How do quick coronavirus tests work, and will the U.S. have enough?
Former FDA Commissioner Scott Gottlieb estimated at least 750,000 rapid point-of-care tests are needed weekly to guide the country out of the pandemic.

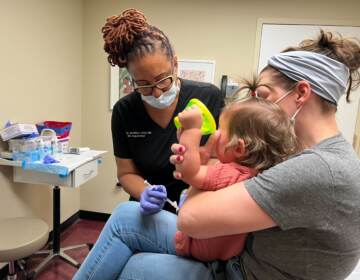
Staff in protective equipment prepare to test people at a drive-thru COVID-19 testing site. (AP Photo/Seth Wenig)
There’s wide agreement that more tests are needed for COVID-19, to track where the coronavirus is and how it is spreading — in particular, rapid tests that give results in minutes, not hours.
Last week, New Jersey Gov. Phil Murphy announced that the state had gotten 15 such tests from the federal government. These are point-of-care tests, meaning samples do not need to be sent to a lab for analysis — the same test President Donald Trump promoted in a news conference earlier this month.
Abbott, the company that makes the test, said it has shipped about 566,000 of these tests to all states. A representative for the U.S. Department of Health and Human Services said the federal government bought about 45,000 tests in the last week for state public health labs and is working directly with manufacturers.
However, a recent report from Scott Gottlieb, former commissioner of the Food and Drug Administration, estimated that at least 750,000 rapid point-of-care tests a week are needed to guide the country out of the pandemic.
Mesa Biotech is one of three companies that got emergency authorization from the FDA for a rapid point-of-care test. It adapted an existing test for the flu and RSV, a common respiratory virus, to test for the new coronavirus.
The company can make about 10,000 tests a week, and is ramping up production to make 20,000 a week by hiring more staff and adding production lines to its factory in San Diego, said Steven Sepulveda, global vice president of business development. He said Mesa has gotten around 1,500 inquiries from government institutions, hospital systems, and other potential clients asking about its test. It is serving 10 to 20 large health care systems, and there are about 500 clients waiting in line. He said the company has received inquiries from hospital systems in Philadelphia that are in progress.
Sepulveda said he has never seen interest like this in his 20 years in the biotech and diagnostics space. Based on his knowledge of the industry, he said, there is much more demand than product available at Mesa Biotech and the other two companies that make rapid point-of-care tests.
All the tests used to detect the virus itself, rather than antibodies, work similarly, said Susan Weiss, a professor of microbiology at the University of Pennsylvania who has studied coronaviruses for decades.
They use a common tool of molecular biology called a polymerase chain reaction: A health care worker takes a sample of someone’s nose or the back of the throat where the coronavirus might be, puts it in a chemical solution so that only genetic material is left, then mixes it with another tool that will bind specifically to any leftover genetic material from the coronavirus and make lots of copies of those for detection. This process takes hours in the lab, Weiss said.
How do the rapid tests speed up that process so it can be done in minutes?
Ron Collman, a virologist and pulmonary specialist at Penn, said that in a lab they will wait for a lot of tests so they can run them all together. Cepheid, the first company whose test the FDA authorized on an emergency basis, got around that by making a cartridge that can run a single test with some automated steps, so you no longer have to wait for a lot of samples to arrive, you just have to wait for the reaction, according to Collman. That shaves the time down to 45 minutes.
Abbott, the company making the quickest test, modified the testing process further so that instead of doing it in an expensive machine in a lab, health care workers can do it on a small kit that can sit in a doctor’s office or hospital or wherever a patient gets care. So now, patients don’t even have to wait for samples to get to a lab, and the test can be done in a few minutes.
Collman said scientists have made similar advances before: Thirty years ago, testing for strep throat required sending samples to a lab, and now it can be done easily in a doctor’s office.
But he added that we should still be cautious about tests because they are not 100% accurate. Sometimes, a test will come back negative even though a patient is known to have the virus. Collman said one possible way that can happen is that a patient has the virus, just not in the nose where a health care worker swabbed. The polymerase chain reaction itself should be fairly reliable, because it is done with controls: samples that are known to have the virus and samples that are known to not have the virus, so scientists can be sure the equipment works properly.
Right now, Collman said, the priority should be to test a lot more people than is currently being done in the United States, regardless of how quickly the results come back.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.





![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)