of five FQHCs in Philadelphia, started with just 100 doses a week at first and was eager to take on more when the city offered. But its leadership recognized early on that the clinics wouldn’t be able to handle the additional supply with only existing staff members, many of whom were already working overtime.
“They had been working on nights and weekends in order to support this process,” said Judith Emmons, director of primary care at Congreso Health Center, one of PHMC’s five clinics.

So they struck a deal with a staffing agency, Aveanna Healthcare, which provides each of the health clinics with about 13 additional personnel on site. As a result, each clinic is able to distribute between 60 and 100 doses per day, sometimes more. PHMC will get $5.5 million from the American Rescue Plan for its network of clinics.
The city also increased Esperanza Health Clinic’s flow of doses early on, but the clinic couldn’t keep up, administering just a quarter of the vaccine it received. It has since managed to hire eight new staffers to help give vaccines. Still, Esperanza is only able to vaccinate a few hundred people a week. Maryanne Salib, associate director of community health and wellness at Esperanza, said adding vaccines to the existing operation is not so simple.
“It’s complicated, it’s not just like giving an MMR (measles, mumps, rubella) vaccine to a child during their well visit,” Salib said. “It requires more than that because we want to do it on such a large scale.”
That’s why Esperanza created an entirely separate vaccine team. “As much as possible, we didn’t want to add the vaccination efforts on top of what the normal health center team is doing,” Salib said.
Esperanza will receive $3 million from the American Rescue Plan in the coming weeks.
Staffing up isn’t always easy. Kirsten Britt, associate director of outreach at Sayre Health Center, said hiring temporary employees isn’t sustainable because they would need training. At the same time, she said, the health center cannot offer as much money as hospital systems can for medical staff.

“Overtime at a hospital is going to be way more than we can compete with,” Britt said. “It’s no real competition, let’s put it that way.” Sayre is slated to receive nearly $1 million from the ARP.
Yet being short-staffed takes a toll.
“Where we felt like it was starting to let up a little bit from the testing standpoint, the vaccines came into play, so it was just like from one thing to the next,” Britt said.
Britt herself lost her sister in January to COVID-19.
“People still have families, and we are still experiencing a pandemic like everyone else.”
Short on space too
When staffing is not a concern, space is. On Saturdays, Esperanza can increase the number of shots it gives out by standing up a separate vaccine clinic — but only because the building in which the clinic is set up doesn’t operate on weekends.
Philadelphia FIGHT, a FQHC that has historically focused on treating those with HIV and AIDS, has managed to scale up by partnering with existing community groups, said clinic director Jane Shull. The organization found a pharmacy partner rather than hire more staff, and has been providing vaccinations with SunRay Drugs in Kensington — the city recently announced the pharmacy is among its first round of awardees for vaccine funding. Grant amounts have not yet been announced.
Still, Shull said, those partnerships only came as a result of not having enough space. When her group wanted to offer COVID-19 tests last winter, the Center City clinic had no parking lot or other open area to set them up. So they forged relationships with Norris Square Community Alliance and with the immigrant and refugee service agency SEAMAAC — two organizations with which they now host vaccination events. With its own clinics and community events combined, Shull estimated FIGHT is administering around 700 doses per week. She anticipates she will have to hire seven staffers to ramp up vaccine administration, and more still if the city asks FQHCs to do walk-up appointments, as it has suggested.
“That will cost money because by doing by appointment, you’ve already done all the sign-up work,” said Shull. “If someone walks up and you don’t want everyone to be waiting, you’re going to have to have more staff to sign them up right then.” Luckily, Shull’s group is expecting more than $1 million in federal assistance from the ARP.
Sayre’s mass vaccination site was first located at the health center, then expanded to Tabernacle Lutheran Church a block away for more space. On April 5, the group will set up in the Sayre High School gym.
Congreso, one of PHMC’s clinics, has managed to open a separate entry point for vaccinations to avoid overcrowding at the reception desk. On a recent afternoon, Angel Santiago waited in the small lobby near the side entrance, balancing a clipboard on his lap. He gets all his primary care at Congreso, and when his doctor told him they were giving out COVID-19 shots, he jumped at the opportunity.
“They only told me about it here,” the 38-year old Santiago said in Spanish. “And there are a lot of people looking for it, so thank God.”
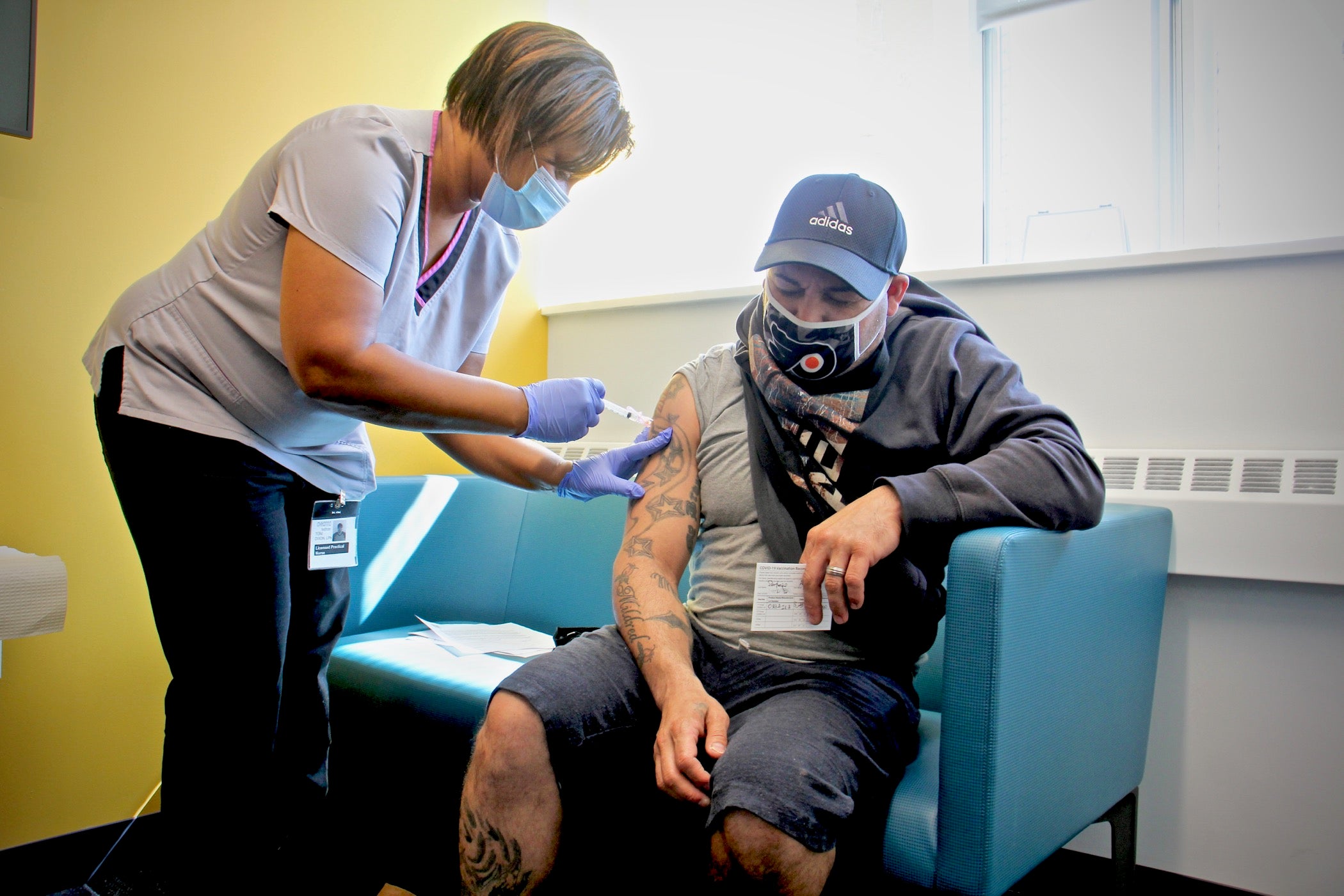
Santiago works at a warehouse in New Jersey and said he’ll be able to rest a bit easier working side by side with colleagues there. Mostly though, he’s excited because his daughter-in-law, who lives with his family, is pregnant and due in May. He’s thrilled he’ll be able to hold the baby when she comes.
Now that he knows they’re giving vaccines out at Congreso, Santiago said he planned to go home and tell his family to do what he had done.
Disclosure: The Public Health Fund, a subsidiary of Public Health Management Corp., is among WHYY’s funders.
 WHYY is one of over 20 news organizations producing Broke in Philly, a collaborative reporting project on solutions to poverty and the city’s push towards economic justice. Follow us at @BrokeInPhilly.
WHYY is one of over 20 news organizations producing Broke in Philly, a collaborative reporting project on solutions to poverty and the city’s push towards economic justice. Follow us at @BrokeInPhilly.

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)





