Hospital ‘super-utilizers’ disproportionately costly
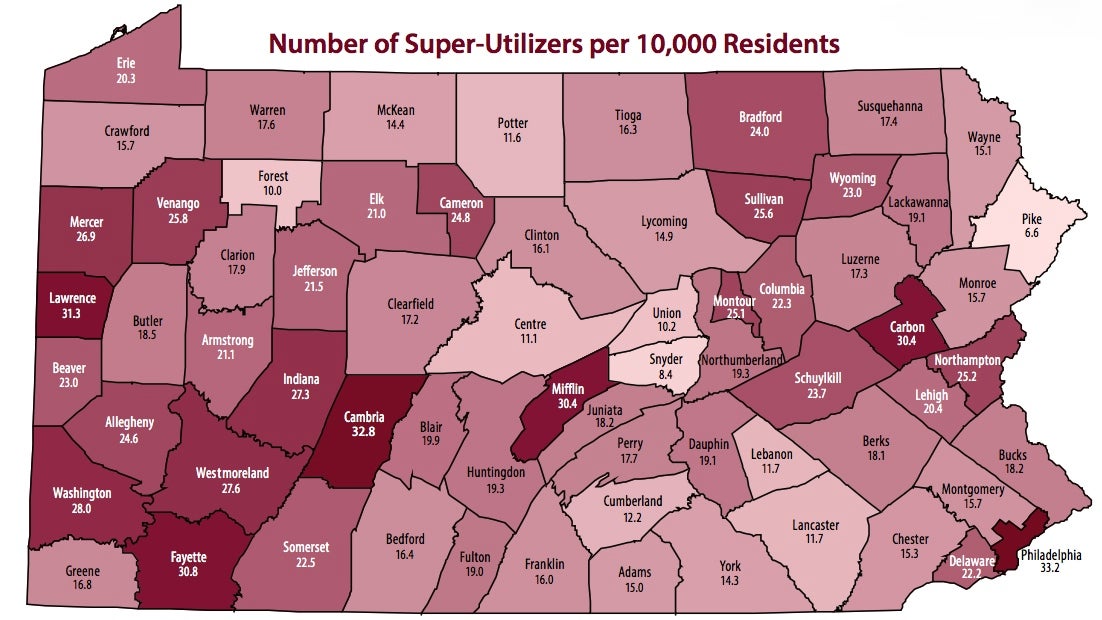
courtesy of PHC4
A report finds a small percentage of hospital patients account for a disproportionate amount of resources.
The Pennsylvania Health Care Cost Containment Council (PHC4) released a report today about “super-utilizers,” or patients who are admitted to a hospital five or more times over a year.
The report found only 3 percent of patients admitted to Pennsylvania hospitals last fiscal year are super-utilizers, but they represented 11 percent of hospital admissions and accounted for 14 percent of Medicare payments and 17 percent of Medicaid payments.
They also tended to have longer hospital stays.
Executive director Joe Martin said, “It’s a very small number of patients. But many of these patients are likely to have multiple conditions. These are very, very sick cases that require careful management.”
According to the report, Philadelphia has the highest rate of super-utilizers–33 out of every 10,000 patients. Allegheny County (home of Pittsburgh), is likewise high at 24.6 super-utilizers per 10,000, but rural counties like Mifflin and Cambria Counties have even higher rates. Martin says it’s likely about access to care.
“It’s hard to pick up a trend and that’s what’s very interesting about this information,” said Martin. “The socioeconomic issues aren’t just an urban issue, they’re also a rural issue.”
Martin says he sees a high number of super-utilizers within the Medicaid population.
In Pennsylvania, hospitals and health systems are addressing the needs of super-utilizers with programs like Lancaster General Hospital’s Care Connections, which provides access to outpatient care, human services, and home visits to repeat patients with multiple medical problems and behavioral health issues.
In a press release addressing PHC4’s report, president and CEO of The Hospital and Healthsystem Association of Pennsylvania Andy Carter affirmed that Pennsylvania hospitals are working to “address the care coordination and health and social factors that can lead to repeated emergency room visits, hospital admissions, and readmissions.”
Carter touted the importance of affordable insurance in reducing super-utilization–and with it, greater access to “routine, preventive, and primary care.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.


